CHAPTER 33 CELIAC DISEASE. Riccardo Troncone and Salvatore Auricchio. Celiac disease (CD), also called gluten-sensitive enteropathy, is a permanent
|
|
|
- Imogene Moore
- 5 years ago
- Views:
Transcription
1 CHAPTER 33 CELIAC DISEASE Riccardo Troncone and Salvatore Auricchio DEFINITION Celiac disease (CD), also called gluten-sensitive enteropathy, is a permanent intestinal intolerance to dietary wheat gliadin and related proteins that produces mucosal lesions in genetically susceptible individuals. HISTORICAL BACKGROUND CD was first accurately described by Samuel Gee in 1888, but it was not until the early 1950s that Dicke in Holland established the role of wheat and rye flour in the pathogenesis of the disease and identified the protein known as gluten as the harmful factor in those cereals (1). A major contribution to the understanding of the disease came from the development of methods for peroral biopsy of the jejunal mucosa, which allowed definition of the mucosal lesion (2), and from the definition of diagnostic criteria published in 1969 by the European Society of Paediatric Gastroenterology and Nutrition (ESPGAN) (3). In recent years a substantial amount of data have been produced that have profoundly changed our understanding of epidemiology, clinical aspects and pathogenesis of CD, opening new perspectives for treatment. 1
2 CEREAL PROTEINS AND OTHER ENVIRONMENTAL FACTORS Cereal Proteins The cereals that are toxic for patients with CD are wheat, rye, and barley; rice and maize are non-toxic and are usually used as wheat substitutes in the diet of patients with CD. The toxicity of oats has been reassessed in recent years. It has in fact been shown that the use of oats as part of a gluten-free diet has no unfavourable effects on adult patients in remission and does not prevent mucosal healing in patients with newly diagnosed disease (4, 5). Nonetheless, a few celiacs seem not to tolerate oats, showing raised levels of intestinal interferon gamma mrna after challenge (6); furthermore, the fear that small amounts of gliadin could contaminate oats, suggests caution before the inclusion of oats is advocated in the diet of celiac patients. Cereal grains belong to the grass family (Gramineae). Grains considered toxic for celiac patients (rye, barley, and, to a lesser extent, oats) bear a close taxonomic relationship to wheat, whereas nontoxic grains (rice and maize) are taxonomically dissimilar (Fig. l). Wheat seed endosperm contains heterogeneous protein classes differentiated, according to their extractability and solubility in different solvents, into albumins, globulins, gliadins, and glutenins. Gliadins are monomers, whereas glutenins form large polymeric structures. Gliadins have been classified according to their N terminal amino acid sequences into alpha, gamma and omega types; glutenins are subdivided into high molecular weight glutenins and low molecular weight glutenins. The wheat toxicity results from the gliadin protein fraction, and the toxicity of cereals other than wheat is most likely associated with prolamin fractions equivalent to 2
3 gliadins in the grain of these other species; on the other hand, glutenin peptides have been shown to be immunogenic for mucosal T cells from celiac patients (7). The amino acid sequence(s) responsible for the disease have not been fully elucidated, also because different part of the gliadin molecules show different biological properties, all potentially involved in the pathogenesis of the disease; several HLA- DQ2 restricted T cell epitopes have been found clustering in regions of gliadin rich in proline residues (8), target of the tissue transglutaminase (TG2) deamidating activity (see pathogenesis); other sequences have been shown to activate innate immunity mechanisms (9), or interact with CD8+ cytotoxic T cells (10). Organ culture systems have validated the biological activity of some of these sequences, but there is no doubt that in vitro methodology must be paralleled by in vivo challenge studies. In fact, histologic changes have been shown to occur in the celiac intestinal mucosa after challenge with synthetic peptides encompassing the (11), and (12), and, more recently, the sequence of A-gliadin (13). Other Environmental Factors The high concordance rate for monozygotic twins, and the similar risk shown by dyzigotic twins and other siblings, suggest that a shared environment (gluten antigen aside) has little or no effect (14). On the other hand, the relevance of environmental factors other than gluten in CD is suggested by the significant changes in the incidence of the disease by time and place. Feeding practices seem to be relevant. Recently, Sweden has experienced an epidemic of symptomatic celiac disease in 3
