Kari C. Nadeau, MD, PhD Division of Allergy, Immunology, and Rheumatology at Stanford
|
|
|
- Garry Owen
- 6 years ago
- Views:
Transcription
1 Kari C. Nadeau, MD, PhD Division of Allergy, Immunology, and Rheumatology at Stanford
2 Describe the pathophysiology, initial evaluation & management of patients with food allergy including gastrointestinal food allergy, oral allergy syndrome and type I food allergy Identify recent advances in the field of food allergy and have some familiarity with published guidelines for managing food allergy Outline current and emerging treatment modalities for food allergic patients
3 Nothing to disclose
4 ID: 9.5 y.o. male with a history of severe food allergies, eczema, and asthma CC: Presents to PICU with hypoxic brain injury due to anaphylaxis from cow s milk ingestion Transferred to PICU from outside hospital after multiple failed resuscitations over a 3 hr period
5 On the evening of , patient accidentally drank from his sister s cup of cow s milk on the way to bed. He immediately developed emesis and became SOB; parents gave Epipen jr. to his thigh and called 911 Paramedics arrived in minutes On the scene, intubation was attempted but difficult Duration of code=1 hr. CT scan showed hypoxic injury and right uncal herniation.
6 In 2001, he presented to LPCH AAI clinic and had severe eczema and asthma. RAST tests were performed at 2001 and showed IgE > 2000, Milk> 100, Peanut>100, Egg 40.3, Soy 17.9, Wheat 20.2, Corn 26.3, Oat No known allergies to beef. He had had one prior visit to the ER for milk ingestion in He presented with hyperventilation and emesis. He was given benadryl and his symptoms improved. He was hospitalized three times in the first year of life for asthma; no intubations but did need steroids
7 Patient and family were prescribed an Epipen jr. and taught about anaphylaxis precautions Patient then began to receive care at private AI facility and was recommended 9 months prior to event to repeat RAST testing. This was not done. Over the past couple of months prior to event, parents decided to allow him to eat wheat, corn, oat, and egg products since he did not seem to have any symptoms from these foods.
8 Background Definition Clinical signs and symptoms Natural History Cow s milk, hen s egg, soy, peanut, tree nuts Diagnostic work-up Treatment Research studies and FAQs
9 Prevalence ~4% - Peanuts 3 million allergic in U.S. (~1.1%) Branum 2009 Pediatrics 124: Most common cause of visits for pediatric anaphylaxis treated in U.S. Emergency Rooms > 15% of patients/year have accidental reactions Yu 2006 J Allergy Clinical Immunology 118:
10 deaths/year reported from food allergies - Bock SA J Allergy Clinical Immunology 2001: 107 (1):
11 Food culprits (n=79) Peanut 56% Tree nut 24% Fish/shellfish 8% Milk 9% Wheat 1% Unknown 3% Mixed nuts, baked goods, cookies, candies, Ethnic food, buffets, sauces, cross-contamination Bock S.A. AAAAI meeting 2009
12 Adolescents Nut Allergy Known food allergy History of Anaphylaxis Asthma, especially those with poor control Lack of skin symptoms Denial of symptoms Concomitant intake of alcohol (which may increase absorption of food) Belief that antihistamines alone were sufficient to treat symptoms Delay or lack of administration of epinephrine However even timely injections of epinephrine do not necessarily prevent death (4 of 32 cases) Bock SA J Allergy Clinical Immunology 2001: 107 (1):
13 Can occur in minutes Due to upper or lower respiratory compromise or cardiovascular collapse Pumphrey et al. Clin Exp Allergy 30 (2000):
14 Adverse health effect arising from a specific immune response that occurs reproducibly on exposure to a given food. National Institute of Allergy and Infectious Diseases (NIAID ) Guidelines for the Diagnosis and Management of Food Allergy 2010
15 National Institute of Allergy and Infectious Diseases (NIAID ) Guidelines for the Diagnosis and Management of Food Allergy 2010
16 Signs and symptoms Percentage of cases Cutaneous >90 Urticaria and angioedema Flush Pruritus without rash 2 5 Respiratory Dyspnea, wheeze Upper airway angioedema Rhinitis Dizziness, syncope, hypotension Abdominal Nausea, vomiting, diarrhea, cramping pain Miscellaneous Headache 5 8 Substernal pain 4 6 Seizure 1 2
17 Over 170 foods have been reported to cause IgE-mediated reactions However over 90% of food allergies are caused by the following foods Milk Hen s egg Soy Wheat Peanut Tree Nuts Shellfish Fish National Institute of Allergy and Infectious Diseases (NIAID ) Guidelines for the Diagnosis and Management of Food Allergy 2010
18 Children with food allergy*: 35-71% atopic dermatitis Possible that peanut sensitization is associated with atopic dermatitis, use of peanut oil containing skin preparations, and household consumption of peanut** 33-40% allergic rhinitis 34-39% asthma * Sicherer et al. J of Allergy and Clin Immunology 2001: 108: ** Fox et al. J of Allergy and Clin Immunology 2009: 123 (2):
19 Oral pruritus, rapid onset, IgE-mediated, rarely progressive Usually fresh fruits and vegetables Heat labile: cooked forms, no reaction Cause: cross reactive proteins pollen/food Birch Ragweed Grass Pollen Apple, apricot, carrot, cherry, kiwi, plum Banana, cucumber, melon, watermelon Cherry, peach, potato, tomato Foods
20 Non-IgE-mediated, typically milk and soy induced Spectrum may include colic, constipation and occult GI blood loss Enterocolitis Enteropathy Proctitis Age Onset: Infant Infant/Toddler Newborn Duration: mo mo 9 mo-12 mo Characteristics: Failure to thrive Malabsorption Bloody stools Shock Villous atrophy Lethargy Eosinophilic Diarrhea Self limited Vomiting
21 Celiac Disease (Gluten-sensitive enteropathy) Anti-gliadin IgG, anti-endomysial IgG, IgA Villus atrophy, malabsorption, pain, associated CA Eosinophilic esophagitis, gastritis, gastroenteritis Eosinophilic infiltration Poor growth, pain, vomit, diarrhea, reflux Multiple food allergy, IgE and non-ige-mediated May affect varying regions of gut Gastrointestinal Anaphylaxis Acute vomit/diarrhea, IgE-mediated
22 Migraines Behavioral / Developmental disorders Arthritis Seizures Inflammatory bowel disease
23 Condition Symptoms Mechanism Lactose intolerance Fructose intolerance Pancreatic insufficiency Gallbladder/liver disease Food poisoning Scombroid fish poisoning Caffeine Tyramine Auriculotemporal syndrome (Frey syndrome) Gustatory rhinitis Panic disorder What is not a food allergy? Bloating, abdominal pain, diarrhea (dose-dependent) Bloating, abdominal pain, diarrhea (dose-dependent) Malabsorption Malabsorption Pain, fever, nausea, emesis, diarrhea Flushing, angioedema, hives, abdominal pain Tremors, cramps, diarrhea Migraine Facial flush in trigeminal nerve distribution associated with spicy foods Profuse watery rhinorrhea associated with spicy foods Subjective reactions, fainting upon smelling or seeing the food Lactase deficiency Fructase deficiency Deficiency of pancreatic enzymes Deficiency of liver enzymes Bacterial toxins in food In spoiled fish histidine is metabolized to histamine Pharmacologic effects of caffeine in susceptible individuals Pharmacologic effects of tyramine in susceptible individuals Neurogenic reflex, frequently associated with birth trauma to trigeminal nerve (forceps delivery) Neurogenic reflex Psychologic
24 Most children will outgrow cow s milk, egg, and wheat allergy Far fewer will outgrow peanut and tree nut allergy A high initial specific IgE against the food is associated with a lower rate of resolution of clinical allergy over time Atopic dermatitis resolution is a useful marker for onset of tolerance to food allergens Skin tests to a food can remain positive long after tolerance to a food has developed. Nevertheless, reduction in the size of the skin test wheal may be a marker for the onset of tolerance to the food allergen. National Institute of Allergy and Infectious Diseases (NIAID ) Guidelines for the Diagnosis and Management of Food Allergy 2010
25 First foreign protein introduced into infant s diet Most common food allergy in young children 2.5% of children in first two years of life 1.1% is IgE-mediated Minimal threshold dose to cause allergic reaction as low as 0.02 ml of milk (e.g. drops)
26 Cross-reactivity with cows, goat, and sheep milk secondary to homology between these proteins 90% children allergic to cow s milk will be reactive to goat s milk on oral food challenge 75% of cow s milk allergic children will tolerate extensively heated cow s milk (e.g. baked goods)
27 1-2% children Yolk considered less allergenic than white Egg white has 23 glycoproteins 70% egg allergic children may be able to ingest small amounts of egg protein in extensively heated (baked) products
28 0.4% children Belongs to legume family with peanut 88% have concomitant peanut allergy
29 1.1% Most common food allergy in pediatric population beyond 4 years of age Most likely to cause fatalities 21.5% chance of outgrowing peanut allergy 8% risk of recurrence
30 0.6% population allergic Walnuts 34% Cashews 20% Almonds 15% Pecan 9% Pistachio 7% Hazelnut, Brazil nut, Pine Nut, Macadamia nut < 5%
31 In recent study, 12% patients allergic to more than 1 tree nut Approximately 30-50% of peanut allergic patients have at least one tree nut allergy Approximately 9% outgrow tree nut allergy Note 14/19 patients who never ingested tree nuts but had elevated specific IgE passed the oral food challenge Of these 14 patients, 58% with specific IgE 5 passed the oral food challenge while 63% with specific IgE 2 passed the oral food challenge Fleischer DM. J Allergy Clin Immunol. 2005;116(5):
32 The severity of a reaction cannot be accurately predicted by the degree of severity of past reactions and depends on: Amount ingested Food form (cooked, raw, or processed) Co-ingestion of other foods The severity also may be influenced by The age of the patient The degree of sensitization at the time of ingestion The rapidity of absorption, based on whether The food is taken on an empty stomach The ingestion is associated with exercise The patient has other co-morbid conditions (e.g., asthma or AD )
33 1% to 20% Typically occur 8 hours after initial reaction, but up to 72 hours later Up to 25% of fatal or near-fatal food reactions There is no consensus on optimal observation time following the initial reaction; recommendations range from 4 to 24 h Minimum 4 hour observation Studies suggest that delayed administration, inadequate dosing, or a need for large doses of epinephrine are risk factors for biphasic reactions Also failure to administer corticosteroids also seems to predispose towards biphasic reaction
