Cow s Milk Allergy as a Cause of Infantile Colic:
|
|
|
- Shonda Thompson
- 6 years ago
- Views:
Transcription
1 Ausc. Puedicrtr. J. i 1917). 1.3: Cow s Milk Allergy as a Cause of Infantile Colic: Immunofluorescent Studies on Jejunal Mucosa M. J. HARRIS, MISS V. PETTY and R. PENNY3 The Prince of Wales Hospital, Randwick, and St. Vincent s Hospital and Department of Medicine, University of New South Wales Harris, M. J., Petts, Miss V. and Penny, R. (1977). Azut. Paediatr , Cow s milk allergy as a cause of infantile colic: Immunofluorescent studies on jejunal mucosa. Fourteen infants and children who had suffered frm infantile colic and related symptoms were diagnosed as beinp allergic to cow s milk because of their response to cow s milk exclusion and then to repeated challenge with cow s milk. The parents of these children frequently were allergic themselves and very frequently refused to drink cow s milk. Small bowel biopsy specimens were taken on these children. but only seven had biopsies both while taking cow s milk and when on a milk free diet. The mucosae were all histologically normal with normal disaccharidase levels. However. on immunological study it has been shown that significantly higher numbers of IgE containing plasma cells were, present in the mucosal specimens when these infants were taking cow s milk, than when they were on a milkfree diet. The diagnosis of cow s milk aller,qy remains an enigma. Clinical assessment is largely subjective, and the available laboratory tests inconclusive. The American medical literature has considered this disorder to be common, while the English literature has very scant references to cow s milk allergyand then only to the rarer manifestations. Analysis of the syndrome of cow s milk allergy has been : (i) Clinical, including wide ranging features from vomiting, colic and diarrhoea, to the potentially fatal anaphylactic shock; (ii) Histological, providing description of intestinal mucosa ; and Honorary Paediatrician, Prince of Wales Hospital. Medical Technolog.ist, Department of Immunology, St. Vincent s Hospital. Associate Professor of Medicine, Department of Immunology, St. Vincent s Hospital and Department of Medicine, University of N.S.W. First received November (iii) Immunological, depending mainly on unreliable skin testing or detection of serum antibodies. The aim of this study has be en to apply particular sophisticated laboratory techniques to substantiate the clinical claim that infantile colic can be due to cow s milk allergy. The authors are not aware that this has been done previously. This study is not a review of the role of cow s milk allergy in the aetiology of infantile colic. Because the allergic reaction takes place in the intestine, this study was designed to analyse the immunological mechanisms operative in the small bowel mucosa of children with cow s milk allergy by studying the changes in plasma cell populations during milk challenge. This study was limited to the small bowe,l mucosa of infants and children who suffered from severe infantile colic which was clinically thought due to cow s milk allergy.
2 CLINICAL MATERIAL Between January and June 1975, approximately 100 infants, M ith a tentativr diagnosis of CON S milk allerg), were seen b\ one of the authors (M.J.H. ) in consultation. The diagnosis was confirmed if the patient s symptoms resolved within 48 hours of changing to a milkfree diet, supplemented u ith Isomil hrand of soya formula. These symptoms Iecurred consistently with repeated challenge with cow s milk products as required in the criteria established by Goldman el 01. (1963). The mother was not forewarned of Mhat changes to expect. Inclusion into the series required the parents informed consent for a small bowel mucosal biopsy to be performed while the child was off and then on milk. This permission was refused in all but 14 instances and was occasionally withdrawn before the second biopsy. There was no obvious clinical difference between the subjects biopsied and those not submitted to this procedure. Fourteen children (9 males, including 2 brothers and 5 females) with cow s milk allergy diagnosed by the above criteria underwent small bowel mucosal biopsy: seven of these had repeat biopsies. STUDY PLAN When an infant with suspected cow s milk allergy responded favourably to cow s milk exclusion, he was fed on Isomil brand soya formula for two weeks and then challenged with a small dose of cow s milk. If his symptoms recurred promptly, he was given a milkfree diet again. Then he was challenged consecutively with 5 g, 10 g and 20 g lactose and also 20 g sucrose. Clinical changes after any one administration were reported immediately by the mother. A further challenge with cow s milk was carried out and finally small bowel biopsy was arranged to coincide with the third challenge of milk, usually lasting one week so as to obtain specimens on and milk. Routine investigations, such as a blood count and microscopy of urine, were performed as indicated. Isomil brand of soya formula was initially given to all the infants in the series. Generally this was found to be a highly satisfactory form of feeding; occasionally an infant did not respond well, and if the clinical diagnosis remained tenable, a further trial with Nulramigen feeding was begun and the same regime followed. Only the involved clinician (M.J.H. 1 was aware of which specimens were taken while on and off cow s milk. The key was broken only after all the results were available. Controls were obtained hy comparing the mucosal findings of the allergic children while on milk with specimens take n during the same time period on 20 children with nonspecific diarrhcea ( which excluded coeliac disease) or with failure to thrive, and also 6 children with common variable immunodeficie.ncy. These children were all drinking milk at the time. It was not felt to he ethical to do mucosal biopsies on normal, healthy infants merely to find out the changes in 1gE cell count in the mucosa when COW S milk was first introduced into the diet. METHODS Jejunal Mucosal Biopsy Jejunal mucosal biopsy was obtained b) a technique using the Watson version of the Crosby paediatric capsule described by Harris et nl ). The biopsy specimen Mas divided into three pieces lor a second piece obtained if necessary) ; one piece was assessed under the dissecting microscope, photographed, and fixed in formolsaline for routine light microscopy. The second piece uas snapfrozen in dr) ice and used in the measurement of mucosal enzyme activity. Enzyme assays were performed usinp the methods described by Dahlquist. The third piece, was snapfrczen in isopentane and dr) ice and stored at 70 C for immunofluorrscent studies. Immunofluorescent Staining Four p serial sections were cut and stained unfixed by the direct immunofluorrscent technique. Fluorescein conjugated anti IgC and IgA, anti IgM i Wellcome Pharmareuticals and anti IgE (Travenol Labs.) were used at dilutions betwreen 1 : 2 and 1 : 10. Slides were examined by epiillumination on a Keirhert Zetopan microscope. All the immunofluorescent positive plasma cells in the villi, but excludinp the, crypt, Mere counted and the result exprvswd
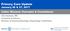
3 c_ as the averape numhei of ~dls per villus. An) abnormal staining pattern seen in the c rjfit \\as also noted. CLINICAL RESULTS The 11, children were all seen fo! the hist time hefore their hist birthdaj: 6 before 2 months of age and 10 before 6 months of age. Symptoms began early in all infants and in 12 before 4< months of ape. Thirteen infants presented w ith excessive crying or screaming, 8 with severe colic or L ~bd, and 7 with spilling and vomiting. Most slept badly and were never happy or relaxed. Four were constipated and four had frequent bowel actions; three had recent poor weight pains but none had significantly failed to thrive (Table 1). TABLE 1 Clznzcnl feattiit s of 14 batzezts wzth cow s ~tialh alleigy Screamed cxcessively I Colic Spilling or vomiting Constipation Diarrhoea Poor weight gain Always hungry One allergic parent Two allergic parents Family history of allergy 13 8 I A history of allergy in the parents occurred in over half of the seriesin both parents in 3 and in one parent in 5. Reluctance or refusal to drink cow s milk occurred in one or both parents in 9 out of 12. These latter parents were not studied to elucidate the reasons or mechanism of their milk refusal. One child had a sibling with coeliac disease. Thirteen of these infants were fed on Isomil brand of soya formula and on milkfree solids as indicated. Two children reeponded inadequately to Isomil and needed Nutramigen feeding. Sugar loading tests produced changed in the bowel function of only two of these children, one had colic with 5 g of lactose but not with 10 g and 20 g and one had loose bowels after 20 g lactose. Both of these children had normal mucosal lactase levels. LABORATORY RESULTS Five children ere biopsied before six months of age: ten before the first birthday and thc remaining 4 at various ages up to 53 years. Most repeat biopsies (5 of the 7) were done xithin three months of the fir$ and all within six months. 1. Dissecting Microscope Findings None shoved any abnormal villous structural patterns of significance no. of + ve cells/ 6 villi 10 OL 0 off milk on milk PICUHE 1: Plasma cell rontent of villi in 7 patients with COW'^ inilk allergy serially biopsied when off milk (open column) and on milk challenge (Hatched column). Histograms represent mean numbers of immunofluorescent positive plasma celld6 intestinal villi, the bars defining the standard error of the mean. 2. Light Microscopy No gross abnormalities of villous structures were seenthe relevance of this finding in relation to the clinical material is discussed below. There were minor differences in the specimens of four paired cases when challenged with milk. These changes included mononuclear infiltration of the lamina propria and/or the epithelium, with or without epithelial oedema. 3. Mueosal Enzymes No infants were found to be lactase, sucrase or isomaltase deficient. One child had low normal results for all enzymes while on milk and another had a low normal sucrase level while on milk.