4 children aged less than two years; the abrupt increase and decline in the incidence of the disease coincided with changes in the dietary pattern of infants (15). The risk of coeliac disease was found to be greater when gluten was introduced in the diet in large amounts (16); on the contrary, it was reduced if children were still breastfed when dietary gluten was introduced (16). This finding add to previous case referent studies showing that breast feeding is protective, while the age of introduction of gluten in infants diet has no effect on risk (17). An important question is whether favourable dietary habits simply postpone the onset of celiac disease, or reduce the overall lifetime risk of the disease; a challenging possibility that requires further studies is that celiac disease might be delayed, or even prevented, intervening in genetically susceptible individuals on dietary patterns of the first year of life. Among other environmental factors that could play a possible role in CD, infective factors have also been considered. The possible role played in pathogenesis by alpha interferon (18), and the epidemiological evidence of increased risk in relation to the month of birth (19), have suggested the possible involvement of a viral infection, but no evidence has so far supported this hypothesis. GENETICS OF CELIAC DISEASE Family Studies Susceptibility to CD is determined to a significant extent by genetic factors. That is suggested by the occurrence of multiple cases in families, the prevalence of CD found among first-degree relatives being approximately 10% (20). Moreover, as 4
5 many as 75% of monozygotic twins have been found to be concordant with the disease (14). The concordance rate among HLA-identical siblings is about 30%, indicating that a significant part of the genetic susceptibility maps to the HLA region on chromosome 6. Genetic Markers The strongest association of CD is with the HLA class II D region markers, class I and class II region gene associations being secondary to linkage disequilibrium. It has been suggested that the primary association of CD is with the DQ αβ heterodimer encoded by the DQA1 *05 and the DQB1*02 genes (21). Such a DQ molecule has been found to be present in 95% or more of celiac patients compared with 20% to 30% of controls. The data available on DQ2-negative celiac patients indicate that they almost invariably are HLA DQ8 positive (DQA1*0301/DQB1*0302) (22). A gene dosage effect has been suggested, and a molecular hypothesis for such phenomenon has been proposed based on the impact of the number and quality of the HLA DQ2 molecules on gluten peptide presentation to T cells (23). The most likely mechanism to explain the association with HLA class II genes is, in fact, that the DQ molecule binds a peptide fragment of an antigen involved in the pathogenesis of CD to present it to T cells. Other non-hla genes could confer susceptibility to CD. Considering the relevance of the immune response in the pathogenesis of the disease, candidate genes are those influencing the T cell response. Among those, several reports imply involvement of 5
6 the gene for the negative costimulatory molecule CTLA4 or a neighbouring gene (24). A series of whole genome screening studies have been performed in CD (25). The region that has most consistently been linked to CD is on the long arm of chromosome 5 (5q 31-33) (25). There is also evidence for susceptibility factors on the chromosomes 11q (26) and 19 (27). EPIDEMIOLOGY The reported prevalence of symptomatic CD is l in 1000 live births, with a range from l in 250 (observed in Sweden) to l in 4000 (observed in Denmark) (28). The prevalence in women appears to be greater than in men. Population based screening studies have clearly shown that CD is underdiagnosed, clinical CD representing the top of the iceberg. A recent Finnish study has shown that the prevalence of biopsy proven CD is at least 1: 99 (29) children, indicating CD as one of the most common genetically based disease. Similar prevalence have been indicated in most European Countries, in North Africa, in South America and in USA (30). Even when there is no policy for actually screening the entire population, the pick-up rate of coeliac patients within a health care system can be greatly increased by general awareness of the protean clinical manifestations of CD. By a policy of aggressive serological testing of family members and other at risk groups (Table 6
7 33.1), and by carrying out duodenal biopsy in every patient who has an upper GI endoscopy, a prevalence of CD similar to that emerged from mass screening studies has been revealed (31). PATHOGENESIS Coeliac disease is a T cell mediated chronic inflammatory disorder with an autoimmune component. It is likely that the loss of tolerance is somewhat related to the peculiar physicochemical properties of gliadin. Altered processing by intraluminal enzymes, changes in intestinal permeability, activation of innate immunity mechanisms precede the activation of the adaptive immune response. Both epithelium and lamina propria are places where the immune response takes place (Fig 2). Low digestibility of gliadin In the brush border of enterocytes are present enzymes able to hydrolyse peptide bonds containing proline (and glutamic acid); these enzymes show in treated celiac patients an activity comparable to that exhibited by controls (32). On the other hand, immunodominant epitopes from gliadin are highly resistant to intraluminal and mucosal digestion (33,34), although they are largely hydrolysed during the transport through the small intestinal mucosa (35); the hydrolysis is reduced only during the passage through the atrophic celiac mucosa (35). It is possible to hypothesize that incomplete degradation favour the immunostimulatory and toxic effects of these sequences. 7