34 *Results from ImmunoCAP testing are not comparable to IgE levels from other assay systems such as Immunolite and Turbo-MP. Must know assay lab using. ImmunoCAP Allergy blood tests* Generally felt to be less sensitive than SPT Allergen ku A /L PPV [+] Egg 7 98 Infants 2 yr [ ] 2 95 Milk Infants 1 [ ] 5 95 Peanut Fish Soybean Wheat Tree nuts [ ] 15 95
35
36 Airway, Breathing, Circulation Vital signs EpiPen Concurrently, call 911 Supine position with legs elevated (unless respiratory compromise or vomiting) Supplemental O2 Optimize organ perfusion and bronchodilates IVF Weight estimation for dosing of medications
37 What are the indications to give Epinephrine? Severe reaction Respiratory distress Swollen throat Loss of Consciousness
38 Seconds but is rapidly metabolized Effect often short-lived and repeat doses may be necessary for severe or protracted anaphylaxis (within 1-2 minutes if first one is not working)
39 10-20% of anaphylactic cases required 2 nd Epipen injection Jarvinen et al. J Allergy Clin Immunology 2008; 122:
40 Second line treatment only Not life-saving Only relieve itching and urticaria Do not relieve stridor, shortness of breath, wheezing, GI symptoms, or shock Onset of action minutes H1 and H2 antagonism superior to H1 alone
41 National Institute of Allergy and Infectious Diseases (NIAID ) Guidelines for the Diagnosis and Management of Food Allergy 2010
42 Prolonged observation is mandated At least 8-24 hours after symptoms have resolved Moderate to severe reaction Asthmatic wheezing Ingested antigen with risk of systemic absorption Previous history of biphasic response
43 Strict Avoidance of Allergenic Foods Regular growth monitoring Nutritionist Possibly decreases risk of malnutrition (e.g. Ca, Vit D) Christie et al. J Am Diet Assoc 2002; 102(11): Education on how to read labels Only 7%, 22%, and 54% of parents correctly identified labeled products containing milk, egg, and peanut respectively Joshi et al. J Allergy Clin Immunol 109(6): Food Allergen Labeling and Consumer Protection Act (FALCA) effective 2006 mandates manufacturer disclosure of the most common allergens (milk, egg, wheat, soy, peanut, tree nuts, fish, and crustacean shellfish) in plain English in the ingredient list or in a separate contains statement 17% of 20,214 products contain advisory labels Pieretti, J Allergy Clin Immunol 2009;124:337-41
44 Strict Avoidance of Allergenic Foods Nutritionist Education on how to read labels Food allergic patients assume incorrectly that terms such as shared equipment, shared facility, or may contain indicate different levels of risk. Avoid products that state may contain or manufactured on equipment 5-17% risk of significant amount of allergen in food 1.9% without declaration of allergen contained allergen - Remington et al. J Allergy Clin Immunol 2010;125 (2): AB218 - Ford et al. J Allergy Clin Immunol 2009; 123 (2): S176
45 Even when patients ask about ingredient information they may receive inaccurate information If symptoms start assume allergic reaction, call for help Bock S.A. Academy of Allergy Asthma and Immunology Annual meeting 2009
46 Food Allergy and Anaphylaxis Network ( Newsletter Website with patient handouts, educational videos and children s books
47
48
49
50
51
52
53
54 Epinephrine 1 st line treatment Life-saving Majority of patients who have prescription do not carry Epinephrine Even those who carry the Epinephrine do not administer the medication when clinically indicated Only 3% of patients who died of food anaphylaxis had Epineprhine Bock et al. J Allergy Clin Immunol 2001;107:191-3 Only 21% of families demonstrate proper use Sicherer, et al. Pediatrics 105 (2000), pp
55
56 Must demonstrate how to use it Have families practice Watch Training Video (EpiPen or TwinJect)
57 While administering epinephrine, call 911 Delayed administration of epinephrine has contributed to fatalities Give Epinephrine immediately, but at least within 30 minutes, of food allergic reaction Sampson et al. Engl J Med (6): All other medications, including antihistamines and corticosteroids considered adjunctive Antihistamine use most common reason cited for not using Epinephrine and may significantly increase risk of life-threatening reaction Simons et al. J Allergy Clin Immunol 2009;124:301-6
58 Liquid Zyrtec or Benadryl at all times Prefilled teaspoons are easy to transport and readily available over the counter
59 Medicalert.org laurenshope.com Inscription example: Patient s name. Allergic to peanuts, tree nuts + Asthma. Give EpiPen and call 911. Mother or father: cell phone number.
60 MMR and Varicella and influenza grown in chicken-embryo fibroblast culture and contains minimal amounts of egg protein Can be administered safely in egg-allergic patients, even those with a severe h/o allergic reaction if skin test is negative National Institute of Allergy and Infectious Diseases (NIAID ) Guidelines for the Diagnosis and Management of Food Allergy 2010
61 History: symptoms, timing, reproducibility Acute reactions vs chronic disease Diet details / symptom diary Specific causal food(s) Hidden ingredient(s) Physical examination: evaluate disease severity Identify general mechanism Allergy vs intolerance IgE versus non-ige mediated
62 Suspect IgE-mediated Prick skin tests (fresh extract if oral allergy) RAST Suspect non-ige-mediated Consider biopsy of gut, skin Suspect non-allergic, consider: Breath hydrogen Sweat test Endoscopy
63 Positive prick test or RAST Indicates presence of IgE antibody NOT clinical reactivity Negative prick test or RAST Essentially excludes IgE antibody (>95%) ID skin test with food Risk of systemic reaction & not predictive Contraindicated Unproven/experimental tests Provocation/neutralization, cytotoxic tests, applied kinesiology, hair analysis, IgG4
64 Recommended Interpretation of Food Allergen-Specific IgE levels (ku/l) Egg Milk Peanut Fish Soy Wheat Reactive if > Possibly reactive (physician challenge) Unlikely reactive if < (home challenge) * Sampson, H. Utility of food specific IgE in predicting symptomatic food allergy. JACI
65 Elimination diets (1 to 6 weeks) Eliminate suspected food(s), or Prescribe limited eat only diet, or Elemental diet Oral challenge testing (MD supervised, ER meds available) Open Single-blind Double-blind, placebo-controlled (DBPCFC)
66 Test for specific-ige antibody Negative: reintroduce food* Positive: start elimination diet Elimination diet No resolution: reintroduce food* Resolution Open / single-blind challenges to screen DBPCFC for equivocal open challenges * Unless convincing history warrants supervised challenge
67 Includes disease with unknown mechanisms Food additive allergy Elimination diets (may need elemental diet) Oral Challenges Timing/dose/approach individualized for disorder Enterocolitis syndrome can elicit shock Enteropathy / eosinophilic gastroenteritis may need prolonged feedings to develop symptoms DBPCFCs preferred May require ancillary testing (endoscopy / biopsy)
68 If Specific IgE to a food > 25 ku/l., low likelihood of losing allergy Component Diagnostic Testing and Epitope Arrays are moving forward to further our knowledge and diagnostics capabilities There are no reliable predictors to determine whose food allergy will persist There are no reliable predictors to determine whose food allergy will lead to severe anaphylaxis (predicted in 50% of cases of food allergy) The gold standard to identify an offending food allergen is a double blind, placebo-controlled in vivo challenge which requires hospitalization, is costly, lengthy and can result in an anaphylactic shock Once the tests occur, there are many false positives that can lead to elimination diets in children associated with malnutrition (NY Times.2009)
69 Epitope Arrays : Development of a novel peptide microarray for large-scale epitope mapping of food allergens Serum dilution experiment (A) and peptide inhibition assay (B). Areas showing non-specific binding are indicated with black arrows. Targeted peptides, which are the peptides pre-incubated with the serum pool are indicated with red arrows for each inhibition group. Areas with possible crossinhibition based on sequence alignment are indicated with blue arrows. J Allergy Clin Immunol Aug;124(2): Lin J, et al.
70 New Diagnostic Allergy Test based on rapid assessment of blood basophil activation Stimulated by Antigen Unstimulated Expression of molecules on the cell surface (expressed by cytoplasmic compartments) for example CD203c or CD63
71 New Diagnostic Allergy Test Based on rapid assessment of blood basophil activation Non Activated-diluent Activated-allergen 20 minutes incubation Spin 300 x g 0 Breaks Plasma Leukocytes Gradient Antibodies 1. Anti-CD203c 2. Anti-CD63 3. Anti-CD HLA-DR Abs Staining RBC TIME To RESULT: ~ 1 HOUR Abs diluted in 1% BSA 0.05% NaN3 in PBS Wash, and Flow Cytometry Responses to multiple allergens can be tested at the same time (to assess which are most important in that patient) Results available within 1 hour Use the finger stick test to determine who can tolerate their next dose of food oral immunotherapy
72 Our Diagnostic Allergy Test Can Detect Allergic vs. Non-allergic Patients Non Activated basophils CD203c (MFI) Activated basophils Modified Bock's Reaction Grade A r 2 = Peanut allergic CD203c MFI Controls Modified Bock's Reaction Grade B r 2 = CD63 MFI
73 Hidden ingredients (peanut in sauces or egg rolls) Labeling issues ( spices, changes, errors) Cross contamination (shared equipment) Code words ( Natural flavor may be CMP) Seeking assistance Registered dietitian: ( Food Allergy Network ( )
74 Artificial butter flavor, butter, butter fat, buttermilk, casein, caseinates (sodium, calcium, etc.), cheese, cream, cottage cheese, curds, custard, Half&Half, hydrolysates (casein, milk, whey), lactalbumin, lactose, milk (derivatives, protein, solids, malted, condensed, evaporated, dry, whole, low-fat, non-fat, skim), nougat, pudding, rennet casein, sour cream, sour cream solids, sour milk solids, whey (delactosed, demineralized, protein concentrate), yogurt. MAY contain milk: brown sugar flavoring, natural flavoring, chocolate, caramel flavoring, high protein flour, margarine. * It is common to have a reaction to a hidden ingredient to rather than to have an allergic reaction to a previously tolerated food.