4 4. Imxnunofluorescence In Figure 1, the numbei of ph5nid (.ells staining for lgg, IgA, IgNl and IgE i. compared in biopsies taken both on and off milk. This is the group of seven infants who had iepeat biopsies. There is no difference in the IgG staining in the trto groups. The IgA and IgM show a trend towards increased numbers off milk on milk (1 < ). The data of the matched and nunmatched biopsies (13 biopsies taken off milk and 8 taken on milk) are shown together in Figure 2. The results were quite similar to the matched group, although the tendency for an increase in IpM plasma cells on milk challenge was diminished. The difference in IgE staining between the two groups was again highly signifcant I P < ). No extracellular IRE ZO no. of + we cells/ 6 villi io 0 FIGURE 2: Plasma cell content of villi in all patients studied with cow s milk allergy. Hatc,hed columns represent mean rrsult when on milk challenge and open column when off milk, the bars defining the standard error of the mean. whm on milk challenge although the differences were not statistically significant by the student ttest in the number of patients analysed (IgA: P < 0.15, IgM: P < 0.2). There was, however, a significant increase in the number of IgE stained plasma ce11s after milk challenge TrlBLE I1 Absolute IgE plasma cell content of valla an seueial gvoiipa oj patzents 1 No. of I No. of IgE Patient group patients plasma cells* Cow s milk allergy on milk 13.5k2.5 Cow s milk allergy off milk I 13 1 Common variable immunodeficiency Miscellaneous I 20 I 9.5&1.5 * Average for 6 vilii&s.e. FIGURE :3: Small intestine in patient on milk challenge wcm with itiirnunofluorescrllt antiwra specific for IgE. IgE hearing plasma cdls arr prominent. was noted. Figuie 3 shoits a typical pattern seen in the intestinal biopsy Mith immunofluorescent antisera to IgE. The results of analysis of IgE plarnia cell content in the two other groups of children are shown in Table 11. All were on milk at the time of the study. The group of children with cow s milk allergy on milk had a higher IFE
5 plasma cell content in [he intestinal i illi than either group, but clue to small numbers. the differences \\ere not Significant (0.1 > P > 0 05 for I)oth groups. DISCUSSION Certain clinical sjndromes have been ascribed to COW'^ milk allerg), in which there are me,asurable changes which alter mith cow s milk exclusion. These include gastrointestinal bleeding t Wilson et al., 1964) and proteinlosing enteropathy 1 Waldman et al., 1967). In other instances there are measurable changes with strong presumptive evidence of the role of cow s milk protein, such as in failure to thrive ( Goldmari et at., 1963 j malabsorption (Kuitunen et al., 1975) and acute dehydration from diarrhoea (Freier et al., 1969). However most instances of clinical cow s milk allergy occur in patients in whom changes of symptomatology may be the only method of assessing change. The range of symptoms in infants was listed by Clein in 1954 and includes (in order of frequency) eczema, regurgitation, spilling, colic diarrhoea, unhappiness and various respiratory tract symptoms. Colic occurred as a solitary symptom in 5% of the series of Rosenblum and Rosenblum, 1952 and in that of Bigler, The series presented has concentrated on babies with colic and ~nhappiness, where the symptoms and assessments are very subjective, but the need for proof of the diagnosis remains important to the patient and his family. It is stressed that diarrhoea was not a significant feature in the past or presenting history cf these babies. Acceptance of cow s milk allergy as a cause will allow further clinical studies. Isomil brand soya formula was easily accepted by almost all infants in this series. No cases of allergy to soya formula were seen, and an inadequate response was infrequent. A trial with Nutramigen feeding was carried out and no cases were seen which did not respond to either Isomil or Nutramigen. The positive family history of allergy is not unexpected, when discussing paediatric allergic disorders, but the frequency with which these parents stated their dislike or inability to tolerate cow s milk is remarkable. The frequency of 75% in this series is in excess of the 60q1 quoted by Gerrard et al. in 1963, and one feels that thi. shouki be considered to be of diagnostic value. Ho\\ever, the mechanisms of the parents refusal to &ink co\+ s milk has not been studied. One child had a sibling with known coeliac. disease. In vieu of the familial nature of this disorder and in view of the association of cow s milk allerg) and coeliac disease in some patients (Visakorpi et al., 1967), it will be interesting to follow up this child further, even though there has been no evidence of gluten enteropathy to date. Lactase deficiency was not a feature of this series. All mucosal enzyme studies were normal and the clinical loading tests, in which the mother made assmsments of increased bowel activity or changes in temperament, were generally normal. Furthermore, none of these infants had a preceding history of acute or significant diarrhoea. Lactose tolerance tests were not done because of the age of these infants, but these may have been relevant in view of the flat curves which were reported in milk sensitivity patients who did not get diarrhoea from lactose loading (Lubos et al., 1967). Nevertheless, it would seem that cow s milk allergy and lactase deficiency are unrelated clinically and aetiologically. Histological studies have only recently been included in ieports on cow s milk allergy. It is stressed that the mucosal specimens in this series looked normal under the dissecting and the light microscope. Similar results were reported by Lubos et al., 1967, minor abnormalities by Silver and Douglas, 1968, and almost universal abnormality in the se8ries of Visakorpi, 1967, in which the patients later developed coeliac disease. It may be that the severity of symptomatology reflects the e xtent of mucosal abnormality and colic is less pathological than diarrhoea or failuretothrive. This may explain the difference between this series and that of Fontaine and Navarro, 1975, where 31 infants had vomiting and/or diarrhoea, and 26 abnormal mucosae; but there may be other differences in the case material in view of the slow return to normal of these mucosae after milk exclusion. Most early studies on cow s milk allergy utilized serum or skin testing in infants and children. As the allergic reaction takes place in the bowel, this i? a more relevant area to
6 investigate. Despite the fact that this group of patients had significantly milder symptoms and gastrointestinal pathology than in other series, immunofluorescence studies of the small bowel provided support for the involvement of immune mechanisms and helped to document the benefit from milk exclusion. In our patients a highly significant increase in the number of IgE bearing plasma cells was found in the lamina propria during milk challenge. The IgE plasma cell content is greater than in a miscellaneous control group of patients. This would strongly favour a Type 1 immediate hypersensitivity reaction to milk and supports the results of smaller series of Shiner (1975) and Kilby (1975) who, in addition, were able to show degranulation of mast cells. Iinlike their study no extracellular IgE was demonstrate,d, although this does not deny the potentially important role of IgE in cow s milk allergy. The suggestive increase in IgA bearing plasma cells in cow s milk allergy would be out of keeping with the hypothesis of Soothill, reported by Taylor et al. (1973) that infants with cow s milk allergy were relatively IgA deficient as one may expect the plasma cell content in the bowel to be also relatively deficient in IgA bearing plasma cell. By immunofluorescence, no IgA, IgM or IgG were found in the blood vessels of the lamina propria on milk challenge; this would tend to exclude antigenantibody complex reaction in intestinal mucosa. Finally, the lcwer numbers of IgE bearing plasma cells in patients receiving soya formula provides considerable immunological basis for the role of cow s milk exclusion in the management of these patients. It is felt that the significance of this series lies in the fact that babies suffering from colic and unhappinms may be allergic to cow s milk, and small bowel mucosal biopsy with appropriate immunological studies offers proof of this. Although this procedure would be hard to justify in routine investigations, it has been useful in the present study in defining changes from the normal immune status in this disease. ACKNOWLEDGEMENTS The authors would like to express their gratitude to the Department of Gastroenterology, Prince of Wales Hospital, for the enzyme assays on the mucosal biopsies and to L)r. E. de C. Baker, for the microscopic examinations. Our thanks to Abbott Lahoratories/Koss Division. for a grant to perform this project. REFERENCES BIGLER. J. A. (1955), Diarrhoea, vomiting and colic in the young infant due to milk allergy, Pediatr. Clin. North Am., 2: CLEIN, N. W. (19541, Symposium on pediatric allergy. COW S milk allergy in infants, Pediatr. Clin. North Am., 4: E ONTAINE, J. L., and NAVARRO, J. (19751, Smal! intestinal biopsy in cow s milk protein allergy in infancy, Arch. Dis. Child., 50: FREIEK, S., KLETTER, B.. and GERY, I., et al. (1969), Intolerance to milk protein, J. Pediatr., 75: GERKARD, J. W., HEINER, U. C., and IVES, E. J., et al. (19h3), Milk allergy. Recognition, natural history and management, Clin. Pediatr., 2: GOLDMAN, A. S., ANDERSON, D. W., Jr., and SELLARS, W. A,, et al. (19631, Mi!k allergy. 1. Oral challenge with milk and isolated milk proteins in allergic children, Pediatrics, 32 : HARRIS, M. J.. HARRINGTCIN, G., and BEVERIDCE, J. ( 1958), Modification to the technique for small howel biopsy in children, Am. J. Dis. Child., 115: KILBY, A., WALKERSMI.L.II, J. A., and WOOD, C. B. (1975), Small intestinal mucosa in cow s milk allergy, Lancet, 1: 531. KUITUNEN, P., VISAKORPI, J. K., and SAVILAHTI, E., et al. (19751, Malabsorption syndrome with cow s milk intolerance. Clinical findings and course in 54 cases, Arch. Dis. Child., 50: LUBOS, M. C., GERRARD, J. W., and BUCIIAN, D. J. ( 1967), Disacchardase activities in milksensitive and celiac patients, 1. Pediatr., 70: ROSENBLUM, A. H., and ROSENBLUM, P. (19521, Gastrointestinal allergy in infancy, Pediatrics, 9: SILVER, H., and DOUGLAS, D. M. (19681, Milk intolerance in infancy, Arch. Dis. Child., 43: SHINER, M., BALLARD, J., and SMITII, M. E. (1975), The sma!l intestinal mucosa in cow s milk allergy, Lancet, 1 : TAYLOR, B., NORMAN, A. P., and ORGEL, H. A., et al. (1973), Transient IgA deficiencies and pathogenesis of infantile atopy, Lancet, 2: VISAKORPI, J. K., and IMMONEN, P. (1967), Intolerance to cow s milk and wheat gluten in the primary malabsorption syndrome in infancy, Actu Paediatr. Scand., 56: WALDMANN, T. A., WOCIINER, R. D., and LASTER, L., et al. (1957), Allergic gastroenteropathy. A cause of excessive gastrointestinal protein loss, N. Engl. J. /Wed., 276: WILSON, J. F., HEINER, D. C., and LAHEY, M. E. (19641, Milk induced gastrointestinal bleeding in infants with hypochromic microcytic anemia, J. Am. Med. Assoc., 89: Correspondence to Dr. M. J. Harris, 19.3 Macquarie Street, Sydney, N.S.W
GP Patient Pathway for Infants under 1 year of age with Cows Milk Protein Allergy (Non IgE Mediated)
 GP Patient Pathway for Infants under 1 year of age with Cows Milk Protein Allergy (Non IgE Mediated) Infant suspected with (non IgE) after an allergy focused clinical history has been completed (see appendix
GP Patient Pathway for Infants under 1 year of age with Cows Milk Protein Allergy (Non IgE Mediated) Infant suspected with (non IgE) after an allergy focused clinical history has been completed (see appendix
GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE
 GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE These are the lactose intolerance guidelines and it is recommended that they are used in conjunction with the Cow s Milk Allergy guidance.
GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE These are the lactose intolerance guidelines and it is recommended that they are used in conjunction with the Cow s Milk Allergy guidance.
GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE AND PRESCRIPTION OF LOW LACTOSE INFANT FORMULA.
 GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE AND PRESCRIPTION OF LOW LACTOSE INFANT FORMULA. These are the lactose intolerance guidelines and it is recommended that they are used in
GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE AND PRESCRIPTION OF LOW LACTOSE INFANT FORMULA. These are the lactose intolerance guidelines and it is recommended that they are used in
Immunological studies in cows' milk protein-sensitive enteropathy
 Archives of Disease in Childhood, 1981, 56, 24-30 Immunological studies in cows' milk protein-sensitive enteropathy M YADAV AND N IYNGKARAN Department of Genetics and Cellular Biology, University of Malaya,
Archives of Disease in Childhood, 1981, 56, 24-30 Immunological studies in cows' milk protein-sensitive enteropathy M YADAV AND N IYNGKARAN Department of Genetics and Cellular Biology, University of Malaya,
Pediatric Food Allergies: Physician and Parent. Robert Anderson MD Rachel Anderson Syracuse, NY March 3, 2018
 Pediatric Food Allergies: Physician and Parent Robert Anderson MD Rachel Anderson Syracuse, NY March 3, 2018 Learning Objectives Identify risk factors for food allergies Identify clinical manifestations
Pediatric Food Allergies: Physician and Parent Robert Anderson MD Rachel Anderson Syracuse, NY March 3, 2018 Learning Objectives Identify risk factors for food allergies Identify clinical manifestations
COW S MILK PROTEIN ALLERGY IN CHILDREN
 COW S MILK PROTEIN ALLERGY IN CHILDREN Wednesday 8th June 2016 By Dr Rukhsana Hussain CMPA Cows' milk protein allergy is an immune-mediated allergic response to proteins in milk Milk contains casein and
COW S MILK PROTEIN ALLERGY IN CHILDREN Wednesday 8th June 2016 By Dr Rukhsana Hussain CMPA Cows' milk protein allergy is an immune-mediated allergic response to proteins in milk Milk contains casein and
Primary Care Update January 26 & 27, 2017 Celiac Disease: Concepts & Conundrums
 Primary Care Update January 26 & 27, 2017 Celiac Disease: Concepts & Conundrums Alia Hasham, MD Assistant Professor Division of Gastroenterology, Hepatology & Nutrition What is the Preferred Initial Test
Primary Care Update January 26 & 27, 2017 Celiac Disease: Concepts & Conundrums Alia Hasham, MD Assistant Professor Division of Gastroenterology, Hepatology & Nutrition What is the Preferred Initial Test
Combined cow's milk protein and gluten-induced
 Case report Combined cow's milk protein and gluten-induced enteropathy: common or rare? J WATT, J R PINCOTT, AND J T HARRIES* Gut, 1983, 24, 165-170 From The Hospitalfor Sick Children, Great Ormond.Street,
Case report Combined cow's milk protein and gluten-induced enteropathy: common or rare? J WATT, J R PINCOTT, AND J T HARRIES* Gut, 1983, 24, 165-170 From The Hospitalfor Sick Children, Great Ormond.Street,
'Every time I eat dairy foods I become ill, could I have a milk allergy.? '. Factors involved in the development of cow's milk allergy:
 'Every time I eat dairy foods I become ill, could I have a milk allergy.? '. Dairy allergy is relatively common in the community. The unpleasant symptoms some people experience after eating dairy foods
'Every time I eat dairy foods I become ill, could I have a milk allergy.? '. Dairy allergy is relatively common in the community. The unpleasant symptoms some people experience after eating dairy foods
Dietary Management of Cow s Milk Protein Allergy
 Dietary Management of Cow s Milk Protein Allergy Amy Roberts Paediatric Dietitians September 2014 Objectives To increase confidence in diagnosing a cow s milk allergy To understand the difference between
Dietary Management of Cow s Milk Protein Allergy Amy Roberts Paediatric Dietitians September 2014 Objectives To increase confidence in diagnosing a cow s milk allergy To understand the difference between
Prescribing Commissioning Policy May Diagnosis and management of Cow s Milk Protein Allergy (CMPA) and Lactose Intolerance
 Prescribing Commissioning Policy May 2018 Diagnosis and management of Cow s Milk Protein Allergy (CMPA) and Lactose Intolerance NHS Eastern Cheshire, NHS South Cheshire and NHS Vale Royal Clinical Commissioning
Prescribing Commissioning Policy May 2018 Diagnosis and management of Cow s Milk Protein Allergy (CMPA) and Lactose Intolerance NHS Eastern Cheshire, NHS South Cheshire and NHS Vale Royal Clinical Commissioning
Prescribing Guidelines for Lactose Intolerance and Cow s Milk Protein Allergy
 Prescribing Guidelines for and Aim To clarify which products and in which circumstances milk substitutes can be prescribed for babies and young children in primary care, as well as to give a guide to prescribing
Prescribing Guidelines for and Aim To clarify which products and in which circumstances milk substitutes can be prescribed for babies and young children in primary care, as well as to give a guide to prescribing
Food Allergies: Fact from Fiction
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/gi-insights/food-allergies-fact-from-fiction/3598/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/gi-insights/food-allergies-fact-from-fiction/3598/
Cow's milk protein allergy (CMPA) suspected
 Background information Patient information Key messages for this pathway When to suspect CMPA Symptoms of CMPA and assessing severity Symptoms of non IgE mediated CMPA Severe CMPA: urgent referral to paediatric
Background information Patient information Key messages for this pathway When to suspect CMPA Symptoms of CMPA and assessing severity Symptoms of non IgE mediated CMPA Severe CMPA: urgent referral to paediatric
ImuPro shows you the way to the right food for you. And your path for better health.