8 Activation of innate immunity Gliadin has the ability to induce a complete activation of the immune system (adaptive and innate). In fact, in the treated celiac mucosa only the nonimmunodominant peptide (and not the peptide 56-68) induce rapid activation of the innate immune system, as revealed by rapid, IL-15, CD83 (a marker of mature dendritic cells), COX-2 (an enzyme rapidly induced during inflammation), and CD 25 expression by CD3- cells (non T-cells) of the innate immune system (9). A particular gliadin fragment, therefore, activates the innate immune system timing the in situ T cell recognition of dominant gliadin epitopes. Lamina propria gliadin specific CD4+ activation The activation of lamina propria T cells by gliadin peptides in the contest of HLA- DQ2 or DQ8 molecules has been long recognised as one of the key events in pathogenesis of CD. A large number of T-cell stimulating peptides have been characterized in gluten proteins (7). Studies by Sollid and Koning have provided a model explaining the interplay between gliadin, DQ2 or DQ8 and TG2. In fact, these gliadin-specific T-cell responses have been found to be enhanced by the action of TG2 (36); the enzyme converts particular glutamine residues into glutamic acid, which results in higher affinity of these gliadin peptides for HLA-DQ2 or HLA-DQ8. The pattern of cytokines produced following gliadin activation is clearly dominated by γ IFN (Th1 skewed), but unexpectedly IL12 is not expressed. IL18 (37) and interferon alpha (18) are both candidate as driving factors for Th1 differentiation and gamma interferon production. The signalling pathway related to gamma interferon 8
9 has also been explored: persistent STAT1 activation was observed (38) as well as enhanced interferon regulations factor 1 (IRF1) expression (39). IL10 is also increased, but not enough to control the strong gamma IFN production (40). Downstream T cell activation, a complex remodelling of the mucosa takes place, involving increased levels of metalloproteinases (41) and growth factors (42) which leads to the classical flat mucosa. Intraepithelial lymphocytes Intraepithelial lymphocytes are a hallmark of CD. Mechanisms other than lamina propria T cell activation are likely to be responsible for their recruitment. Alterations of intestinal epithelium occur in untreated CD; MIC and HLA-E are induced in response to stress and gamma interferon, or to gluten itself. MIC and HLA-E are recognised by NK receptors (NKG2D and CD94) present on intraepithelial lymphocytes and up-regulated by IL15 (43). More recently a direct recognition of gliadin peptides by CD8+ lymphocytes has also been demonstrated (10). Activation of intraepithelial lymphocytes is likely to contribute to epithelial cell apoptosis and villous atrophy via FAS/FAS ligand (44) and perforin-granzyme (45) pathways. Coeliac disease and autoimmunity This Th1 skewed immunological picture is common to other conditions of organ autoimmunity; moreover, in recent years, the demonstration of autoimmune phenomena and the strict association with other autoimmune diseases have favoured the inclusion of CD itself in the number of autoimmune diseases. The most evident 9
10 expression of autoimmunity is the presence of serum antibodies to tissue transglutaminase (TG2) (46). Tests based on the measurement of IgA antibodies to the enzyme discriminates very efficiently coeliac patients (see diagnosis). As far as mechanisms of damage are concerned, antibodies to TG2 inhibit its activity in a dose dependent manner, both in vitro and in situ, although the inhibition is only partial (47). In in vitro models it has been shown that such antibodies interfere with differentiation of epithelial cells, probably disturbing TGF beta-mediated epithelialfibroblast crosstalk (48). Several evidences suggest that TG2 autoantibodies are primarily produced in the gut mucosa of celiac patients (49), where they can be detected before they appear in the circulation. The finding of IgA deposits on extracellular TG2 in the liver, lymphnodes and muscles indicates that TG2 is accessible to the gut-derived autoantibodies (50). Several extraintestinal clinical manifestations of CD (e.g. liver, heart, nervous system) are possibly related to the presence of autoantibodies in situ. The mechanisms leading to autoimmunity are largely unknown. Upregulation of TG2 in inflamed sites may generate additional antigenic epitopes by crosslinking or deamidating external or endogenous proteins. Unmasking of cryptic epitopes has also been hypothesized in the context of an inflamed environment where antigen processing and presentation may be more efficient. Finally, help for the production of autoantibodies given by gliadin-specific T cells in the mucosa has been advocated to explain why these autoantibodies are dependent on the presence of gluten in the diet (51). TG2 are not the only autoantibodies present in CD: antibodies to actin (52) and to calreticulin (53) have 10