75 Soy (confirm soy IgE negative) <15% soy allergy among IgE-CMA ~50% soy allergy among non-ige CMA Cow s milk protein hydrolysates >90% tolerance in IgE-CMA Partial hydrolysates Not hypoallergenic! (ex/ Nutramigen) Elemental amino acid-based formulas Lack allergenicity (ex/ Neocate) * CMA=cow s milk allergy
76 Epinephrine: drug of choice for reactions Self-administered epinephrine readily available Train patients: indications/technique Antihistamines: secondary therapy Emergency plan in writing Schools, spouses, caregivers, mature sibs / friends Emergency identification bracelet
77 Re-evaluate for tolerance periodically Interval and decision to re-challenge: Type of food allergy Severity of previous symptoms Allergen Ancillary testing Skin prick test/rast may remain positive Reduced concentration food specific-ige encouraging
78 Aimed at high risk newborn Positive family history: biparental or parent / sib Breast feeding generally protective of allergy Wean / supplement with extensively hydrolyzed hypoallergenic protein hydrolysate Delay introduction of solid foods > 6 mo Cow milk/dairy: 6-12 months Egg: months Peanut, tree nut, seafood > mo
79 Identification of causative food Institution of elimination diet Education on food avoidance Development of action plan Prevention of other allergies
80 History and physical paramount IgE & non-ige mediated conditions exist Diagnosis by elimination and challenge Avoidance/education/preparation for emergencies are current therapies Periodic re-challenge to monitor tolerance as indicated by history, allergen, and level of food specific-ige
81 Review several new forms of allergen immunotherapy Discuss positive and negative findings of their use in clinical trials and argument if they might become available in the future Discuss the usefulness of immunotherapy in food allergy and the current status of these investigations
82 Recombinant anti-ige antibody (Stanford) Gene (naked DNA) immunization with CPG repeats (Johns Hopkins) Sublingual Immunotherapy (Stanford) Oral Immunotherapy (Stanford) Hypo-allergenic formulas (Stanford) Probiotics (UCSF)
83 Background BACKGROUND There is no effective, FDA-approved treatment for food allergy, except to avoid the offending foods and to have ready access to self-injectable epinephrine. Recently, oral desensitization has been used to treat patients with food allergy; the process is slow and associated with frequent allergic reactions.
84 OIT (multi or single) yrs Milk, Wheat, Egg, Peanut, Tree Nut, Sesame Seed, and/or Soy Recombinant anti-ige antibody + OIT yrs Sublingual Immunotherapy (peanut only) yrs Skin patch (peanut only) yrs Chinese Herbal Medicine yrs Recombinant/Engineered protein allergens Peanut OIT- 12 mo to 48 mo Lactobacillus (genetically modified)---phase I Denatured/baked milk vs non baked milk yrs Highly cooked egg vs less cooked egg yrs
85 Oral Immunotherapy Study Design Provided by Dr. Wesley Burks of Duke University
86 * Inclusion Criteria: Age >4 yrs age Symptomatic food allergy sensitivity include positive skin prick testing (greater tha n 8 mm) and specific IgE > 7 ku/l. Medically documented history of near fatal reaction to food ingestion Positive DBPCFC Allowed to take antihistamines, asthma meds, and nasal steroid s as indicated for symptomatic control of atopic conditions Exclusion Criteria: No significant organ system disease Failure to comply with training for allergy reactions FEV1 or PEF is <80% predicted with or without meds Subjects taking oral, IM,IV steroids, beta blockers. * Similar to Duke and Arkansas
87 Screening period is very important Preliminary Dosing Visit: Incremental escalating doses of fod flour given orally as tolerated to a max of the top dose of allergen of 6 mg (as per Duke and Arkansas protocol). Up dosing visits weekly to MTD (awareness of symptoms) Treatment Course: Top dose ( maintenance dose ) self administered daily for minimum of 12 months Blood samples minimally should be collected at baseline, 6 months, 12 months, continuing
88 Role of Adjunctive therapy in OIT: Use of Anti IgE in reported studies as example AAAAI, 2011 Savage, et al. Omalizumab In Peanut Allergy: Effects On The Basophil, Mast Cell, And Food Challenge Response N=10 Peanut-allergic adults with 6 mos of omalizumab. At a median of 5 weeks, a DBPCPC was performed in 9 subjects. Results: There was a significant increase in the mean dose of peanut protein tolerated (DPP, 212 mg to 6,010 mg,p<0.01) AAAAI, 2011 Pena-Peloche, et al. Treatment Of Severe And Persistent Food Allergy With Omalizumab Milk and egg allergic children underwent 16 weeks of omalizumab. Out of seven patients, 2 patients showed improvement on food challenge, 3 patients went forward with OIT. JACI, 2011 Sampson, et al. A phase II, randomized, double-blind, parallel-group, placebo-controlled oral food challenge trial of Xolair (omalizumab) in peanut allergy subjects reached primary endpoint (n=9 Xolair and n=5 placebo) and comparing change from baseline in maximum tolerable peanut dose after 24 wks of treatment, there appeared to be a greater shift in peanut tolerability in subjects treated with omalizumab (44%) vs placebo (20%). NEJM, 2003 Leung, D. et al. Effect of anti-ige therapy in patients with peanut allergy A double-blind, randomized, dose-ranging trial in 84 patients. A 450-mg dose of TNX-901 increased the threshold of sensitivity to peanut on oral food challenge from 0.5 to 9 peanuts. Allergy Asthma Proc Rafi, et al. Effects of omalizumab in patients with food allergy. Assessed the efficacy of omalizumab in 22 patients with persistent asthma and concomitant IgEmediated food allergy with improvement on reexposure to sensitized foods.
89 CURRENTLY ONGOING ANTI IGE AND FOOD ORAL IMMUNOTHERAPY STUDIES - Milk OIT + omalizumab in milk allergic subjects (7-35 yrs) PI, Dr. Hugh Sampson Peanut OIT + omalizumab study in peanut allergic patients (>12 yrs) PI, Dr. Wesley Burks Peanut OIT + anti IgE in peanut allergic subjects (>18 yrs) Novartis Peanut OIT + omalizumab in peanut allergic subjects (7-25 yrs) PI, Dr. Dale T. Umetsu Multi OIT + omalizumab in tree nut, milk, egg, and/or peanut allergic subjects (4-55 yrs) PI, Dr. Kari Nadeau Source: clinicaltrials.gov
90 Mechanisms of Anti IgE Therapy IgE Anti-IgE Anti-IgE FcεRI receptor Mast cell Monoclonal anti-ige antibodies, like omalizumab, selectively bind to the Cɛ3 domain of IgE with high affinity. Each IgE molecule has two antigenic sites for anti-ige, and so can be bound by two drug molecules simultaneously. These form small, soluble, biologically inert IgE/anti-IgE complexes that are easily cleared from the circulation.
91 Possible historical comparisons: Cow s milk OIT with no omalizumab Anti IgE Studies in Food Allergy at Stanford (example) Study Patient Population Methods Results Yu et al. (2009) 5 pts (5-25 yrs) with peanut allergy; positive peanut SPT ( 8mm wheal) or serumspecific IgE (peanut IgE 15kUa/L) Pilot study using omalizumab every 2-4 wks (dosing based on wgt/ige level per product insert); no placebo Free IgE anti-peanut decreased (from mean of kua/l to 5.9 kua/l) within 4-12 wks of treatment. One pt developed a negative peanut SPT at 4 wks and was able to tolerate 5 gms of peanut in DBPCFC. Iyengar et al. (2008) 8 patients (4-22 yrs) with food allergy and severe refractory AD Pilot phase I study using higher dosing frequency of omalizumab for higher IgE levels (<3,000 IU/ml; mean=1,068 IU/ml) and 1:1 placebo Clinical effect not markedly different (likely due to very high serum total IgE); TARC, TSLP, and OX40 ligand reduced (60-80% in 3/4 pts; 50-75% and 70-80% in 4/4 pts, respectively) and IL-10 levels increased % in treatment group Nadeau et al (2011) 11 children (7-17 years) with cow s milk allergy; milk-specific IgE (median 50; range kua/l), positive milk SPT (median 20/50 mm; range, 11-45/20-52 mm), Pilot phase I study using omalizumab (starting 9 wks before) rapid oral milk desensitization to 1000-mg; wkly dose increase over next 7-12 wks 9/10 patients reached 1000-mg dose during oneday desensitization period; 9/10 patients reached the max 2000 mg daily dose by wk 16; All 9 pts passed DBPCFC 8 wks after last dose (wk 24) during which cumulative dose of 7250 mg (or 220 ml milk) given. All 9 pts continued daily milk >8000 mg/day after DBPCFC; reactions (mostly local and GI) occurred at approx. 1%
92 Phase I single center study using AntiIgE Schematic with milk of Clinical oral Study: immunotherapy Study design: Baseline visit Start omalizumab (wk 0) Desensitization (1000 mg milk powder dose, 2000 mg cumulative) Weekly up dosing and continued omalizumab Maintain daily milk dose at home Off omalizumab Maintenance dose was 2000 mg DBPCFC* Week 0-9 Week 9 Week 9-16, escalation phase Week Week Home daily milk 8 oz Week Nadeau, K, Schneider, L, Hoyte, L, Borras, I, and Umetsu, D. JACI *DBPCFC=double blind placebo controlled food challenge
93 Summary of Demographics Subject Characteristics 11 patients with histories of acute reactions to uncooked and cooked milk (recruited at 2 study sites). Subjects with prior history of eosinophilic GI diseases, immunotherapy, severe asthma, and/or history of intubation were excluded. Mean age: 10 years (median 8 years). Mean skin test to milk: 22 mm wheal (median 20 mm). Mean milk specific IgE: 98 ku/l (median 50 ku/l). Mean total IgE: 701 ku/l (median 349 ku/l). Nadeau, K, Schneider, L, Hoyte, L, Borras, I, and Umetsu, D. JACI. 2011
94 Results Efficacy Results One-day desensitization to 1,000 mg (cumulative dose=2,000 mg of milk) 7 out of 11 patients passed. One drop out after first day of desensitization. After up to 7-11 additional wks, 9 out of 10 subjects reached an oral daily dose of 2,000 mg (primary endpoint) At wks, DBPCFC to 3,000 mg (cumulative dose 7,200 mg) 9 out of 10 patients passed. After passing DBPCFC, 9 patients began tolerating 8-12 oz milk/day (including ice cream, pizza, yogurt) the next day. Nadeau, K, Schneider, L, Hoyte, L, Borras, I, and Umetsu, D. JACI. 2011