 Your personal ImuPro Screen + documents Sample ID: 33333 Dear, With this letter, you will receive the ImuPro result for your personal IgG food allergy test. This laboratory report contains your results
Your personal ImuPro Screen + documents Sample ID: 33333 Dear, With this letter, you will receive the ImuPro result for your personal IgG food allergy test. This laboratory report contains your results
Meredythe A. McNally, M.D. Gastroenterology Associates of Cleveland Beachwood, OH
 Meredythe A. McNally, M.D. Gastroenterology Associates of Cleveland Beachwood, OH Case in point 42 year old woman with bloating, gas, intermittent diarrhea alternating with constipation, told she has IBS
Meredythe A. McNally, M.D. Gastroenterology Associates of Cleveland Beachwood, OH Case in point 42 year old woman with bloating, gas, intermittent diarrhea alternating with constipation, told she has IBS
Diagnostic Testing Algorithms for Celiac Disease
 Diagnostic Testing Algorithms for Celiac Disease HOT TOPIC / 2018 Presenter: Melissa R. Snyder, Ph.D. Co-Director, Antibody Immunology Laboratory Department of Laboratory Medicine and Pathology, Mayo Clinic
Diagnostic Testing Algorithms for Celiac Disease HOT TOPIC / 2018 Presenter: Melissa R. Snyder, Ph.D. Co-Director, Antibody Immunology Laboratory Department of Laboratory Medicine and Pathology, Mayo Clinic
Gluten Sensitivity Fact from Myth. Disclosures OBJECTIVES 18/09/2013. Justine Turner MD PhD University of Alberta. None Relevant
 Gluten Sensitivity Fact from Myth Justine Turner MD PhD University of Alberta Disclosures None Relevant OBJECTIVES Understand the spectrum of gluten disorders Develop a diagnostic algorithm for gluten
Gluten Sensitivity Fact from Myth Justine Turner MD PhD University of Alberta Disclosures None Relevant OBJECTIVES Understand the spectrum of gluten disorders Develop a diagnostic algorithm for gluten
November Laboratory Testing for Celiac Disease. Inflammation in Celiac Disease
 November 2011 Gary Copland, MD Chair, Department of Pathology, Unity Hospital Laboratory Medical Director, AMC Crossroads Chaska and AMC Crossroads Dean Lakes Laboratory Testing for Celiac Disease Celiac
November 2011 Gary Copland, MD Chair, Department of Pathology, Unity Hospital Laboratory Medical Director, AMC Crossroads Chaska and AMC Crossroads Dean Lakes Laboratory Testing for Celiac Disease Celiac
New immunofluorescent blood test for gluten
 Archives of Disease in Childhood, 1981, 56, 864868 New immunofluorescent blood test for gluten sensitivity D J UNSWORTH, P D MANUEL, J A WALKERSMITH, C A CAMPBELL, G D JOHNSON, AND E J HOLBOROW MRC Immunology
Archives of Disease in Childhood, 1981, 56, 864868 New immunofluorescent blood test for gluten sensitivity D J UNSWORTH, P D MANUEL, J A WALKERSMITH, C A CAMPBELL, G D JOHNSON, AND E J HOLBOROW MRC Immunology
Disclosures GLUTEN RELATED DISORDERS CELIAC DISEASE UPDATE OR GLUTEN RELATED DISORDERS 6/9/2015
 Disclosures CELIAC DISEASE UPDATE OR GLUTEN RELATED DISORDERS 2015 Scientific Advisory Board: Alvine Pharmaceuticals, Alba Therapeutics, ImmunsanT Peter HR Green MD Columbia University New York, NY GLUTEN
Disclosures CELIAC DISEASE UPDATE OR GLUTEN RELATED DISORDERS 2015 Scientific Advisory Board: Alvine Pharmaceuticals, Alba Therapeutics, ImmunsanT Peter HR Green MD Columbia University New York, NY GLUTEN
See Policy CPT CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: LAB Policy No: 404 Medical Policy Committee Approved Date: 12/17; 12/18 1/1/19 Medical Officer Date APPLIES TO: All lines of business See Policy CPT CODE section below
Effective Date: 1/1/2019 Section: LAB Policy No: 404 Medical Policy Committee Approved Date: 12/17; 12/18 1/1/19 Medical Officer Date APPLIES TO: All lines of business See Policy CPT CODE section below
BIOPSY AVOIDANCE IN CHILDREN: THE EVIDENCE
 BIOPSY AVOIDANCE IN CHILDREN: THE EVIDENCE Steffen Husby Hans Christian Andersen Children s Hospital Odense University Hospital DK-5000 Odense C, Denmark Agenda Background Algorithm Symptoms HLA Antibodies
BIOPSY AVOIDANCE IN CHILDREN: THE EVIDENCE Steffen Husby Hans Christian Andersen Children s Hospital Odense University Hospital DK-5000 Odense C, Denmark Agenda Background Algorithm Symptoms HLA Antibodies
CLINICAL AUDIT. Appropriate prescribing of specialised infant formula for cows milk protein allergy
 CLINICAL AUDIT Appropriate prescribing of specialised infant formula for cows milk protein allergy Valid to December 2019 bpac nz better medicin e Background Specialised infant formulae subsidised on the
CLINICAL AUDIT Appropriate prescribing of specialised infant formula for cows milk protein allergy Valid to December 2019 bpac nz better medicin e Background Specialised infant formulae subsidised on the
Paediatric Food Allergy and Intolerance. Abigail Macleod, Associate Specialist, RBH
 Paediatric Food Allergy and Intolerance Abigail Macleod, Associate Specialist, RBH Ig E mediated food allergy Commonest cause of chronic disease in childhood up to 20% children But treatable, manageable
Paediatric Food Allergy and Intolerance Abigail Macleod, Associate Specialist, RBH Ig E mediated food allergy Commonest cause of chronic disease in childhood up to 20% children But treatable, manageable
Gliadin antibody detection in gluten
 The Ulster Medical Journal, Volume 55, No. 2, pp. 160-164, October 1986. Gliadin antibody detection in gluten enteropathy R G P Watson, S A McMillan, Clare Dolan, Cliona O'Farrelly, R J G Cuthbert, Margaret
The Ulster Medical Journal, Volume 55, No. 2, pp. 160-164, October 1986. Gliadin antibody detection in gluten enteropathy R G P Watson, S A McMillan, Clare Dolan, Cliona O'Farrelly, R J G Cuthbert, Margaret
Diagnosis Diagnostic principles Confirm diagnosis before treating
 Diagnosis 1 1 Diagnosis Diagnostic principles Confirm diagnosis before treating Diagnosis of Celiac Disease mandates a strict gluten-free diet for life following the diet is not easy QOL implications Failure
Diagnosis 1 1 Diagnosis Diagnostic principles Confirm diagnosis before treating Diagnosis of Celiac Disease mandates a strict gluten-free diet for life following the diet is not easy QOL implications Failure
Food Intolerance & Expertise SARAH KEOGH CONSULTANT DIETITIAN EATWELL FOOD & NUTRITION
 Food Intolerance & Expertise SARAH KEOGH CONSULTANT DIETITIAN EATWELL FOOD & NUTRITION Food Intolerance & Expertise What is food intolerance? Common food intolerances Why are consumers claiming more food
Food Intolerance & Expertise SARAH KEOGH CONSULTANT DIETITIAN EATWELL FOOD & NUTRITION Food Intolerance & Expertise What is food intolerance? Common food intolerances Why are consumers claiming more food
Coeliac disease. Do I have coeliac. disease? Diagnosis, monitoring & susceptibilty. Laboratory flowsheet included
 Laboratory flowsheet included I have coeliac disease. What monitoring tests should be performed? Do I have coeliac disease? Are either of our children susceptible to coeliac disease? Monitoring tests Diagnostic
Laboratory flowsheet included I have coeliac disease. What monitoring tests should be performed? Do I have coeliac disease? Are either of our children susceptible to coeliac disease? Monitoring tests Diagnostic
Malabsorption syndrome with cow's milk intolerance
 Archives of Disease in Childhood, 1975, 50, 351. Malabsorption syndrome with cow's milk intolerance Clinical findings and course in 54 cases P. KUITUNEN, J. K. VISAKORPI, E. SAVILAHTI, and P. PELKONEN
Archives of Disease in Childhood, 1975, 50, 351. Malabsorption syndrome with cow's milk intolerance Clinical findings and course in 54 cases P. KUITUNEN, J. K. VISAKORPI, E. SAVILAHTI, and P. PELKONEN
UPDATE ON SPECIALIST INFANT FEEDING GUIDELINES
 UPDATE ON SPECIALIST INFANT FEEDING GUIDELINES Miranda Potter and Lindsey Mowles Specialist Paediatric Dietitians Ipswich Hospital OUTLINE Summary of Specialist Infant Formula Prescribing guidelines Updated
UPDATE ON SPECIALIST INFANT FEEDING GUIDELINES Miranda Potter and Lindsey Mowles Specialist Paediatric Dietitians Ipswich Hospital OUTLINE Summary of Specialist Infant Formula Prescribing guidelines Updated
Pain = allergy surely true?
 Pain = allergy surely true? Dr Warren Hyer Consultant Paediatrician Consultant Paediatric Gastroenterologist Educational objectives Screamers silent reflux is this an internet diagnosis PPI s for abdominal
Pain = allergy surely true? Dr Warren Hyer Consultant Paediatrician Consultant Paediatric Gastroenterologist Educational objectives Screamers silent reflux is this an internet diagnosis PPI s for abdominal
Food Allergies on the Rise in American Children
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/hot-topics-in-allergy/food-allergies-on-the-rise-in-americanchildren/3832/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/hot-topics-in-allergy/food-allergies-on-the-rise-in-americanchildren/3832/
FPIES ANOTHER DISEASE ABOUT WHICH YOU SHOULD KNOW OBJECTIVES FPIES FPIES 11/10/2016. What is that? Robert P. Dillard, M.D.