11 been detected in celiac sera. New autoantigens (enolase, ATP synthase beta chain) have recently been identified by mass fingerprinting approach (54). PATHOLOGY CD manifests itself pathologically as a disease of the small intestine. A distinct pattern of abnormalities has been observed; the features include l) partial to total villous atrophy; 2) elongated crypts; 3) increased mitotic index in the crypts; 4) increased intraephitelial lymphocytes (IELs); 5) infiltrations of plasma cells and lymphocytes as well as mast cells, eosinophils, and basophils in the lamina propria; and 6) absence of identifiable brush border and abnormalities in the epithelial cells, which become flattened, cuboidal, and pseudostratified. However, these changes are not pathognomic of CD, and most of them may be seen in other entities, such as cow's milk or soy protein hypersensitivity, intractable diarrhea of infancy, heavy infestation with Giardia lamblia, primary immunodeficiencies, tropical sprue, bacterial overgrowth, and intestinal lymphoma. Hence, it is crucial to establish the gluten dependence of the jejunal lesion. It has now become clear that, from a pathological point of view, the small intestinal enteropathy in celiac disease may be of variable severity. A spectrum of pathological changes of increasing severity, ranging from a mild picture characterized by infiltration of the epithelium by lymphocytes, to crypt hyperplasia, to villous atrophy. In cases presenting with mild enteropathy immunohistochemical analysis has gained importance. Signs of activated mucosal cell mediated immunity (enhanced epithelial 11
12 expression of HLA -DR and -DP, increased density of CD25 positive cells) have been found in jejunal biopsies, for instance in first degree relatives of coeliac patients, considered for that to be potential coeliacs (55). More specific for coeliac disease, but both sensitivity and specificity far from being absolute, is the finding of increased density of intraepithelial lymphocytes with gamma/delta T cell receptor (56) (Fig 3). Nonetheless, these investigations are available only in specialised laboratories. In the presence of very mild signs of small intestinal enteropathy, such as the increased density of intraepithelial lymphocytes or the presence of immunohistochemical signs of T cell activation, the demonstration of the gluten dependence of such signs becomes central, in other words their disappearance after a period of gluten free diet; but this is not always easy to demonstrate (57). CLINICAL PRESENTATION Clinical features of CD differ considerably. Intestinal symptoms are common in children diagnosed within the first two years of life; failure to thrive, chronic diarrhoea, vomiting, abdominal distension, muscle wasting, anorexia and irritability are present in most cases. With the shifting of the age at presentation of the disease later in childhood, and with the wider and more liberal use of serological screening tests, extra-intestinal manifestations, without any accompanying digestive symptom, have increasingly been recognized, affecting almost all organs. Short stature has probably been the first isolated extraintestinal presentation of CD to be recognized; already in the early 80s, approximately 10% of patients with 12
13 isolated short stature undergoing jejunal biopsy were found to have a total villous atrophy (58). Nonetheless, both in children and in adults, the most frequent extraintestinal manifestation of CD is iron-deficiency anemia (59). The prevalence of CD in adult patients with microcytic anemia unresponsive to iron therapy is as high as 8.5% (60). As far as the locomotor apparatus is concerned, arthritis and arthralgia as presentation symptoms of CD were described by Maki (61). A screening study using determination of antigliadin antibodies in patients with idiopathic osteoporosis has shown an incidence of CD ten-fold higher than in healthy people (62). As a matter of fact the majority of adult coeliac patients suffer from metabolic osteopathy; gluten free diet normalizes bone mass only in a proportion of subjects. Patients whose CD was diagnosed in childhood and who have since then been receiving gluten free diet have a bone mineral density similar to that of healthy controls (63). The nervous system is also involved in CD. An Italian report has proposed an association between CD and epilepsy in patients with bilateral occipital calcifications (64) (Fig 4); in such patients gluten-free diet beneficially affects the course of epilepsy only when started soon after epilepsy onset. Moreover, gluten sensitivity is proposed to be common in patients with neurological diseases of unknown etiology. One example is gluten ataxia (65), a recently described condition, which seems to affect 60% of unclassified ataxia and which is identified on the basis of high serum titres of antigliadin antibody; up to 40% of them are coeliacs. Peripheral neuropathies of axonal and demyelinisating types have also been reported and may respond to elimination of gluten from the diet. There is no doubt that the liver is a target of gluten toxicity in 13