95 Results: Overall Safety Data Safety Results Total number of subjects=11 Milk doses per child, mean (range) 209 (36-334) Symptom/treatment Total doses 2301 No. (%) of total doses No. of reactions per child, mean (range) Total reactions 41 (1.8%) 3.7 (1-7) Grade 1 (Mild) symptoms 29 (1.3%) 2.6 (1-5) On rush desensitization day 14 During weekly dose escalation phase During maintenance dosing 5 Grade 2 (Moderate) symptoms 8 (0.3%) 0.7 (0-2) On rush desensitization day 5 During weekly dose escalation phase During maintenance dosing 2 Grade 3 (Severe) symptoms 4* (0.1%) 0.3 (0-1) On rush desensitization day 2 During weekly dose escalation phase During maintenance dosing 1 Nadeau, K, Schneider, L, Hoyte, L, Borras, I, and Umetsu, D. JACI
96 Summary CLINICAL CONCLUSIONS This study is the first published study to use omalizumab in combination with oral desensitization. 9 of 11 patients with milk allergy treated with omalizumab and oral milk desensitization achieved the primary objective, and tolerated desensitization to a dose of 2,000 mg/day within 7-10 wks. The 9 patients then passed a DBPCFC, and began tolerating >240 ml (>8 oz) of milk/day in their diet. These results suggest a potential value for using omalizumab during rapid oral desensitization for food allergy. Nadeau, K, Schneider, L, Hoyte, L, Borras, I, and Umetsu, D. JACI. 2011
97 Summary SAFETY OIT: CONCLUSIONS There is no cure at the current time. Drop out rates during clinical OIT studies are 15-25% Although most reactions are mild, up to 4% have been reported to be severe (requiring epinephrine). Most allergic reactions occur during home dosing Patients and families must be frequently educated Random allergic reactions can occur 3-4 years after OIT was begun. Viral infections, temperature, other allergies, exercise, menstruation all can modulate the threshold for an allergic reaction during ingestion of food therapy Reaction medications must still be available at all times
98 Possible mechanisms of Oral Immunotherapy Incorvaia, et al. 2008, Antunez, et al. 2008, Aslam, et al 2010, Frew, 2010, Jutel, et al. 2006, Jones, et al. 2009, Adkis and Adkis, 2009 Nadeau and Umetsu, 2011
99 Why study mechanisms of OIT? Provides our field with new targets for Therapy (ie. peptide vaccine based in recognized epitopes in T cells) Diagnostics (ie. basophil activation) Prognostics (ie. following epitope arrays and inhibitory assays) Identifies predictive biomarkers in samples for successful and safe clinical outcomes (ie. Treg epigenetics? Basophil threshold studies?) Defines biological parameters for improved, customized, patient-focused therapy (dose amount, dose frequency, initiation and termination of therapy, adverse event frequency)
100
101 OIT Study Summary Results OIT could be promising HOWEVER It must be considered experimental and in its early phases There is still much to learn as to dosing and frequency and length of time on therapy SAFETY is paramount Work with appropriate regulatory agencies and institutional boards Trained staff should perform DBPCFCs and DEs in a hospital setting Patients and their families must be trained and frequently retrained Constant (i.e. 24/7) availability of trained staff, short term and long term follow up are important. OIT IS NOT READY FOR CLINIC USE
102 Identification of causative food Institution of elimination diet Education on food avoidance Development of action plan Prevention of other allergies
103 History and physical paramount IgE & non-ige mediated conditions exist Diagnosis by elimination and challenge Avoidance/education/preparation for emergencies are current therapies Periodic re-challenge to monitor tolerance as indicated by history, allergen, and level of food specific-ige
104 Stanford Alliance For Food Allergy Research Funded By:
105 Seeking Clinical Trials and Mechanistic Assays of Immune Tolerance in Allergy and Asthma The ITN provides: Funding for innovative research Collaborative scientific exchange Public education and involvement Partnership opportunities Submit your proposal:
106 Any questions? Contact
Pediatric Food Allergies: Physician and Parent. Robert Anderson MD Rachel Anderson Syracuse, NY March 3, 2018
 Pediatric Food Allergies: Physician and Parent Robert Anderson MD Rachel Anderson Syracuse, NY March 3, 2018 Learning Objectives Identify risk factors for food allergies Identify clinical manifestations
Pediatric Food Allergies: Physician and Parent Robert Anderson MD Rachel Anderson Syracuse, NY March 3, 2018 Learning Objectives Identify risk factors for food allergies Identify clinical manifestations
WHY IS THERE CONTROVERSY ABOUT FOOD ALLERGY AND ECZEMA. Food Allergies and Eczema: Facts and Fallacies
 Food Allergies and Eczema: Facts and Fallacies Lawrence F. Eichenfield,, M.D. Professor of Clinical Pediatrics and Medicine (Dermatology) University of California, San Diego Rady Children s s Hospital,
Food Allergies and Eczema: Facts and Fallacies Lawrence F. Eichenfield,, M.D. Professor of Clinical Pediatrics and Medicine (Dermatology) University of California, San Diego Rady Children s s Hospital,
COW S MILK PROTEIN ALLERGY IN CHILDREN
 COW S MILK PROTEIN ALLERGY IN CHILDREN Wednesday 8th June 2016 By Dr Rukhsana Hussain CMPA Cows' milk protein allergy is an immune-mediated allergic response to proteins in milk Milk contains casein and
COW S MILK PROTEIN ALLERGY IN CHILDREN Wednesday 8th June 2016 By Dr Rukhsana Hussain CMPA Cows' milk protein allergy is an immune-mediated allergic response to proteins in milk Milk contains casein and
Oral food immunotherapy/desensitization
 Oral Immunotherapy and Anti-IgE Antibody- Adjunctive Treatment for Food Allergy: Omalizumab facilitates oral desensitization in high-risk peanut allergy patients Dale T. Umetsu, MD, PhD The Prince Turki
Oral Immunotherapy and Anti-IgE Antibody- Adjunctive Treatment for Food Allergy: Omalizumab facilitates oral desensitization in high-risk peanut allergy patients Dale T. Umetsu, MD, PhD The Prince Turki
APPROACH TO FOOD ALLERGY IN CHILDREN WHY TALK ABOUT FOOD ALLERGY? DISEASES BLAMED ON FOOD ALLERGY ADVERSE REACTIONS TO FOOD OVERVIEW
 APPROACH TO FOOD ALLERGY IN CHILDREN DR MEERA THALAYASINGAM INTERNATIONAL MEDICAL UNIVERSITY RAMSAY SIME DARBY HEALTHCARE MALAYSIA APAPARI WORKSHOP PHNOM PENH CAMBODIA_ 12 TH SEPT 2015 WHY TALK ABOUT FOOD
APPROACH TO FOOD ALLERGY IN CHILDREN DR MEERA THALAYASINGAM INTERNATIONAL MEDICAL UNIVERSITY RAMSAY SIME DARBY HEALTHCARE MALAYSIA APAPARI WORKSHOP PHNOM PENH CAMBODIA_ 12 TH SEPT 2015 WHY TALK ABOUT FOOD
'Every time I eat dairy foods I become ill, could I have a milk allergy.? '. Factors involved in the development of cow's milk allergy:
 'Every time I eat dairy foods I become ill, could I have a milk allergy.? '. Dairy allergy is relatively common in the community. The unpleasant symptoms some people experience after eating dairy foods
'Every time I eat dairy foods I become ill, could I have a milk allergy.? '. Dairy allergy is relatively common in the community. The unpleasant symptoms some people experience after eating dairy foods
Food Allergy A buffet of truths and myths
 Food Allergy A buffet of truths and myths Toronto Anaphylaxis Education Group Adelle R. Atkinson M.D. FRCPC Associate Professor of Paediatrics University of Toronto Clinical Immunologist Division of Immunology
Food Allergy A buffet of truths and myths Toronto Anaphylaxis Education Group Adelle R. Atkinson M.D. FRCPC Associate Professor of Paediatrics University of Toronto Clinical Immunologist Division of Immunology
Paediatric Food Allergy and Intolerance. Abigail Macleod, Associate Specialist, RBH
 Paediatric Food Allergy and Intolerance Abigail Macleod, Associate Specialist, RBH Ig E mediated food allergy Commonest cause of chronic disease in childhood up to 20% children But treatable, manageable
Paediatric Food Allergy and Intolerance Abigail Macleod, Associate Specialist, RBH Ig E mediated food allergy Commonest cause of chronic disease in childhood up to 20% children But treatable, manageable
Disclaimers. Food Allergy. Outline. Disclaimers II
 Disclaimers Food Allergy Matthew Fogg MD Allergy and Asthma Specialists I have no conflict of interest in any of the information I am providing. The information I am providing is free of bias. I have no
Disclaimers Food Allergy Matthew Fogg MD Allergy and Asthma Specialists I have no conflict of interest in any of the information I am providing. The information I am providing is free of bias. I have no
This Product May Contain Trace Amounts of Peanuts Educating Families & Patients About Food Allergies
 This Product May Contain Trace Amounts of Peanuts Educating Families & Patients About Food Allergies Kenya Beard EdD GNP-C NP-C ACNP-BC K Beard & Associates, LLC Assistant Professor Hunter College kenya@kbeardandassociates.com
This Product May Contain Trace Amounts of Peanuts Educating Families & Patients About Food Allergies Kenya Beard EdD GNP-C NP-C ACNP-BC K Beard & Associates, LLC Assistant Professor Hunter College kenya@kbeardandassociates.com
Food Allergies Among Children -
 Food Allergies Among Children - Growth, Treatment, Prevention and a Challenge for the Food Industry Steve L. Taylor, Ph.D. Food Allergy Research & Resource Program University of Nebraska Food Navigator
Food Allergies Among Children - Growth, Treatment, Prevention and a Challenge for the Food Industry Steve L. Taylor, Ph.D. Food Allergy Research & Resource Program University of Nebraska Food Navigator
How to avoid complete elimination
 How to avoid complete elimination Yu Okada 1, 2), Noriyuki Yanagida 2), Sakura Sato 2), Motohiro Ebisawa 2) 1) Department of Family Physician, Kameda Family Clinic Tateyama, Chiba, Japan 2) Department
How to avoid complete elimination Yu Okada 1, 2), Noriyuki Yanagida 2), Sakura Sato 2), Motohiro Ebisawa 2) 1) Department of Family Physician, Kameda Family Clinic Tateyama, Chiba, Japan 2) Department
GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE AND PRESCRIPTION OF LOW LACTOSE INFANT FORMULA.
 GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE AND PRESCRIPTION OF LOW LACTOSE INFANT FORMULA. These are the lactose intolerance guidelines and it is recommended that they are used in
GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE AND PRESCRIPTION OF LOW LACTOSE INFANT FORMULA. These are the lactose intolerance guidelines and it is recommended that they are used in
Sequoia Education Systems, Inc. 1
 Functional Medicine University s Functional Diagnostic Medicine Program Module 3 * FDMT 527C The Elimination Diet & The Modified Elimination Diet Wayne L. Sodano, D.C., D.A.B.C.I. & Ron Grisanti, D.C.,
Functional Medicine University s Functional Diagnostic Medicine Program Module 3 * FDMT 527C The Elimination Diet & The Modified Elimination Diet Wayne L. Sodano, D.C., D.A.B.C.I. & Ron Grisanti, D.C.,
S101- Food Allergies and Formula Sensitivity
 S101- Food Allergies and Formula Sensitivity Vivian Hernandez-Trujillo, MD Director, Division of Allergy and Immunology Director, Allergy-Immunology Fellowship Miami Children s Hospital Miami, Florida
S101- Food Allergies and Formula Sensitivity Vivian Hernandez-Trujillo, MD Director, Division of Allergy and Immunology Director, Allergy-Immunology Fellowship Miami Children s Hospital Miami, Florida
prevalence 181 Atopy patch test, see Patch test
 Subject Index AD, see Atopic dermatitis Adrenaline, anaphylaxis management 99 101, 194, 195 Adverse food reaction definition 4 nonallergic reactions 6, 9 Allergen Nomenclature database 20, 21 Allergen
Subject Index AD, see Atopic dermatitis Adrenaline, anaphylaxis management 99 101, 194, 195 Adverse food reaction definition 4 nonallergic reactions 6, 9 Allergen Nomenclature database 20, 21 Allergen
GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE
 GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE These are the lactose intolerance guidelines and it is recommended that they are used in conjunction with the Cow s Milk Allergy guidance.
GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE These are the lactose intolerance guidelines and it is recommended that they are used in conjunction with the Cow s Milk Allergy guidance.
Understanding Food Intolerance and Food Allergy
 Understanding Food Intolerance and Food Allergy There are several different types of sensitivities or adverse reactions to foods. One type is known as a food intolerance ; an example is lactose intolerance.
Understanding Food Intolerance and Food Allergy There are several different types of sensitivities or adverse reactions to foods. One type is known as a food intolerance ; an example is lactose intolerance.
Objectives. 1 st half: 2 nd half:
 Ask the Allergist Edmond S. Chan, MD, FRCPC Clinical Associate Professor, UBC Division of Allergy & Immunology June 14, 2014 Metro Vancouver Anaphylaxis Group Burnaby Objectives 1 st half: Discuss: How
Ask the Allergist Edmond S. Chan, MD, FRCPC Clinical Associate Professor, UBC Division of Allergy & Immunology June 14, 2014 Metro Vancouver Anaphylaxis Group Burnaby Objectives 1 st half: Discuss: How
Infants and Toddlers: Food Allergies and Food Intolerance
 Infants and Toddlers: Food Allergies and Food Intolerance A Webinar Presented by the Virginia Infant & Toddler Specialist Network and the Fairfax County Office for Children WHAT IS THE DIFFERENCE BETWEEN
Infants and Toddlers: Food Allergies and Food Intolerance A Webinar Presented by the Virginia Infant & Toddler Specialist Network and the Fairfax County Office for Children WHAT IS THE DIFFERENCE BETWEEN
GP Patient Pathway for Infants under 1 year of age with Cows Milk Protein Allergy (Non IgE Mediated)
 GP Patient Pathway for Infants under 1 year of age with Cows Milk Protein Allergy (Non IgE Mediated) Infant suspected with (non IgE) after an allergy focused clinical history has been completed (see appendix
GP Patient Pathway for Infants under 1 year of age with Cows Milk Protein Allergy (Non IgE Mediated) Infant suspected with (non IgE) after an allergy focused clinical history has been completed (see appendix
FPIES ANOTHER DISEASE ABOUT WHICH YOU SHOULD KNOW OBJECTIVES FPIES FPIES 11/10/2016. What is that? Robert P. Dillard, M.D.
 ANOTHER DISEASE ABOUT WHICH YOU SHOULD KNOW What is that? Robert P. Dillard, M.D. Food Protein Induced Enterocolitis Syndrome. OBJECTIVES 1: Awareness of this syndrome 2: Characteristics 3: Diagnosis 4:
ANOTHER DISEASE ABOUT WHICH YOU SHOULD KNOW What is that? Robert P. Dillard, M.D. Food Protein Induced Enterocolitis Syndrome. OBJECTIVES 1: Awareness of this syndrome 2: Characteristics 3: Diagnosis 4:
Dietary Management of Cow s Milk Protein Allergy
 Dietary Management of Cow s Milk Protein Allergy Amy Roberts Paediatric Dietitians September 2014 Objectives To increase confidence in diagnosing a cow s milk allergy To understand the difference between
Dietary Management of Cow s Milk Protein Allergy Amy Roberts Paediatric Dietitians September 2014 Objectives To increase confidence in diagnosing a cow s milk allergy To understand the difference between
Beth Strong, RN, FNP-C The Jaffe Food Allergy Institute Mount Sinai School of Medicine New York 2/23/13
 Beth Strong, RN, FNP-C The Jaffe Food Allergy Institute Mount Sinai School of Medicine New York 2/23/13 I do not have any financial disclosure to report Why Challenge? To confirm that the suspected food
Beth Strong, RN, FNP-C The Jaffe Food Allergy Institute Mount Sinai School of Medicine New York 2/23/13 I do not have any financial disclosure to report Why Challenge? To confirm that the suspected food
Prevention and Response
 Prevention and Response Allergy and Anaphylaxis Pre-Test Questions 1. Name 6 of the 8 most common food allergens. 2. Name 10 common signs and symptoms of an allergic reaction. 3. What is the immediate
Prevention and Response Allergy and Anaphylaxis Pre-Test Questions 1. Name 6 of the 8 most common food allergens. 2. Name 10 common signs and symptoms of an allergic reaction. 3. What is the immediate
Managing Food Allergies in School April 9, Maria Crain, RN, CPNP Amy Arneson, RN, BSN Food Allergy Center Children s Medical Center Dallas
 Managing Food Allergies in School April 9, 2011 Maria Crain, RN, CPNP Amy Arneson, RN, BSN Food Allergy Center Children s Medical Center Dallas -None Conflict of Interest Learning Objectives -Define food
Managing Food Allergies in School April 9, 2011 Maria Crain, RN, CPNP Amy Arneson, RN, BSN Food Allergy Center Children s Medical Center Dallas -None Conflict of Interest Learning Objectives -Define food
rgies_immune/food_allergies.html
 http://www.kidshealth.org/teen/diseases_conditions/alle rgies_immune/food_allergies.html Food Allergies Peter had always loved seafood, so he was surprised one day when he noticed his mouth tingling after
http://www.kidshealth.org/teen/diseases_conditions/alle rgies_immune/food_allergies.html Food Allergies Peter had always loved seafood, so he was surprised one day when he noticed his mouth tingling after
Gluten Sensitivity Fact from Myth. Disclosures OBJECTIVES 18/09/2013. Justine Turner MD PhD University of Alberta. None Relevant
 Gluten Sensitivity Fact from Myth Justine Turner MD PhD University of Alberta Disclosures None Relevant OBJECTIVES Understand the spectrum of gluten disorders Develop a diagnostic algorithm for gluten
Gluten Sensitivity Fact from Myth Justine Turner MD PhD University of Alberta Disclosures None Relevant OBJECTIVES Understand the spectrum of gluten disorders Develop a diagnostic algorithm for gluten
LIVING WITH FOOD ALLERGY
 LIVING WITH FOOD ALLERGY D R J E N N Y H U G H E S C O N S U L T A N T P A E D I A T R I C I A N N O R T H E R N H E A L T H & S O C I A L C A R E T R U S T QUIZ: TRUE / FALSE Customers with food allergies
LIVING WITH FOOD ALLERGY D R J E N N Y H U G H E S C O N S U L T A N T P A E D I A T R I C I A N N O R T H E R N H E A L T H & S O C I A L C A R E T R U S T QUIZ: TRUE / FALSE Customers with food allergies
Prescribing Guidelines for Lactose Intolerance and Cow s Milk Protein Allergy
 Prescribing Guidelines for and Aim To clarify which products and in which circumstances milk substitutes can be prescribed for babies and young children in primary care, as well as to give a guide to prescribing
Prescribing Guidelines for and Aim To clarify which products and in which circumstances milk substitutes can be prescribed for babies and young children in primary care, as well as to give a guide to prescribing
Clinical Manifestations and Management of Food Allergy
 Clinical Manifestations and Management of Food Allergy Adrian Sie Consultant in paediatrics, Wishaw General, Lanarkshire April 2013 To do Bring Allergy plan Prevention photo Contents Is it allergy? How
Clinical Manifestations and Management of Food Allergy Adrian Sie Consultant in paediatrics, Wishaw General, Lanarkshire April 2013 To do Bring Allergy plan Prevention photo Contents Is it allergy? How
Peanut and Tree Nut allergy
 Peanut and Tree Nut allergy What are peanuts & tree nuts? Peanuts are also called ground nuts, monkey nuts, beer nuts, earth nuts, goober peas, mendelonas and arachis Tree nuts include almond, Brazil,
Peanut and Tree Nut allergy What are peanuts & tree nuts? Peanuts are also called ground nuts, monkey nuts, beer nuts, earth nuts, goober peas, mendelonas and arachis Tree nuts include almond, Brazil,
Primary Prevention of Food Allergies
 Primary Prevention of Food Allergies Graham Roberts Professor & Honorary Consultant, Paediatric Allergy and Respiratory Medicine, David Hide Asthma and Allergy Research Centre, Isle of Wight & CES & HDH,
Primary Prevention of Food Allergies Graham Roberts Professor & Honorary Consultant, Paediatric Allergy and Respiratory Medicine, David Hide Asthma and Allergy Research Centre, Isle of Wight & CES & HDH,
Aquarium of the Pacific Food Allergy and Anaphylaxis Protocol
 Aquarium of the Pacific Food Allergy and Anaphylaxis Protocol Purpose Statement: The Aquarium of the Pacific recognizes the increasing prevalence of allergies in children, including many life threatening
Aquarium of the Pacific Food Allergy and Anaphylaxis Protocol Purpose Statement: The Aquarium of the Pacific recognizes the increasing prevalence of allergies in children, including many life threatening
Prescribing Commissioning Policy May Diagnosis and management of Cow s Milk Protein Allergy (CMPA) and Lactose Intolerance
 Prescribing Commissioning Policy May 2018 Diagnosis and management of Cow s Milk Protein Allergy (CMPA) and Lactose Intolerance NHS Eastern Cheshire, NHS South Cheshire and NHS Vale Royal Clinical Commissioning
Prescribing Commissioning Policy May 2018 Diagnosis and management of Cow s Milk Protein Allergy (CMPA) and Lactose Intolerance NHS Eastern Cheshire, NHS South Cheshire and NHS Vale Royal Clinical Commissioning