 ANOTHER DISEASE ABOUT WHICH YOU SHOULD KNOW What is that? Robert P. Dillard, M.D. Food Protein Induced Enterocolitis Syndrome. OBJECTIVES 1: Awareness of this syndrome 2: Characteristics 3: Diagnosis 4:
ANOTHER DISEASE ABOUT WHICH YOU SHOULD KNOW What is that? Robert P. Dillard, M.D. Food Protein Induced Enterocolitis Syndrome. OBJECTIVES 1: Awareness of this syndrome 2: Characteristics 3: Diagnosis 4:
Diseases of the gastrointestinal system Dr H Awad Lecture 5: diseases of the small intestine
 Diseases of the gastrointestinal system 2018 Dr H Awad Lecture 5: diseases of the small intestine Small intestinal villi Small intestinal villi -Villi are tall, finger like mucosal projections, found
Diseases of the gastrointestinal system 2018 Dr H Awad Lecture 5: diseases of the small intestine Small intestinal villi Small intestinal villi -Villi are tall, finger like mucosal projections, found
prevalence 181 Atopy patch test, see Patch test
 Subject Index AD, see Atopic dermatitis Adrenaline, anaphylaxis management 99 101, 194, 195 Adverse food reaction definition 4 nonallergic reactions 6, 9 Allergen Nomenclature database 20, 21 Allergen
Subject Index AD, see Atopic dermatitis Adrenaline, anaphylaxis management 99 101, 194, 195 Adverse food reaction definition 4 nonallergic reactions 6, 9 Allergen Nomenclature database 20, 21 Allergen
Guideline for Prescribing Specialist Infant Formula in Primary Care For Infants With Cow s Milk Protein Allergy (CMPA) or Lactose Intolerance
 Guideline for Prescribing Specialist Infant in Primary Care For Infants With Cow s Milk Protein Allergy (CMPA) or Lactose Intolerance Date Produced: March 2013 Date for Review: March 2015 Version: 2.0
Guideline for Prescribing Specialist Infant in Primary Care For Infants With Cow s Milk Protein Allergy (CMPA) or Lactose Intolerance Date Produced: March 2013 Date for Review: March 2015 Version: 2.0
Sequoia Education Systems, Inc. 1
 Functional Medicine University s Functional Diagnostic Medicine Program Module 3 * FDMT 527C The Elimination Diet & The Modified Elimination Diet Wayne L. Sodano, D.C., D.A.B.C.I. & Ron Grisanti, D.C.,
Functional Medicine University s Functional Diagnostic Medicine Program Module 3 * FDMT 527C The Elimination Diet & The Modified Elimination Diet Wayne L. Sodano, D.C., D.A.B.C.I. & Ron Grisanti, D.C.,
Primary Prevention of Food Allergies
 Primary Prevention of Food Allergies Graham Roberts Professor & Honorary Consultant, Paediatric Allergy and Respiratory Medicine, David Hide Asthma and Allergy Research Centre, Isle of Wight & CES & HDH,
Primary Prevention of Food Allergies Graham Roberts Professor & Honorary Consultant, Paediatric Allergy and Respiratory Medicine, David Hide Asthma and Allergy Research Centre, Isle of Wight & CES & HDH,
Clinical Manifestations and Management of Food Allergy
 Clinical Manifestations and Management of Food Allergy Adrian Sie Consultant in paediatrics, Wishaw General, Lanarkshire April 2013 To do Bring Allergy plan Prevention photo Contents Is it allergy? How
Clinical Manifestations and Management of Food Allergy Adrian Sie Consultant in paediatrics, Wishaw General, Lanarkshire April 2013 To do Bring Allergy plan Prevention photo Contents Is it allergy? How
CELIAC DISEASE - GENERAL AND LABORATORY ASPECTS Prof. Xavier Bossuyt, Ph.D. Laboratory Medicine, Immunology, University Hospital Leuven, Belgium
 CELIAC DISEASE - GENERAL AND LABORATORY ASPECTS Prof. Xavier Bossuyt, Ph.D. Laboratory Medicine, Immunology, University Hospital Leuven, Belgium 5.1 Introduction Celiac disease is a chronic immune-mediated
CELIAC DISEASE - GENERAL AND LABORATORY ASPECTS Prof. Xavier Bossuyt, Ph.D. Laboratory Medicine, Immunology, University Hospital Leuven, Belgium 5.1 Introduction Celiac disease is a chronic immune-mediated
Intestinal absorption of food antigens in coeliac disease
 Archives of Disease in Childhood, 1982, 57, 462-466 Intestinal absorption of food antigens in coeliac disease ROBERT W PITCHER-WILMOTT, IAN BOOTH, JOHN HARRIES, AND ROLAND J LEVINSKY Department ofimmunology
Archives of Disease in Childhood, 1982, 57, 462-466 Intestinal absorption of food antigens in coeliac disease ROBERT W PITCHER-WILMOTT, IAN BOOTH, JOHN HARRIES, AND ROLAND J LEVINSKY Department ofimmunology
Spectrum of Gluten Disorders
 Food Intolerance:Celiac Disease and Gluten Sensitivity-A Guide for Healthy Lifestyles Ellen Karlin 2018 Spectrum of Gluten Disorders Wheat allergy - prevalence 3-8 % (up to 3 years old) Non-celiac gluten
Food Intolerance:Celiac Disease and Gluten Sensitivity-A Guide for Healthy Lifestyles Ellen Karlin 2018 Spectrum of Gluten Disorders Wheat allergy - prevalence 3-8 % (up to 3 years old) Non-celiac gluten
Gluten-Free China Gastro Q&A
 Gluten-Free China Gastro Q&A Akiko Natalie Tomonari MD akiko.tomonari@parkway.cn Gastroenterology Specialist ParkwayHealth Introduction (of myself) Born in Japan, Raised in Maryland, USA Graduated from
Gluten-Free China Gastro Q&A Akiko Natalie Tomonari MD akiko.tomonari@parkway.cn Gastroenterology Specialist ParkwayHealth Introduction (of myself) Born in Japan, Raised in Maryland, USA Graduated from
Using the Milk Ladder to re-introduce milk and dairy
 Paediatric Unit information for parents and carers Using the Ladder to re-introduce milk and dairy This leaflet explains what the Ladder is and how to use it. What is the Ladder? The Ladder is an evidence-based
Paediatric Unit information for parents and carers Using the Ladder to re-introduce milk and dairy This leaflet explains what the Ladder is and how to use it. What is the Ladder? The Ladder is an evidence-based
Understanding Food Intolerance and Food Allergy
 Understanding Food Intolerance and Food Allergy There are several different types of sensitivities or adverse reactions to foods. One type is known as a food intolerance ; an example is lactose intolerance.
Understanding Food Intolerance and Food Allergy There are several different types of sensitivities or adverse reactions to foods. One type is known as a food intolerance ; an example is lactose intolerance.
WHY IS THERE CONTROVERSY ABOUT FOOD ALLERGY AND ECZEMA. Food Allergies and Eczema: Facts and Fallacies
 Food Allergies and Eczema: Facts and Fallacies Lawrence F. Eichenfield,, M.D. Professor of Clinical Pediatrics and Medicine (Dermatology) University of California, San Diego Rady Children s s Hospital,
Food Allergies and Eczema: Facts and Fallacies Lawrence F. Eichenfield,, M.D. Professor of Clinical Pediatrics and Medicine (Dermatology) University of California, San Diego Rady Children s s Hospital,
Improving allergy outcomes. IgE and IgG 4 food serology in a Gastroenterology Practice. Jay Weiss, Ph.D and Gary Kitos, Ph.D., H.C.L.D.