14 CD. Isolated hypertransaminasemia has been recognized as a possible presentation of CD; it may be expression of chronic "cryptogenic" hepatitis resolving on a glutenfree diet (66). As 4% of patients with cryptogenic hepatitis are affected by otherwise silent CD, serological screening for CD is mandatory in such patients (67). Recently, patients with severe liver disease have been described in whom gluten-free diet prevented progression to hepatic failure, even in cases in which liver transplantation was considered (68). Patients having fertility problems may have subclinical CD: unexplained infertility may be the only sign of CD (69). Similarly, unfavourable outcome of pregnancy such as recurrent abortions, or premature delivery, or low weight at birth, are more often observed in undiagnosed or untreated CD patients (70). Different degrees of dental abnormalities have been described in children with CD; severe enamel hypoplasia is present in up to 30 percent of untreated CD children (71). Alopecia areata has been reported to be the only clinical manifestation of CD (72). A special place in this list is taken by dermatitis herpetiformis (DH), a gluten dependent condition characterized by a symmetric pruritic skin rash with subepidermal blisters and granular subepidermal deposits of IgA in remote uninvolved skin. Most patients with DH have abnormal small intestinal biopsy pathology, histologically indistinguishable from that of CD, although usually less severe. Approximately 60% of children with DH have been reported to have subtotal villous atrophy, and 30% have partial villous atrophy on jejunal biopsy (73). The histologic changes return to normal after dietary exclusion of gluten. Therapy with 14
15 dapsone usually leads to prompt clinical improvement; a strict gluten-free diet permits a reduction or discontinuation of dapsone over a period of months. Improvement of skin lesions on a gluten-free diet seems to occur also in patients with no evident mucosal abnormality; in the same patients the rash recurs with a gluten rechallenged. Different may be the mechanisms operating in these different situations. Such extradigestive manifestations may more likely result from the intestinal damage and consequent nutritional deficiencies (e.g. anemia, osteopenia) and/or due to the deranged (auto?)immune response (e.g. skin, liver, joints, CNS involvement). ASSOCIATED DISEASES Some diseases, many with an autoimmune pathogenesis, are found with a higher than normal frequency in celiac patients; among these are thyroid diseases (74), Addison's disease (75), pernicious anemia (76), autoimmune thrombocytopenia (77), sarcoidosis (78), insulin-dependent diabetes mellitus (79), alopecia (80) and cardiomyopathies (81). Such associations have been interpreted as a consequence of the sharing of identical HLA haplotypes (e.g., B8, DR3). Nevertheless, the relation between CD and autoimmunity is more complex. In CD patients there is evidence that the risk of developing autoimmune diseases seems to be directly correlated to the duration of gluten exposure (82). An increased incidence of CD has been found in Down syndrome patients compared with the general population (83). Similarly in Turner s syndrome and Williams 15
16 syndrome higher number of CD cases was also observed (84,85). Selective IgA deficiency is also a condition associated with celiac disease (86). Screening test alternatives to those based on the measurement of IgA isotype antibodies must be adopted in such patients. LABORATORY FINDINGS Tests for Malabsorption and permeability Tests for malabsorption may be of help in approaching the diagnosis of CD. Determination of hemoglobin, serum iron, calcium, phosphorus, alkaline phosphatase, magnesium, and protein levels may be indicative of malabsorption. In particular, red blood cell folate levels have been found to be a sensitive index (20) Prothrombin levels should be checked in any case before intestinal biopsy is performed. Over the last few years, tests based on intestinal permeability to sugars have been found of value as a noninvasive screening tool. Most of them are based on the differential intestinal absorption of two nonmetabolized sugars. In untreated CD the absorption of the smaller probe (mannitol, rhamnose) is reduced owing to the loss of intestinal surface area, and that of the larger one (lactulose, cellobiose) is reported as increased, because paracellular pathways are "leakier" and/or increased in number. Expression of the results as a ratio of disaccharide: monosaccharide recovery gives clear separation between normal cases and patients with CD (87,88). Although this test has a sufficient sensitivity for abnormalities of jejunal mucosa, it is also 16
17 characterized by a low specificity for CD and false-positive results occurring mainly in patients with mucosal abnormalities due to other causes (e.g., Crohn's disease, atopic eczema, food allergy, and damage induced by nonsteroidal anti-inflammatory agents). Serological Tests Serological tests have also acquired a strong importance, in particular the search for antiendomysial antibodies; more recently, after the demonstration that tissue transglutaminase is the main autoantigen recognised by endomysial antibodies (46), antitissue transglutaminase antibodies have shown a great sensitivity and specificity for the diagnosis of celiac disease (89) (Table 33.2). The specificity is almost absolute also considering that subjects with positive serum endomysial antibodies and normal histology have a high chance to develop enteropathy in the following years (90). On the other hand, a note of caution comes from studies in adult patients indicating a lower sensitivity, particularly in subjects with milder form of enteropathy (91). In the last years after first generation test based on the use of guinea pig antigen, the most recent assays, based on the use of recombinant human enzyme as coating antigen in ELISA, have further improved the diagnostic efficacy. We can expect further improvement by the definition of the epitopes of tissue transglutaminase recognised by coeliac sera (49). However, a series of technical problems common to other ELISA tests still are present, for example the correct definition of cut-off values. Furthermore, while it has now been clearly shown that the site of production 17