Guidelines for the Diagnosis and Management of Food Allergy in the United States. Summary for Patients, Families, and Caregivers
 Guidelines for the Diagnosis and Management of Food Allergy in the United States NIAID Summary for Patients, Families, and Caregivers National Institute of Allergy and Infectious Diseases U.S. DEPARTMENT
Guidelines for the Diagnosis and Management of Food Allergy in the United States NIAID Summary for Patients, Families, and Caregivers National Institute of Allergy and Infectious Diseases U.S. DEPARTMENT
Food Allergy Prevention, Detection and Treatment
 Food Allergy Prevention, Detection and Treatment Scott H. Sicherer, MD Jaffe Professor of Pediatrics, Allergy and Immunology NJAAP Annual Conference May 11, 2016 Disclosures and Learning Objectives I have
Food Allergy Prevention, Detection and Treatment Scott H. Sicherer, MD Jaffe Professor of Pediatrics, Allergy and Immunology NJAAP Annual Conference May 11, 2016 Disclosures and Learning Objectives I have
FOOD ALLERGY PROTOCOL
 FOOD ALLERGY PROTOCOL Kerby is dedicated to keeping students with food allergies safe in the school environment. There is no one way to manage food allergies and each student s situation needs careful
FOOD ALLERGY PROTOCOL Kerby is dedicated to keeping students with food allergies safe in the school environment. There is no one way to manage food allergies and each student s situation needs careful
Food Allergies. In the School Setting
 Food Allergies In the School Setting Food Allergy Basics Food Allergy Basics The role of the immune system is to protect the body from germs and disease A food allergy is an abnormal response by the immune
Food Allergies In the School Setting Food Allergy Basics Food Allergy Basics The role of the immune system is to protect the body from germs and disease A food allergy is an abnormal response by the immune
Food Allergy. Allergy and Immunology Awareness Program
 Food Allergy Allergy and Immunology Awareness Program Food Allergy Allergy and Immunology Awareness Program What is a food allergy? A food allergy is when your body s immune system reacts to a food protein
Food Allergy Allergy and Immunology Awareness Program Food Allergy Allergy and Immunology Awareness Program What is a food allergy? A food allergy is when your body s immune system reacts to a food protein
CLINICAL AUDIT. Appropriate prescribing of specialised infant formula for cows milk protein allergy
 CLINICAL AUDIT Appropriate prescribing of specialised infant formula for cows milk protein allergy Valid to December 2019 bpac nz better medicin e Background Specialised infant formulae subsidised on the
CLINICAL AUDIT Appropriate prescribing of specialised infant formula for cows milk protein allergy Valid to December 2019 bpac nz better medicin e Background Specialised infant formulae subsidised on the
Food Intolerance & Expertise SARAH KEOGH CONSULTANT DIETITIAN EATWELL FOOD & NUTRITION
 Food Intolerance & Expertise SARAH KEOGH CONSULTANT DIETITIAN EATWELL FOOD & NUTRITION Food Intolerance & Expertise What is food intolerance? Common food intolerances Why are consumers claiming more food
Food Intolerance & Expertise SARAH KEOGH CONSULTANT DIETITIAN EATWELL FOOD & NUTRITION Food Intolerance & Expertise What is food intolerance? Common food intolerances Why are consumers claiming more food
PREVENTION OF FOOD ALLERGY. Dr Kate Swan Dr Claire Stockdale
 PREVENTION OF FOOD ALLERGY Dr Kate Swan Dr Claire Stockdale Objectives To understand: Food allergy phenotypes The role of the skin barrier in sensitisation Early introduction of food as an allergy prevention
PREVENTION OF FOOD ALLERGY Dr Kate Swan Dr Claire Stockdale Objectives To understand: Food allergy phenotypes The role of the skin barrier in sensitisation Early introduction of food as an allergy prevention
Food Allergies: Fact from Fiction
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/gi-insights/food-allergies-fact-from-fiction/3598/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/gi-insights/food-allergies-fact-from-fiction/3598/
Cow's milk protein allergy (CMPA) suspected
 Background information Patient information Key messages for this pathway When to suspect CMPA Symptoms of CMPA and assessing severity Symptoms of non IgE mediated CMPA Severe CMPA: urgent referral to paediatric
Background information Patient information Key messages for this pathway When to suspect CMPA Symptoms of CMPA and assessing severity Symptoms of non IgE mediated CMPA Severe CMPA: urgent referral to paediatric
Preventing food allergy in higher risk infants: guidance for healthcare professionals
 Preventing food allergy in higher risk infants: guidance for healthcare professionals This information sheet complements current advice from the Scientific Advisory Committee on Nutrition (SACN) and the
Preventing food allergy in higher risk infants: guidance for healthcare professionals This information sheet complements current advice from the Scientific Advisory Committee on Nutrition (SACN) and the
Anaphylaxis in Schools School Year
 Anaphylaxis in Schools 2017-2018 School Year Overview Sabrina s Law Expectations for School Staff Definition of Anaphylaxis Recognition Action How to use an Auto-injector Sabrina s Law Legislation: Bill
Anaphylaxis in Schools 2017-2018 School Year Overview Sabrina s Law Expectations for School Staff Definition of Anaphylaxis Recognition Action How to use an Auto-injector Sabrina s Law Legislation: Bill
Diagnostic Testing Algorithms for Celiac Disease
 Diagnostic Testing Algorithms for Celiac Disease HOT TOPIC / 2018 Presenter: Melissa R. Snyder, Ph.D. Co-Director, Antibody Immunology Laboratory Department of Laboratory Medicine and Pathology, Mayo Clinic
Diagnostic Testing Algorithms for Celiac Disease HOT TOPIC / 2018 Presenter: Melissa R. Snyder, Ph.D. Co-Director, Antibody Immunology Laboratory Department of Laboratory Medicine and Pathology, Mayo Clinic
Allergy and Anaphylaxis Policy
 Statement This policy serves to promote an allergy aware community. At Splash Centre we have recognised the need to adopt a policy on allergies that may be present in the children who attend our centre.
Statement This policy serves to promote an allergy aware community. At Splash Centre we have recognised the need to adopt a policy on allergies that may be present in the children who attend our centre.
Oral Food Challenges in an Office Setting
 Oral Food Challenges in an Office Setting S. Allan Bock, MD National Jewish Health and Boulder Valley Asthma and Allergy Clinic, University of Colorado, Denver School of Medicine, Boulder, California Faculty
Oral Food Challenges in an Office Setting S. Allan Bock, MD National Jewish Health and Boulder Valley Asthma and Allergy Clinic, University of Colorado, Denver School of Medicine, Boulder, California Faculty
According to a post-hoc analysis, 62.6% of patients receiving Viaskin Peanut showed an increase in their eliciting dose at 12 months of treatment
 Montrouge, France, February 22, 2019 DBV Technologies Announces Publication of Detailed Phase III Trial Results Evaluating Viaskin Peanut as a Novel Treatment for Peanut Allergy in The Journal of the American
Montrouge, France, February 22, 2019 DBV Technologies Announces Publication of Detailed Phase III Trial Results Evaluating Viaskin Peanut as a Novel Treatment for Peanut Allergy in The Journal of the American
Associate Professor Rohan Ameratunga
 Associate Professor Rohan Ameratunga Adult and Paediatric Clinical Immunologist and Allergist Auckland 9:25-9:45 Preventing Food Allergy Update on Food allergy Associate Professor Rohan Ameratunga Food
Associate Professor Rohan Ameratunga Adult and Paediatric Clinical Immunologist and Allergist Auckland 9:25-9:45 Preventing Food Allergy Update on Food allergy Associate Professor Rohan Ameratunga Food
Primary Care Update January 26 & 27, 2017 Celiac Disease: Concepts & Conundrums
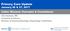 Primary Care Update January 26 & 27, 2017 Celiac Disease: Concepts & Conundrums Alia Hasham, MD Assistant Professor Division of Gastroenterology, Hepatology & Nutrition What is the Preferred Initial Test
Primary Care Update January 26 & 27, 2017 Celiac Disease: Concepts & Conundrums Alia Hasham, MD Assistant Professor Division of Gastroenterology, Hepatology & Nutrition What is the Preferred Initial Test
Special Health Care Needs in Early Childhood: Food Allergies
 Special Health Care Needs in Early Childhood: Food Allergies Colleen Kraft, M.D., FAAP CHSA Annual Conference April 12, 2016 Who s Here Today? Health Managers? Family Services Managers? Other Area Managers?
Special Health Care Needs in Early Childhood: Food Allergies Colleen Kraft, M.D., FAAP CHSA Annual Conference April 12, 2016 Who s Here Today? Health Managers? Family Services Managers? Other Area Managers?
Guideline for the Management of Children with Egg Allergy and guidance on referral to paediatric allergy clinic
 Guideline for the Management of Children with Egg Allergy and guidance on referral to paediatric allergy clinic Aim and Scope To give guidance on how to identify those children who have egg allergy or
Guideline for the Management of Children with Egg Allergy and guidance on referral to paediatric allergy clinic Aim and Scope To give guidance on how to identify those children who have egg allergy or
ImuPro shows you the way to the right food for you. And your path for better health.
 Your personal ImuPro Screen + documents Sample ID: 33333 Dear, With this letter, you will receive the ImuPro result for your personal IgG food allergy test. This laboratory report contains your results
Your personal ImuPro Screen + documents Sample ID: 33333 Dear, With this letter, you will receive the ImuPro result for your personal IgG food allergy test. This laboratory report contains your results
Module 5: Food Allergies and Intolerances
 A Preschool Nutrition Primer for Dietitians Module 5: Food Allergies and Intolerances Slide 1: A Preschool Nutrition Primer for Dietitians Module 5: Food Allergies and Intolerances The Nutrition Resource
A Preschool Nutrition Primer for Dietitians Module 5: Food Allergies and Intolerances Slide 1: A Preschool Nutrition Primer for Dietitians Module 5: Food Allergies and Intolerances The Nutrition Resource
RECOMMENDED PROTOCOL
 RECOMMENDED PROTOCOL St. Thecla is dedicated to keeping students with food allergies safe in the school environment. There is no one way to manage food allergies and each student s situation needs careful
RECOMMENDED PROTOCOL St. Thecla is dedicated to keeping students with food allergies safe in the school environment. There is no one way to manage food allergies and each student s situation needs careful
Improving allergy outcomes. IgE and IgG 4 food serology in a Gastroenterology Practice. Jay Weiss, Ph.D and Gary Kitos, Ph.D., H.C.L.D.