 Improving allergy outcomes IgE and IgG 4 food serology in a Gastroenterology Practice Jay Weiss, Ph.D and Gary Kitos, Ph.D., H.C.L.D. IgE and IgG4 food serology in a gastroenterology practice The following
Improving allergy outcomes IgE and IgG 4 food serology in a Gastroenterology Practice Jay Weiss, Ph.D and Gary Kitos, Ph.D., H.C.L.D. IgE and IgG4 food serology in a gastroenterology practice The following
Preventing food allergy in higher risk infants: guidance for healthcare professionals
 Preventing food allergy in higher risk infants: guidance for healthcare professionals This information sheet complements current advice from the Scientific Advisory Committee on Nutrition (SACN) and the
Preventing food allergy in higher risk infants: guidance for healthcare professionals This information sheet complements current advice from the Scientific Advisory Committee on Nutrition (SACN) and the
Testing for food allergy in children and young people
 Issue date: February 2011 Understanding NICE guidance Information for people who use NHS services Testing for food allergy in children and young people NICE clinical guidelines advise the NHS on caring
Issue date: February 2011 Understanding NICE guidance Information for people who use NHS services Testing for food allergy in children and young people NICE clinical guidelines advise the NHS on caring
Milk. Allergy. Intolerance. in Infants. Advisory panel
 Milk Book Text 2/24/05 1:18 PM Page 1 & Milk Allergy Intolerance in Infants and Children Advisory panel Chairperson Professor Terry D Bolin MD(NSW), BS(Syd), FRACP, FRCP(Lond), FRCP(Edin), DCH(Lond), President,
Milk Book Text 2/24/05 1:18 PM Page 1 & Milk Allergy Intolerance in Infants and Children Advisory panel Chairperson Professor Terry D Bolin MD(NSW), BS(Syd), FRACP, FRCP(Lond), FRCP(Edin), DCH(Lond), President,
Evidence Based Guideline
 Evidence Based Guideline Serologic Diagnosis of Celiac Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: serologic_diagnosis_of_celiac_disease 4/2012 Description of Procedure
Evidence Based Guideline Serologic Diagnosis of Celiac Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: serologic_diagnosis_of_celiac_disease 4/2012 Description of Procedure
APPROACH TO FOOD ALLERGY IN CHILDREN WHY TALK ABOUT FOOD ALLERGY? DISEASES BLAMED ON FOOD ALLERGY ADVERSE REACTIONS TO FOOD OVERVIEW
 APPROACH TO FOOD ALLERGY IN CHILDREN DR MEERA THALAYASINGAM INTERNATIONAL MEDICAL UNIVERSITY RAMSAY SIME DARBY HEALTHCARE MALAYSIA APAPARI WORKSHOP PHNOM PENH CAMBODIA_ 12 TH SEPT 2015 WHY TALK ABOUT FOOD
APPROACH TO FOOD ALLERGY IN CHILDREN DR MEERA THALAYASINGAM INTERNATIONAL MEDICAL UNIVERSITY RAMSAY SIME DARBY HEALTHCARE MALAYSIA APAPARI WORKSHOP PHNOM PENH CAMBODIA_ 12 TH SEPT 2015 WHY TALK ABOUT FOOD
GI Allergy and Tolerance. Jon A. Vanderhoof, M.D. Division of Gastroenterology/Nutrition Boston Children s Hospital Harvard Medical School
 GI Allergy and Tolerance Jon A. Vanderhoof, M.D. Division of Gastroenterology/Nutrition Boston Children s Hospital Harvard Medical School Disclosure Medical Advisor- Mead Johnson Nutrition Food Allergy
GI Allergy and Tolerance Jon A. Vanderhoof, M.D. Division of Gastroenterology/Nutrition Boston Children s Hospital Harvard Medical School Disclosure Medical Advisor- Mead Johnson Nutrition Food Allergy
Dietary management of food allergy & intolerance
 Dietary management of food allergy & intolerance Dr Emilia Vassilopoulou BsC, PhD, Post-Doc Clinical Nutritionist Dietitian Food Allergy An adverse immune response to a food protein Reactions to a food
Dietary management of food allergy & intolerance Dr Emilia Vassilopoulou BsC, PhD, Post-Doc Clinical Nutritionist Dietitian Food Allergy An adverse immune response to a food protein Reactions to a food
Celiac & Gluten Sensitivity; serum
 TEST NAME: Celiac & Gluten Sensitivity (Serum) Celiac & Gluten Sensitivity; serum ANTIBODIES REFERENCE RESULT/UNIT INTERVAL NEG WEAK POS POSITIVE Tissue Transglutaminase (ttg) IgA 1420 U < 20.0 Tissue
TEST NAME: Celiac & Gluten Sensitivity (Serum) Celiac & Gluten Sensitivity; serum ANTIBODIES REFERENCE RESULT/UNIT INTERVAL NEG WEAK POS POSITIVE Tissue Transglutaminase (ttg) IgA 1420 U < 20.0 Tissue
DEAMIDATED GLIADIN PEPTIDES IN COELIAC DISEASE DIAGNOSTICS
 DEAMIDATED GLIADIN PEPTIDES IN COELIAC DISEASE DIAGNOSTICS Z. Vanickova 1, P. Kocna 1, K. Topinkova 1, M. Dvorak 2 1 Institute of Clinical Biochemistry & Laboratory Diagnostics; 2 4th Medical Department,
DEAMIDATED GLIADIN PEPTIDES IN COELIAC DISEASE DIAGNOSTICS Z. Vanickova 1, P. Kocna 1, K. Topinkova 1, M. Dvorak 2 1 Institute of Clinical Biochemistry & Laboratory Diagnostics; 2 4th Medical Department,
Does my child have a Cow s Milk Allergy?
 This factsheet has been written to help you understand and gain some advice on suspected cow s milk allergy in babies and children. Cow s milk allergy is one of the most common food allergies to affect
This factsheet has been written to help you understand and gain some advice on suspected cow s milk allergy in babies and children. Cow s milk allergy is one of the most common food allergies to affect
OHTAC Recommendation
 OHTAC Recommendation Clinical Utility of Serologic Testing for Celiac Disease in Ontario Presented to the Ontario Health Technology Advisory Committee in April and October, 2010 December 2010 Background
OHTAC Recommendation Clinical Utility of Serologic Testing for Celiac Disease in Ontario Presented to the Ontario Health Technology Advisory Committee in April and October, 2010 December 2010 Background
What should I do if I think my child needs to follow a dairy free diet?
 pg. 1 pg. 2 Feeding Children, a dairy free diet- an at home guide Children may need to follow a dairy free diet for several different reasons. They may have an allergy to the protein in cow s milk, or
pg. 1 pg. 2 Feeding Children, a dairy free diet- an at home guide Children may need to follow a dairy free diet for several different reasons. They may have an allergy to the protein in cow s milk, or
Food Allergy A buffet of truths and myths
 Food Allergy A buffet of truths and myths Toronto Anaphylaxis Education Group Adelle R. Atkinson M.D. FRCPC Associate Professor of Paediatrics University of Toronto Clinical Immunologist Division of Immunology
Food Allergy A buffet of truths and myths Toronto Anaphylaxis Education Group Adelle R. Atkinson M.D. FRCPC Associate Professor of Paediatrics University of Toronto Clinical Immunologist Division of Immunology
New Insights on Gluten Sensitivity
 New Insights on Gluten Sensitivity Sheila E. Crowe, MD, FRCPC, FACP, FACG, AGAF Department of Medicine University of California, San Diego Page 1 1 low fat diet low carb diet gluten free diet low fat diet
New Insights on Gluten Sensitivity Sheila E. Crowe, MD, FRCPC, FACP, FACG, AGAF Department of Medicine University of California, San Diego Page 1 1 low fat diet low carb diet gluten free diet low fat diet
Allergies and Intolerances Policy
 Allergies and Intolerances Policy 2016 2018 This policy should be read in conjunction with the following documents: Policy for SEND/Additional Needs Safeguarding & Child Protection Policy Keeping Children
Allergies and Intolerances Policy 2016 2018 This policy should be read in conjunction with the following documents: Policy for SEND/Additional Needs Safeguarding & Child Protection Policy Keeping Children
Diagnosis of Food Allergy by RAST
 Diagnosis of Food Allergy by RAST Donald R. Hoffman, Ph.D. Objective The purpose of this paper is to relate experience with RAST in the diagnosis of food allergy mediated by specific IgE antibodies. The
Diagnosis of Food Allergy by RAST Donald R. Hoffman, Ph.D. Objective The purpose of this paper is to relate experience with RAST in the diagnosis of food allergy mediated by specific IgE antibodies. The
Clinical Immunology and Allergy Fellowship Program Kuwait Institute for Medical Specialization
 Issued: June, 2011 Clinical Immunology and Allergy Fellowship Program Kuwait Institute for Medical Specialization I. INTRODUCTION The primary aim of the Allergy and Clinical Immunology Fellowship Program
Issued: June, 2011 Clinical Immunology and Allergy Fellowship Program Kuwait Institute for Medical Specialization I. INTRODUCTION The primary aim of the Allergy and Clinical Immunology Fellowship Program
Challenges in Celiac Disease. Adam Stein, MD Director of Nutrition Support Northwestern University Feinberg School of Medicine
 Challenges in Celiac Disease Adam Stein, MD Director of Nutrition Support Northwestern University Feinberg School of Medicine Disclosures None Overview Celiac disease Cases Celiac disease Inappropriate
Challenges in Celiac Disease Adam Stein, MD Director of Nutrition Support Northwestern University Feinberg School of Medicine Disclosures None Overview Celiac disease Cases Celiac disease Inappropriate
Gluten Free and Still Symptomatic
 How many celiac patients are affected? Gluten Free and Still Symptomatic 6.2% of all celiac patients have continuing diarrhea after 2 years on a gluten free diet 18% will develop constipation in this time
How many celiac patients are affected? Gluten Free and Still Symptomatic 6.2% of all celiac patients have continuing diarrhea after 2 years on a gluten free diet 18% will develop constipation in this time
Allergy Awareness and Management Policy
 Allergy Awareness and Management Policy Overview This policy is concerned with a whole school approach to the health care management of those members of our school community suffering from specific allergies.