18 of endomysial and tissue transglutaminase antibodies is the gut mucosa (92), and that their presence in the serum is the result of their spill-over, is more than a working hypothesis the possibility that there are seronegative subjects with presence of such antibodies only in their intestinal secretions (93). HLA As already mentioned, coeliac disease is strongly associated with some HLA allele specificities, namely those serologically recognised as HLA DQ2 (90-95% of cases) and HLA DQ8 (approximately 5% of cases); less than 2% of coeliac patients lack both HLA specificities; at the same time approximately one third of our normal population has one or the other marker; that means that the demonstration of being DQ2 and/or DQ8 positive has a strong negative predictive value, but a very weak positive predictive value for the diagnosis of coeliac disease. With these limitation the test may prove useful to exclude coeliac disease in subjects on a gluten-free diet, or in subjects belonging to at risk group (eg first degree relatives, insulin-dependent diabetics, patients with Down s syndrome) to avoid long term follow-up. Simplified methods based on molecular typing of only the alleles associated to coeliac disease have been set up (94). DIAGNOSIS The two requirements mandatory for the diagnosis of CD remain: 1) the finding of villous atrophy with hyperplasia of the crypts and abnormal surface epithelium, while 18
19 the patient is eating adequate amounts of gluten; and 2) a full clinical remission after withdrawal of gluten from the diet. The finding of circulating IgA antibodies to gliadin, reticulin, and endomysium at the time of diagnosis, and their disappearance on a gluten-free diet, adds weight to the diagnosis. A control biopsy to verify the consequences on the mucosal architecture of the gluten- free diet is considered mandatory only in patients with equivocal clinical response to the diet and in patients asymptomatic at first presentation (as is often the case in patients diagnosed during screening programs, e.g., first-degree relatives of celiac patients) (95). Gluten challenge is not considered mandatory, except under unusual circumstances. These include situations where there is doubt about the initial diagnosis, for example when no initial biopsy was done, or when the biopsy specimen was inadequate or not typical of CD. Gluten challenge should be discouraged before the age of 7 years and during the pubertal growth spurt. Once decided, gluten challenge should always been performed under strict medical supervision. It should be precedend by an assessment of mucosal histology and performed with a standard dose of at least 10 g of gluten per day without disrupting established dietary habits. A further biopsy is taken when there is a noticeable clinical relapse or, in any event, after 3 to 6 months. Serologic tests (IgA gliadin, reticulin and endomysium antibodies, absorptive and permeability tests), more than clinical symptoms, can be of help in assessing the timing of the biopsy to shorten the duration of the challenge (96). In a situation where jejunal histology has lost specificity, and with the growing 19
20 contribution by serology, and to a less extent by HLA, many propose to move to a new diagnostic approach mainly based on antibodies and genetics. Nonetheless, the contribution of the analysis of jejunal biopsies may still be very important; in particular the study of the intestinal mucosa could prove decisive in the definition of the disease state. In fact, considering that more than 30% of the population has the HLA alleles implicated in celiac disease and more than 1% a positive serology, with an increasing number of subjects showing signs of minor enteropathy, the same definition of disease and the consequent need of a gluten free diet still awaits a definitive response. It is quite clear that subjects with severe gluten dependent enteropathy face a series of health risks, mainly nutritional; they probably have also higher risk of developing autoimmunity, and, although less than previously thought, of presenting neoplastic complications. On the contrary, little is known of those with minor enteropathy, maybe silent from a clinical point of view, for instance subjects belonging to groups such as first degree relatives or insulin-dependant diabetics. A recent report (57) showing nutritional deficiencies also in patients with minor enteropathy, positive serology and right genetics, resolving on a gluten free diet, seems to indicate in all these subjects the need for a gluten free diet. Prospective studies are necessary. Until serological methods are improved, the genetic make up of celiac patients is better defined, it seems wise for a diagnosis of coeliac disease still rely on a combined approach based of clinical criteria, histology, serology and genetics. 20