 Improving allergy outcomes IgE and IgG 4 food serology in a Gastroenterology Practice Jay Weiss, Ph.D and Gary Kitos, Ph.D., H.C.L.D. IgE and IgG4 food serology in a gastroenterology practice The following
Improving allergy outcomes IgE and IgG 4 food serology in a Gastroenterology Practice Jay Weiss, Ph.D and Gary Kitos, Ph.D., H.C.L.D. IgE and IgG4 food serology in a gastroenterology practice The following
Melbourne University Sport Anaphylaxis Policy
 Melbourne University Sport Anaphylaxis Policy The safety and well-being of children is of prime importance at Melbourne University Sport Programs. All reasonable steps will be taken to ensure the safety
Melbourne University Sport Anaphylaxis Policy The safety and well-being of children is of prime importance at Melbourne University Sport Programs. All reasonable steps will be taken to ensure the safety
FOOD ALLERGY IN SOUTH AFRICA Mike Levin
 FOOD ALLERGY IN SOUTH AFRICA Mike Levin Michael.levin@uct.ac.za SAFFA: The South African Food sensitisation and Food Allergy study Botha M, Basera W, Gray C, Facey-Thomas H, Levin ME. The Prevalence of
FOOD ALLERGY IN SOUTH AFRICA Mike Levin Michael.levin@uct.ac.za SAFFA: The South African Food sensitisation and Food Allergy study Botha M, Basera W, Gray C, Facey-Thomas H, Levin ME. The Prevalence of
Cow`s Milk Protein Allergy. COW`s MILK PROTEIN ALLERGY Eyad Altamimi, MD
 Cow`s Milk Protein Allergy COW`s MILK PROTEIN ALLERGY Eyad Altamimi, MD Agenda of the talk Definitions CMPA Epidemiology and Pathogenesis CMPA Diagnosis CMPA Management CMPA prevention Adverse Food Reaction
Cow`s Milk Protein Allergy COW`s MILK PROTEIN ALLERGY Eyad Altamimi, MD Agenda of the talk Definitions CMPA Epidemiology and Pathogenesis CMPA Diagnosis CMPA Management CMPA prevention Adverse Food Reaction
Diagnosis of Food Allergy by RAST
 Diagnosis of Food Allergy by RAST Donald R. Hoffman, Ph.D. Objective The purpose of this paper is to relate experience with RAST in the diagnosis of food allergy mediated by specific IgE antibodies. The
Diagnosis of Food Allergy by RAST Donald R. Hoffman, Ph.D. Objective The purpose of this paper is to relate experience with RAST in the diagnosis of food allergy mediated by specific IgE antibodies. The
Food allergy in children. Jan Sinclair Paediatric Allergy and Clinical Immunology Starship Children s Hospital
 Food allergy in children Jan Sinclair Paediatric Allergy and Clinical Immunology Starship Children s Hospital Aims Understand something of the epidemiology of childhood food allergy in NZ Review an approach
Food allergy in children Jan Sinclair Paediatric Allergy and Clinical Immunology Starship Children s Hospital Aims Understand something of the epidemiology of childhood food allergy in NZ Review an approach
St. Hugo of the Hills School Food Allergy Recommended Protocol
 St. Hugo of the Hills School Food Allergy Recommended Protocol St. Hugo of the Hills School is dedicated to keeping students with food allergies safe in the school environment. There is no one way to manage
St. Hugo of the Hills School Food Allergy Recommended Protocol St. Hugo of the Hills School is dedicated to keeping students with food allergies safe in the school environment. There is no one way to manage
Oral food challenge - Up to date. Philippe Eigenmann University Children s Hospital, Geneva CH
 Oral food challenge - Up to date Philippe Eigenmann University Children s Hospital, Geneva CH Food challenges belong to the stone age! Sampson HA et al. J Allergy Clin Immunol 2001: 107: 891-6 IgE cut-off
Oral food challenge - Up to date Philippe Eigenmann University Children s Hospital, Geneva CH Food challenges belong to the stone age! Sampson HA et al. J Allergy Clin Immunol 2001: 107: 891-6 IgE cut-off
Food allergy symptoms
 Allergic disorders such as asthma, hayfever and eczema have been increasing over the last 20 years. Food allergy is also on the increase and reactions are becoming more serious. Along with insect stings
Allergic disorders such as asthma, hayfever and eczema have been increasing over the last 20 years. Food allergy is also on the increase and reactions are becoming more serious. Along with insect stings
History of Food Allergies
 Grand Valley State University From the SelectedWorks of Jody L Vogelzang PhD, RDN, FAND, CHES Spring 2013 History of Food Allergies Jody L Vogelzang, PhD, RDN, FAND, CHES, Grand Valley State University
Grand Valley State University From the SelectedWorks of Jody L Vogelzang PhD, RDN, FAND, CHES Spring 2013 History of Food Allergies Jody L Vogelzang, PhD, RDN, FAND, CHES, Grand Valley State University
Medical Conditions Policy
 Medical Conditions Policy Background: Anaphylaxis is a severe, life-threatening allergic reaction. Up to two per cent of the general population and up to 5 percent of young children (0-5yrs) are at risk.
Medical Conditions Policy Background: Anaphylaxis is a severe, life-threatening allergic reaction. Up to two per cent of the general population and up to 5 percent of young children (0-5yrs) are at risk.
Food Allergy and Anaphylaxis
 Food Allergy and Anaphylaxis Professor Mimi Tang The Royal Children s Hospital, Melbourne Murdoch Childrens Research Institute, Melbourne University of Melbourne, Australia Food Allergy and Anaphylaxis
Food Allergy and Anaphylaxis Professor Mimi Tang The Royal Children s Hospital, Melbourne Murdoch Childrens Research Institute, Melbourne University of Melbourne, Australia Food Allergy and Anaphylaxis
FOOD ALLERGIES 12/17/2014 WHAT FOODS CAUSE ALLERGIES? AN ALLERGIC REACTION
 FOOD ALLERGY AWARENESS and EDUCATION IS IT FOOD INTOLERANCE, FOOD POISONING OR A FOOD ALLERGY? FOOD INTOLERANCE The inability to Metabolize or Process a Food Product Signs & Symptoms: Nausea, Stomach Pain,
FOOD ALLERGY AWARENESS and EDUCATION IS IT FOOD INTOLERANCE, FOOD POISONING OR A FOOD ALLERGY? FOOD INTOLERANCE The inability to Metabolize or Process a Food Product Signs & Symptoms: Nausea, Stomach Pain,
Allergies and Intolerances Policy
 Allergies and Intolerances Policy 2016 2018 This policy should be read in conjunction with the following documents: Policy for SEND/Additional Needs Safeguarding & Child Protection Policy Keeping Children
Allergies and Intolerances Policy 2016 2018 This policy should be read in conjunction with the following documents: Policy for SEND/Additional Needs Safeguarding & Child Protection Policy Keeping Children
Leander ISD Food Allergy Management Plan (FAMP)
 Leander ISD Food Allergy Management Plan (FAMP) Leander ISD s food allergy management plan has been developed according to Texas Education Code, EDUC 38.0151. Anaphylaxis is a sudden, severe, and potentially
Leander ISD Food Allergy Management Plan (FAMP) Leander ISD s food allergy management plan has been developed according to Texas Education Code, EDUC 38.0151. Anaphylaxis is a sudden, severe, and potentially
588-Complete Dietary Antigen Testing
 REPORT-1857 9 Dunwoody Park, Suite 121 Dunwoody, GA 3338 P: 678-736-6374 F: 77-674-171 Email: info@dunwoodylabs.com www.dunwoodylabs.com PATIENT INFO NAME: SAMPE PATIENT REQUISITION ID: 1857 SAMPE ID:
REPORT-1857 9 Dunwoody Park, Suite 121 Dunwoody, GA 3338 P: 678-736-6374 F: 77-674-171 Email: info@dunwoodylabs.com www.dunwoodylabs.com PATIENT INFO NAME: SAMPE PATIENT REQUISITION ID: 1857 SAMPE ID:
Food Allergy Acknowledgement
 Food Allergy Acknowledgement Campus Limitations: Due to the nature of our university style educational model where students, teachers, and staff come and go by periods of the day, and the inability to
Food Allergy Acknowledgement Campus Limitations: Due to the nature of our university style educational model where students, teachers, and staff come and go by periods of the day, and the inability to
SCHOOL SUPPORT STAFF CHECKLIST
 Food Allergy Management & Education SUPPORT STAFF SCHOOL SUPPORT STAFF CHECKLIST (Volunteers/Coaches, Extended Day Providers) Follow school district food allergy policy and procedure Participate in team
Food Allergy Management & Education SUPPORT STAFF SCHOOL SUPPORT STAFF CHECKLIST (Volunteers/Coaches, Extended Day Providers) Follow school district food allergy policy and procedure Participate in team
CME Disclosure Announcement
 Allergy & Asthma Specialists Educational Foundation BREATH VII Food Allergy Patrick Vannelli, MD March 31, 2017 Continuing Medical Education (CME) Credit This course offers 6 AMA Category 1 CME credit(s)
Allergy & Asthma Specialists Educational Foundation BREATH VII Food Allergy Patrick Vannelli, MD March 31, 2017 Continuing Medical Education (CME) Credit This course offers 6 AMA Category 1 CME credit(s)
PRESCHOOL Allergy & Medical Care Information School Year OVERVIEW
 PRESCHOOL Allergy & Medical Care Information 2017-2018 School Year OVERVIEW 1. Food Allergy Precautions If your child has severe food sensitivities and/or life threatening food allergies, complete and
PRESCHOOL Allergy & Medical Care Information 2017-2018 School Year OVERVIEW 1. Food Allergy Precautions If your child has severe food sensitivities and/or life threatening food allergies, complete and
Finding a Path to Safety in Food Allergy Highlights of the Consensus Report
 Finding a Path to Safety in Food Allergy Highlights of the Consensus Report 1 Disclosure Report of The National Academies of Sciences This activity was supported by Federal Sponsors: The Food and Drug
Finding a Path to Safety in Food Allergy Highlights of the Consensus Report 1 Disclosure Report of The National Academies of Sciences This activity was supported by Federal Sponsors: The Food and Drug
Anaphylaxis Policy. The symptoms of anaphylaxis can develop quickly although the initial presentation can be delayed and/or mild.