Allergy Awareness and Management Policy Overview This policy is concerned with a whole school approach to the health care management of those members of our school community suffering from specific allergies.
SOY PROTEIN-ANOTHER CAUSE OF THE FLAT INTESTINAL LESION
 GASTROENTEROLOGY Copyright 1972 by The Williams & Wilkins Co. Vol. 62, No.2 Printed in U. S. A. SOY PROTEIN-ANOTHER CAUSE OF THE FLAT INTESTINAL LESION MARVIN E. AMENT, M.D., AND CYRUS E. RUBIN, M.D. Department
GASTROENTEROLOGY Copyright 1972 by The Williams & Wilkins Co. Vol. 62, No.2 Printed in U. S. A. SOY PROTEIN-ANOTHER CAUSE OF THE FLAT INTESTINAL LESION MARVIN E. AMENT, M.D., AND CYRUS E. RUBIN, M.D. Department
Hertfordshire Guidelines for Specialist Infant Feeds - CMPA - (HMMC) Feb 2015 (Updated July 2015 and June 2016)
 COWS MILK PROTEIN ALLERGY (CMPA) Symptoms and Diagnosis Refer to NICE Clinical Guideline 116 (February 2011) Food Allergy in children and young people for full details of symptoms, an allergy focused clinical
COWS MILK PROTEIN ALLERGY (CMPA) Symptoms and Diagnosis Refer to NICE Clinical Guideline 116 (February 2011) Food Allergy in children and young people for full details of symptoms, an allergy focused clinical
Activation of Innate and not Adaptive Immune system in Gluten Sensitivity
 Activation of Innate and not Adaptive Immune system in Gluten Sensitivity Update: Differential mucosal IL-17 expression in gluten sensitivity and the autoimmune enteropathy celiac disease A. Sapone, L.
Activation of Innate and not Adaptive Immune system in Gluten Sensitivity Update: Differential mucosal IL-17 expression in gluten sensitivity and the autoimmune enteropathy celiac disease A. Sapone, L.
Food Allergies Among Children -
 Food Allergies Among Children - Growth, Treatment, Prevention and a Challenge for the Food Industry Steve L. Taylor, Ph.D. Food Allergy Research & Resource Program University of Nebraska Food Navigator
Food Allergies Among Children - Growth, Treatment, Prevention and a Challenge for the Food Industry Steve L. Taylor, Ph.D. Food Allergy Research & Resource Program University of Nebraska Food Navigator
History of Food Allergies
 Grand Valley State University From the SelectedWorks of Jody L Vogelzang PhD, RDN, FAND, CHES Spring 2013 History of Food Allergies Jody L Vogelzang, PhD, RDN, FAND, CHES, Grand Valley State University
Grand Valley State University From the SelectedWorks of Jody L Vogelzang PhD, RDN, FAND, CHES Spring 2013 History of Food Allergies Jody L Vogelzang, PhD, RDN, FAND, CHES, Grand Valley State University
Is It Celiac Disease or Gluten Sensitivity?
 Is It Celiac Disease or Gluten Sensitivity? Mark T. DeMeo MD, FACG Rush University Med Center Case Study 35 y/o female Complains of diarrhea, bloating, arthralgias, and foggy mentation Cousin with celiac
Is It Celiac Disease or Gluten Sensitivity? Mark T. DeMeo MD, FACG Rush University Med Center Case Study 35 y/o female Complains of diarrhea, bloating, arthralgias, and foggy mentation Cousin with celiac
Am I a Silly Yak? Laura Zakowski, MD. No financial disclosures
 Am I a Silly Yak? Laura Zakowski, MD No financial disclosures Patient NP 21 year old male with chronic headaches for 6 years extensively evaluated and treated Acupuncturist suggests testing for celiac
Am I a Silly Yak? Laura Zakowski, MD No financial disclosures Patient NP 21 year old male with chronic headaches for 6 years extensively evaluated and treated Acupuncturist suggests testing for celiac
Cow`s Milk Protein Allergy. COW`s MILK PROTEIN ALLERGY Eyad Altamimi, MD
 Cow`s Milk Protein Allergy COW`s MILK PROTEIN ALLERGY Eyad Altamimi, MD Agenda of the talk Definitions CMPA Epidemiology and Pathogenesis CMPA Diagnosis CMPA Management CMPA prevention Adverse Food Reaction
Cow`s Milk Protein Allergy COW`s MILK PROTEIN ALLERGY Eyad Altamimi, MD Agenda of the talk Definitions CMPA Epidemiology and Pathogenesis CMPA Diagnosis CMPA Management CMPA prevention Adverse Food Reaction
screening test for coeliac disease
 Archives of Disease in Childhood, 197, 62, 469-473 Humoral response to a gliadin as serological screening test for coeliac disease J KELLY, C O'FARRELLY, J P R REES, C FEIGHERY, AND D G W WEIR Departments
Archives of Disease in Childhood, 197, 62, 469-473 Humoral response to a gliadin as serological screening test for coeliac disease J KELLY, C O'FARRELLY, J P R REES, C FEIGHERY, AND D G W WEIR Departments
Diet Isn t Working, We Need to Do Something Else
 Diet Isn t Working, We Need to Do Something Else Ciarán P Kelly, MD Celiac Center Beth Israel Deaconess Medical Center & Celiac Program Harvard Medical School Boston Gluten Free Diet (GFD) Very good but
Diet Isn t Working, We Need to Do Something Else Ciarán P Kelly, MD Celiac Center Beth Israel Deaconess Medical Center & Celiac Program Harvard Medical School Boston Gluten Free Diet (GFD) Very good but
Celiac Disease 1/13/2016. Objectives. Question 1. Understand the plethora of conditions or symptoms that require testing for Celiac Disease (CD)
 Celiac Disease MONTE E. TROUTMAN, DO, FACOI JANUARY 6, 2016 Objectives Understand the plethora of conditions or symptoms that require testing for Celiac Disease (CD) Develop a knowledge of testing needed
Celiac Disease MONTE E. TROUTMAN, DO, FACOI JANUARY 6, 2016 Objectives Understand the plethora of conditions or symptoms that require testing for Celiac Disease (CD) Develop a knowledge of testing needed
Module 5: Food Allergies and Intolerances
 A Preschool Nutrition Primer for Dietitians Module 5: Food Allergies and Intolerances Slide 1: A Preschool Nutrition Primer for Dietitians Module 5: Food Allergies and Intolerances The Nutrition Resource
A Preschool Nutrition Primer for Dietitians Module 5: Food Allergies and Intolerances Slide 1: A Preschool Nutrition Primer for Dietitians Module 5: Food Allergies and Intolerances The Nutrition Resource
Baboons Affected by Hereditary Chronic Diarrhea as a Possible Non-Human Primate Model of Celiac Disease
 Baboons Affected by Hereditary Chronic Diarrhea as a Possible Non-Human Primate Model of Celiac Disease Debby Kryszak 1, Henry McGill 2, Michelle Leland 2,, Alessio Fasano 1 1. Center for Celiac Research,
Baboons Affected by Hereditary Chronic Diarrhea as a Possible Non-Human Primate Model of Celiac Disease Debby Kryszak 1, Henry McGill 2, Michelle Leland 2,, Alessio Fasano 1 1. Center for Celiac Research,
Associate Professor Rohan Ameratunga
 Associate Professor Rohan Ameratunga Adult and Paediatric Clinical Immunologist and Allergist Auckland 9:25-9:45 Preventing Food Allergy Update on Food allergy Associate Professor Rohan Ameratunga Food
Associate Professor Rohan Ameratunga Adult and Paediatric Clinical Immunologist and Allergist Auckland 9:25-9:45 Preventing Food Allergy Update on Food allergy Associate Professor Rohan Ameratunga Food
Guidance On Prescribing Cow's Milk Free Formulae To Treat Cow's Milk Protein Allergy In Infants And Children. Uncontrolled when printed.