 Anaphylaxis Policy Anaphylaxis is a serious allergic reaction and can be life threatening. The allergic reaction may be related to food, insect stings, medicine, latex, exercise, etc., with the most common
Anaphylaxis Policy Anaphylaxis is a serious allergic reaction and can be life threatening. The allergic reaction may be related to food, insect stings, medicine, latex, exercise, etc., with the most common
REVISED 04/10/2018 Page 1 of 7 FOOD ALLERGY MANAGEMENT PLAN
 GARLAND INDEPENDENT SCHOOL DISTRICT HEALTH SERVICES Food Allergy Management Plan DEFINITIONS FOOD INTOLERANCE ALLERGIC REACTION SEVERE FOOD ALLERGY ANAPHYLACTIC REACTION FOOD ALLERGY MANAGEMENT PLAN (FAMP)
GARLAND INDEPENDENT SCHOOL DISTRICT HEALTH SERVICES Food Allergy Management Plan DEFINITIONS FOOD INTOLERANCE ALLERGIC REACTION SEVERE FOOD ALLERGY ANAPHYLACTIC REACTION FOOD ALLERGY MANAGEMENT PLAN (FAMP)
a) all students and staff with a life threatening allergy (anaphylaxis) are entitled to safe and healthy learning and working environments.
 Title: ANAPHYLACTIC REACTIONS Adopted: December 1, 2015 Reviewed: February 2018 Revised: Authorization: Sabrina s Law POLICY It is the policy of the Bloorview School Authority that: a) all students and
Title: ANAPHYLACTIC REACTIONS Adopted: December 1, 2015 Reviewed: February 2018 Revised: Authorization: Sabrina s Law POLICY It is the policy of the Bloorview School Authority that: a) all students and
Clinical Immunology and Allergy Fellowship Program Kuwait Institute for Medical Specialization
 Issued: June, 2011 Clinical Immunology and Allergy Fellowship Program Kuwait Institute for Medical Specialization I. INTRODUCTION The primary aim of the Allergy and Clinical Immunology Fellowship Program
Issued: June, 2011 Clinical Immunology and Allergy Fellowship Program Kuwait Institute for Medical Specialization I. INTRODUCTION The primary aim of the Allergy and Clinical Immunology Fellowship Program
FOOD ALLERGY AND ANAPHYLAXIS PROGRAM
 FOOD ALLERGY AND ANAPHYLAXIS PROGRAM Phoebe and Paul (above), both living with nut allergies, are among the many Canadian children that the SickKids Food Allergy and Anaphylaxis Program will benefit. Parents,
FOOD ALLERGY AND ANAPHYLAXIS PROGRAM Phoebe and Paul (above), both living with nut allergies, are among the many Canadian children that the SickKids Food Allergy and Anaphylaxis Program will benefit. Parents,
DR.RAJIV SHARMA BOOK SERIES 2
 DR.RAJIV SHARMA BOOK SERIES 2 CELIAC DISEASE AND GLUTEN 1 DR.RAJIV SHARMA CELIAC DISEASE AND GLUTEN GLUTEN IS LIKE AIR. ITS EVERYWHERE. As long as you have a beating heart you cannot avoid Gluten. Gluten
DR.RAJIV SHARMA BOOK SERIES 2 CELIAC DISEASE AND GLUTEN 1 DR.RAJIV SHARMA CELIAC DISEASE AND GLUTEN GLUTEN IS LIKE AIR. ITS EVERYWHERE. As long as you have a beating heart you cannot avoid Gluten. Gluten
FEEDING THE ALLERGIC CHILD
 FEEDING THE ALLERGIC CHILD Berber Vlieg-Boerstra, RD PhD Senior research dietitian OLVG, Amsterdam University of Applied Sciences, Groningen Vlieg&Melse Dietitians, Practice for food allergy Disclose NO
FEEDING THE ALLERGIC CHILD Berber Vlieg-Boerstra, RD PhD Senior research dietitian OLVG, Amsterdam University of Applied Sciences, Groningen Vlieg&Melse Dietitians, Practice for food allergy Disclose NO
GI Allergy and Tolerance. Jon A. Vanderhoof, M.D. Division of Gastroenterology/Nutrition Boston Children s Hospital Harvard Medical School
 GI Allergy and Tolerance Jon A. Vanderhoof, M.D. Division of Gastroenterology/Nutrition Boston Children s Hospital Harvard Medical School Disclosure Medical Advisor- Mead Johnson Nutrition Food Allergy
GI Allergy and Tolerance Jon A. Vanderhoof, M.D. Division of Gastroenterology/Nutrition Boston Children s Hospital Harvard Medical School Disclosure Medical Advisor- Mead Johnson Nutrition Food Allergy
See Policy CPT CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: LAB Policy No: 404 Medical Policy Committee Approved Date: 12/17; 12/18 1/1/19 Medical Officer Date APPLIES TO: All lines of business See Policy CPT CODE section below
Effective Date: 1/1/2019 Section: LAB Policy No: 404 Medical Policy Committee Approved Date: 12/17; 12/18 1/1/19 Medical Officer Date APPLIES TO: All lines of business See Policy CPT CODE section below
Advisor. The Asthma. enter. Education and Research Fund. Types of food intolerance (non-allergic) Natural history of food allergy. theasthmacenter.
 The Asthma C enter Education and Research Fund Advisor theasthmacenter.org F D AllergY Introduction Food allergies are often blamed for any adverse reactions before or during the ingestion of a specific
The Asthma C enter Education and Research Fund Advisor theasthmacenter.org F D AllergY Introduction Food allergies are often blamed for any adverse reactions before or during the ingestion of a specific
Dietary management of food allergy & intolerance
 Dietary management of food allergy & intolerance Dr Emilia Vassilopoulou BsC, PhD, Post-Doc Clinical Nutritionist Dietitian Food Allergy An adverse immune response to a food protein Reactions to a food
Dietary management of food allergy & intolerance Dr Emilia Vassilopoulou BsC, PhD, Post-Doc Clinical Nutritionist Dietitian Food Allergy An adverse immune response to a food protein Reactions to a food
It s Not Just Peanut Butter Food Allergies in Early Childhood Education. Marcy Davidson CAEYC Professional Conference March 17, 2012
 It s Not Just Peanut Butter Food Allergies in Early Childhood Education Marcy Davidson CAEYC Professional Conference March 17, 2012 Manny Manny s favorite toy cars Manny s favorite friend Tyler Manny s
It s Not Just Peanut Butter Food Allergies in Early Childhood Education Marcy Davidson CAEYC Professional Conference March 17, 2012 Manny Manny s favorite toy cars Manny s favorite friend Tyler Manny s
What is a Food Allergen?
 What is a Food Allergen? An abnormal or pathological reaction to food substances in amounts that do not affect most people. Foods contain protein and an allergic reaction occurs when the body s immune
What is a Food Allergen? An abnormal or pathological reaction to food substances in amounts that do not affect most people. Foods contain protein and an allergic reaction occurs when the body s immune
November Laboratory Testing for Celiac Disease. Inflammation in Celiac Disease
 November 2011 Gary Copland, MD Chair, Department of Pathology, Unity Hospital Laboratory Medical Director, AMC Crossroads Chaska and AMC Crossroads Dean Lakes Laboratory Testing for Celiac Disease Celiac
November 2011 Gary Copland, MD Chair, Department of Pathology, Unity Hospital Laboratory Medical Director, AMC Crossroads Chaska and AMC Crossroads Dean Lakes Laboratory Testing for Celiac Disease Celiac
FOOD ALLERGY GUIDELINES FOR SCHOOLS. Training Module
 FOOD ALLERGY GUIDELINES FOR SCHOOLS Training Module GOAL Create an environment where children with food allergies will be safe Employ prevention and avoidance strategies-education education is key Be prepared
FOOD ALLERGY GUIDELINES FOR SCHOOLS Training Module GOAL Create an environment where children with food allergies will be safe Employ prevention and avoidance strategies-education education is key Be prepared
Food Triggers: The Degree of Avoidance
 Food Triggers: The Degree of Avoidance Marion Groetch, MS, RDN marion.groetch@mssm.edu Director of Nutrition Services, Jaffe Food Allergy Institute Icahn School of Medicine American Academy of Allergy,
Food Triggers: The Degree of Avoidance Marion Groetch, MS, RDN marion.groetch@mssm.edu Director of Nutrition Services, Jaffe Food Allergy Institute Icahn School of Medicine American Academy of Allergy,
Report No. 3 of the Health and Emergency Medical Services Committee Regional Council Meeting of April 27, SABRINA'S LAW
 1 SABRINA'S LAW The Health and Emergency Medical Services Committee recommends the adoption of the recommendation contained in the following report, March 9, 2006, from the Commissioner of Community Services,
1 SABRINA'S LAW The Health and Emergency Medical Services Committee recommends the adoption of the recommendation contained in the following report, March 9, 2006, from the Commissioner of Community Services,
Am I a Silly Yak? Laura Zakowski, MD. No financial disclosures
 Am I a Silly Yak? Laura Zakowski, MD No financial disclosures Patient NP 21 year old male with chronic headaches for 6 years extensively evaluated and treated Acupuncturist suggests testing for celiac
Am I a Silly Yak? Laura Zakowski, MD No financial disclosures Patient NP 21 year old male with chronic headaches for 6 years extensively evaluated and treated Acupuncturist suggests testing for celiac
Early Allergen Introduction & Prevention of Food Allergy
 Early Allergen Introduction & Prevention of Food Allergy Burcin Uygungil, MD, MPH Division of Allergy and Immunology Children s National Health System (adapted from Sharma 2016) Discussion Objectives Review
Early Allergen Introduction & Prevention of Food Allergy Burcin Uygungil, MD, MPH Division of Allergy and Immunology Children s National Health System (adapted from Sharma 2016) Discussion Objectives Review
Food Challenges. Exceptional healthcare, personally delivered
 Food Challenges Exceptional healthcare, personally delivered Introduction You have been referred to the Immunology department to explore your food allergies. This leaflet provides information on allergies
Food Challenges Exceptional healthcare, personally delivered Introduction You have been referred to the Immunology department to explore your food allergies. This leaflet provides information on allergies
Up to Date on Food Allergies
 Up to Date on Food Allergies Robyn Morrissette, PA-C Division of Allergy and Immunology 10/5/18 Learning Objectives To understand the various types of food allergies, based on underlying immunologic mechanisms.
Up to Date on Food Allergies Robyn Morrissette, PA-C Division of Allergy and Immunology 10/5/18 Learning Objectives To understand the various types of food allergies, based on underlying immunologic mechanisms.