 NHS Grampian Guidance On Prescribing Cow's Milk Free Formulae To Treat Cow's Milk Protein Allergy In Infants And Children Co-ordinators: Consultation Group: Approver: Dietetic Prescribing NHS Grampian
NHS Grampian Guidance On Prescribing Cow's Milk Free Formulae To Treat Cow's Milk Protein Allergy In Infants And Children Co-ordinators: Consultation Group: Approver: Dietetic Prescribing NHS Grampian
Title: The effect of replacing cow s milk with soy or goat s milk in blueberry muffins on
 Amanda Kendall Written Report F&N 43 November 21, 2 Title: The effect of replacing cow s milk with soy or goat s milk in blueberry muffins on taste and texture. Abstract: Some people are cannot tolerate
Amanda Kendall Written Report F&N 43 November 21, 2 Title: The effect of replacing cow s milk with soy or goat s milk in blueberry muffins on taste and texture. Abstract: Some people are cannot tolerate
Immune mediated enteropathies. Aurora Tatu Bern 26/07/2017
 Immune mediated enteropathies Aurora Tatu Bern 26/07/2017 Definition/classification Systemic disease, mediated by antibodies, caracterised by histological changes of the small bowel Coeliac and noncoeliac
Immune mediated enteropathies Aurora Tatu Bern 26/07/2017 Definition/classification Systemic disease, mediated by antibodies, caracterised by histological changes of the small bowel Coeliac and noncoeliac
MacKillop Catholic College Allergy Awareness and Management Policy
 MacKillop Catholic College Allergy Awareness and Management Policy Overview This policy is concerned with a whole school approach to the health care management of those members of the school community
MacKillop Catholic College Allergy Awareness and Management Policy Overview This policy is concerned with a whole school approach to the health care management of those members of the school community
Celiac Disease. Etiology. Food Intolerance:Celiac Disease and Gluten Sensitivity-A Guide for Healthy Lifestyles
 Food Intolerance:Celiac Disease and Gluten Sensitivity-A Guide for Healthy Lifestyles Ellen Karlin 2017 Celiac Disease World s most common genetic food disorder Rising prevalence - over past 5 decades,
Food Intolerance:Celiac Disease and Gluten Sensitivity-A Guide for Healthy Lifestyles Ellen Karlin 2017 Celiac Disease World s most common genetic food disorder Rising prevalence - over past 5 decades,
Enquiring About Tolerance (EAT) Study. Randomised controlled trial of early introduction of allergenic foods to induce tolerance in infants
 Enquiring About Tolerance (EAT) Study Randomised controlled trial of early introduction of allergenic foods to induce tolerance in infants Final version 20/08/2012 STATISTICAL ANALYSIS PLAN FOR MAIN PAPER
Enquiring About Tolerance (EAT) Study Randomised controlled trial of early introduction of allergenic foods to induce tolerance in infants Final version 20/08/2012 STATISTICAL ANALYSIS PLAN FOR MAIN PAPER
Infants and Toddlers: Food Allergies and Food Intolerance
 Infants and Toddlers: Food Allergies and Food Intolerance A Webinar Presented by the Virginia Infant & Toddler Specialist Network and the Fairfax County Office for Children WHAT IS THE DIFFERENCE BETWEEN
Infants and Toddlers: Food Allergies and Food Intolerance A Webinar Presented by the Virginia Infant & Toddler Specialist Network and the Fairfax County Office for Children WHAT IS THE DIFFERENCE BETWEEN
Cow Milk Protein Allergy During the Rrst Year of Life : A 1 2 Year Experience at the Children's Hospital, Bangkok
 Asian Pacific Journal of Allergy and Immunology (1995) 13 : 107-111 Cow Milk Protein Allergy During the Rrst Year of Life : A 1 2 Year Experience at the Children's Hospital, Bangkok Supar Harikul 1, Yupin
Asian Pacific Journal of Allergy and Immunology (1995) 13 : 107-111 Cow Milk Protein Allergy During the Rrst Year of Life : A 1 2 Year Experience at the Children's Hospital, Bangkok Supar Harikul 1, Yupin
Name of Policy: Human Leukocyte Antigen (HLA) Testing for Celiac Disease
 Name of Policy: Human Leukocyte Antigen (HLA) Testing for Celiac Disease Policy #: 545 Latest Review Date: June 2015 Category: Laboratory Policy Grade: B Background/Definitions: As a general rule, benefits
Name of Policy: Human Leukocyte Antigen (HLA) Testing for Celiac Disease Policy #: 545 Latest Review Date: June 2015 Category: Laboratory Policy Grade: B Background/Definitions: As a general rule, benefits
Medical Conditions Policy
 Medical Conditions Policy Background: Anaphylaxis is a severe, life-threatening allergic reaction. Up to two per cent of the general population and up to 5 percent of young children (0-5yrs) are at risk.
Medical Conditions Policy Background: Anaphylaxis is a severe, life-threatening allergic reaction. Up to two per cent of the general population and up to 5 percent of young children (0-5yrs) are at risk.
HL-A8: a genetic link between dermatitis herpetiformis and gluten-sensitive enteropathy
 HL-A8: a genetic link between dermatitis herpetiformis and gluten-sensitive enteropathy Stephen I. Katz,, G. Nicholas Rogentine, Warren Strober J Clin Invest. 1972;51(11):2977-2980. https://doi.org/10.1172/jci107123.
HL-A8: a genetic link between dermatitis herpetiformis and gluten-sensitive enteropathy Stephen I. Katz,, G. Nicholas Rogentine, Warren Strober J Clin Invest. 1972;51(11):2977-2980. https://doi.org/10.1172/jci107123.
This Product May Contain Trace Amounts of Peanuts Educating Families & Patients About Food Allergies
 This Product May Contain Trace Amounts of Peanuts Educating Families & Patients About Food Allergies Kenya Beard EdD GNP-C NP-C ACNP-BC K Beard & Associates, LLC Assistant Professor Hunter College kenya@kbeardandassociates.com
This Product May Contain Trace Amounts of Peanuts Educating Families & Patients About Food Allergies Kenya Beard EdD GNP-C NP-C ACNP-BC K Beard & Associates, LLC Assistant Professor Hunter College kenya@kbeardandassociates.com
INTEGRATIVE MEDICINE
 TEST PATIENT TEST PHYSICIAN DR JOHN DOE 6DPSOH 7HVW 1DPH Sex : ) 111 CLINIC ST5((7 DDWH Collected : 00-00-0000 &/,1,& 68%85% 9,& 111 7(67 ROAD TEST SUBURB /AB,': 00000000 UR#:0000000 IgA P: 1300 688 522
TEST PATIENT TEST PHYSICIAN DR JOHN DOE 6DPSOH 7HVW 1DPH Sex : ) 111 CLINIC ST5((7 DDWH Collected : 00-00-0000 &/,1,& 68%85% 9,& 111 7(67 ROAD TEST SUBURB /AB,': 00000000 UR#:0000000 IgA P: 1300 688 522
Living with Coeliac Disease Information & Support is key
 Living with Coeliac Disease Information & Support is key Mary Twohig Chairperson Coeliac Society of Ireland What is Coeliac Disease? LIVING WITH COELIAC DISEASE Fact Not Fad Auto immune disease - the body
Living with Coeliac Disease Information & Support is key Mary Twohig Chairperson Coeliac Society of Ireland What is Coeliac Disease? LIVING WITH COELIAC DISEASE Fact Not Fad Auto immune disease - the body
Not elevated 71. Elevated 14. Highly elevated out of 90 tested allergens were elevated or highly elevated
 Sample ID: Test101 Dear Your Name, This ImuPro laboratory report contains your personalized food allergy test results and recommendations for your path to wellness. Your blood has been analyzed for the
Sample ID: Test101 Dear Your Name, This ImuPro laboratory report contains your personalized food allergy test results and recommendations for your path to wellness. Your blood has been analyzed for the
The first and only fully-automated, random access, multiplex solution for Celiac IgA and Celiac IgG autoantibody testing.
 Bio-Rad Laboratories bioplex 2200 SYSTEM BioPlex 2200 Celiac IgA and IgG Kits * The first and only fully-automated, random access, multiplex solution for Celiac IgA and Celiac IgG autoantibody testing.
Bio-Rad Laboratories bioplex 2200 SYSTEM BioPlex 2200 Celiac IgA and IgG Kits * The first and only fully-automated, random access, multiplex solution for Celiac IgA and Celiac IgG autoantibody testing.
FOOD ALLERGY IN SOUTH AFRICA Mike Levin
 FOOD ALLERGY IN SOUTH AFRICA Mike Levin Michael.levin@uct.ac.za SAFFA: The South African Food sensitisation and Food Allergy study Botha M, Basera W, Gray C, Facey-Thomas H, Levin ME. The Prevalence of
FOOD ALLERGY IN SOUTH AFRICA Mike Levin Michael.levin@uct.ac.za SAFFA: The South African Food sensitisation and Food Allergy study Botha M, Basera W, Gray C, Facey-Thomas H, Levin ME. The Prevalence of
Beth Strong, RN, FNP-C The Jaffe Food Allergy Institute Mount Sinai School of Medicine New York 2/23/13
 Beth Strong, RN, FNP-C The Jaffe Food Allergy Institute Mount Sinai School of Medicine New York 2/23/13 I do not have any financial disclosure to report Why Challenge? To confirm that the suspected food
Beth Strong, RN, FNP-C The Jaffe Food Allergy Institute Mount Sinai School of Medicine New York 2/23/13 I do not have any financial disclosure to report Why Challenge? To confirm that the suspected food