21 THERAPY Gluten-Free Diet Since the identification of gluten as etiologic factor in CD, a strict gluten-free diet has become the cornerstone of the management of such patients. Their diet should exclude wheat, rye, and barley; the inclusion of oats is still debated, because the toxicity has not been definitively disproved and because of the fear that small amounts of gliadin could contaminate oats; rice and maize are nontoxic and are usually used as wheat substitutes. The clinical response to withdrawal of gluten is often dramatic, but it must be stressed that the gluten-free diet is recommended for both symptomatic and asymptomatic patients with CD. Normalization of the jejunal histology occurs after about 6 months. The most likely cause of lack of response is failure to adhere strictly to the diet, but the possibility of sensitivity to other dietary proteins, lymphoma, and immunodeficiency should also be considered. All the present evidence strongly supports the view that restriction of gliadin and related prolamines should be complete and for life for all patients. A gluten-free diet is thought to be protective against the development of maligned disease. Patients with celiac disease have a risk of small bowel adenocarcinoma that is about 80-fold greater than that of the general population (97). The predominant celiac-associated lymphoma is the enteropathy-associated T-cell lymphoma, which doses not respond well to chemotherapy and is rapidly fatal (98). Malignancies are not the only risk that celiac patients not compliant with gluten-free diet are exposed to; nutritional 21
22 deficiencies (99), osteoporosis, and more recent evidence that the risk of developing autoimmune diseases is related to the duration of exposure to gluten are additional concerns (82). Other Therapeutic Measures Specific vitamin, mineral, and trace element deficiencies should be corrected. Replacement therapy can generally be discontinued after clinical and histologic recovery on gluten- free diet has been documented. Other dietary measures are rarely needed. The disaccharidase activity is greatly depressed in atrophic celiac mucosa, but it is advisable to remove milk and lactosecontaining products only if intolerance is clinically manifest. Secondary lactase deficiency resolves rapidly after institution of a gluten-free diet, and milk can usually be tolerated after 2 to 4 weeks of the diet. When patients present in celiac crisis, rapid correction of volume depletion and fluid and electrolyte abnormalities is crucial; steroid therapy is helpful. Short-term administration of steroids (2 mg/kg per 24 hours of prednisone for 1-2 weeks) may also be used in severely ill infants in whom anorexia and malabsorption do not rapidly respond to the gluten-free diet. Therapeutic strategies for the future. Significant progress has been made in recent years in the understanding of the cellular and molecular basis of CD and in the consequent identification of possible targets for therapy. Recently it has been shown that, because of the high 22
23 proline content, gliadin peptides are highly resistant to digestive processing by pancreatic and brush border proteases. Enzyme supplement therapy using bacterial endopeptidases has been proposed to promote complete digestion of cereal proteins and thus destroy T cell multipotent epitopes. The identification of gliadin peptide sequences having biological effects, either through non immune-mediated mechanisms, or by activation of T cells, is important. Breeding programs and/or transgenic technology may lead to production of wheat that is devoid of biologically active peptide sequences. The identification of specific epitopes may also provide a target for immunomodulation of antigenic peptides. Engineered peptides may potentially bind to HLA molecules but not T cell receptors (TCR), or bind TCR but switch a proinflammatory Th1 to a Th2 or protective Th3 response. Other promising areas include inhibition of the innate immune response activated by gliadin peptides, preventing gliadin presentation to T cells by blocking HLA binding sites, use of TG2 inhibitors, and assessing IL-10 as a tool to promote tolerance. An immunomodulatory approach will need to have a safety profile equivalent to that of the gluten-free diet, but with the advantage of increased compliance. REFERENCES 1. Dicke WM, Weijers HA, Van de Kamer JK: The presence in wheat of a factor having a deleterious effect in cases of coeliac disease. Acta Pediatr 1953;42: Shiner M, Doniach I: Histopathologic studies in steatorrhoea. Gastroenterology 23
24 1960;38: Meeuwisse G: Diagnostic criteria in coeliac disease. Acta Pediatr Scand 1970;59: Janatuinen EK, Pikkarainem PH, Kemppainen TA, et al: A comparison of diets with and without oats in adults with celiac disease. N Engl J Med 1995;333: Srinivasan U, Leonard N, Jones E, et al: Absence of oats toxicity in adult coeliac disease. BMJ 1996;313: Lundin KE, Nilsen EM, Scott HG, et al: Oats induced villous atrophy in coeliac disease. Gut 2003; 52: Vader W, Kooy Y, Van Veelen P, et al: The gluten response in children with celiac disease is directed toward multiple gliadin and glutenin peptides. Gastroenterology 2002; 122: Arentz-Hansen H, Mcadam SN, Molberg O, et al: Celiac lesion T cells recognize epitopes that cluser in regions of gliadins rich in proline residues. Gastroenterology 2002; 123: Maiuri L, Ciacci C, Ricciardelli I, et al: Association between innate response to gliadin and activation of pathogenic T cell in coeliac disease. Lancet 2003;362: Gianfrani C, Troncone R, Mugione P, et al: Celiac disease association with CD8+ T cell responses: indentification of a novel gliadin-derived HLA-A2-restricted epitope. J Immunol 2003;170:
25 11. Sturgess R, Day P, Ellis HJ, et al: Wheat peptide challenge in coeliac disease. Lancet 1994;343: Marsh MN, Morgan S, Ensari A, et al: In vivo activity of peptides 31-43,44-55, of A-gliadin in gluten-sensitive enteropathy (GSE). Gastroenterology 1995;108:A Fraser JS, Engel W, Ellisi HJ, et al: Celiac disease: in vivo toxicity of the putative immunodominant epitope. Gut 2003;52: Greco L, Romino R, Coto I, et al: The first large population based twin study of coeliac disease. Gut 2002;50: Ivarsson A, Persson LA, Nystrom L, et al: Epidemic of coeliac disease in Swedish children. Acta Paediat 2000;89: Ivarsson A, Hernell O, Stenlund H et al: Breast-feeding protects against celiac disease. Am J Clin Nutr 2002;75: Auricchio S, Follo D, de Ritis G, et al: Working hypothesis: does breast feeding protect against the development of clinical symptoms of coeliac disease in children? J Pediatr Gastroenterol Nutr 1983;2: Monteleone G, Pender SL, Alstead E, et al: Role of interferon alpha in promoting T helper cell type 1 responses in the small intestine in coeliac disease. Gut 2001;48: Ivarsson A, Hernell O, Nystrom L et al: Children born in the summer have increased risk for coeliac disease. J Epidemiol Community Health. 2003;57: Auricchio S, Mazzacca G, Tosi R, et al: Coeliac disease as a familial condition: 25
26 identification of asymtomatic coeliac patients within family groups. Gastroenterol Int 1988;1: Sollid ML, Markussen G, Ek J, et al: Evidence for a primary association of celiac disease to a particular HLA-DQ alpha/beta heterodimer. J Exp Med 1989;169: Karell K, Louka AS, Moodie SJ, et al: HLA types in celiac disease patients not carrying the DQA1*05-DQB1*02 (DQ2) heterodimer: results from the European Genetics Cluster on celiac disease. Hum Immunol 2003;64: Vader W, Stepniak D, Kooy Y, et al: The HLA-DQ2 gene dose effect in celiac disease is directly related to the magnitude and breadth of gluten-specific T cell responses. Proc Natl Acad Sci USA 2003; 100: Djilali-Saiah I, Schmitz J, Harfouch-Hammoud E, et al: CTLA-4gene polymorphism is associated with predisposition to celiac disease. Gut 1998;43: Babron MC, Nilsson S, Adamovic S, et al: Meta and pooled analysis of European coeliac disease data. Eur J Hum Genet 2003;11: Greco L, Corazza G, Babron MC, et al: Genome search in celiac disease Am J Hum Genet 1998; 62: Van Belzen MJ, Meijer JW, Sandkuijl LA, et al: A major non-hla locus in celiac disease maps to chromosome 19. Gastroenterology 2003;125: Greco L, Maki M, Di Donato F, Visakorpi IK: Epidemiology of coeliac disease in Europe and the Mediterranean area: a summary report on multicentre study by the 26
27 European Society of Paediatric Gastroenterol ogy and Nutrition. In Auricchio S, Visakorpi JK (eds): Common Food Intolerances. Vol 1: Epidemiology of Coeliac Disease. Basel, Karger, 1992, pp Maki M, Mustalahti K, Kokkonen J, et al: Prevalance of celiac disease among children in Finland. N Engl J Med 2003;348: Fasano A, Catassi C: Current approaches to diagnosis and treatment of celiac disease: an evolving spectrum. Gastoenterology 2001; 120: Collin P, Rasmussen M, Kyronpalo S, et al: The hunt for coeliac disease in primary care. QJM 2002;95: Andria G, Cucchiara S, De Vizia B, et al: Brush border and cytosol peptidase activities of human small intestine in normal subjects and celiac disease. Pediatr Res 1980;14: Hausch F, Shan L, Santiago NA, et al: Intestinal digestive resitence of immunodominant gliadin peptides. Am J Physiol Gastrointest Liver Physiol 2002;283:G996-G Shan L, Molberg O, Parrot I, et al: Structural basis for gluten intolerance in celiac sprue. Science 2002; 297: Matysiak-Budnik T, Candalh C, Dugave C, et al: Alterations of the intestinal trasport and processing of gliadin peptides in celiac disease. Gastroenterology 2003;125: Sollid L: Coeliac disease dissecting a complex inflammatory disorder. Nat Rev Immunol 2002;9:
28 37. Salvati VM, MacDonald TT, Bajaj-Elliott M, et al: Interleukin 18 and associated markers of T Helper cell type 1 activity in coeliac disease. Gut 2002;50: Mazzarella G, MacDonald TT, Salvati VM, et al: Constitutive activation of the signal transducer and activator of trascription pathway in celiac disease lesions. Am J Pathol 2003;162: Salvati VM, MacDonald TT, Del Vecchio Blanco G, et al: Enhanced expression of interferon regulatory factor-1 in the mucosa of children with celiac disease. Pediatr Res 2003;54: Forsberg G, Hernell O, Melgar S, et al: Paradoxical coexpression of proinflammatory and Down-regulatory cytokines in intestinal T cells in childhood celiac disease. Gastroenterology 2002;123: Daum S, Bauer U, Foss HD, et al: Increased expression of mrna for matrix metalloproteinases-1 and 3 and tissue inhibitor of metalloproteinases-1 in intestinal biopsy speciems from patients with coeliac disease. Gut 1999;44: Salvati VM, Bajaj-Elliott M, Poulsom R, et al: Keratinocyte growth factor and coeliac disease. Gut 2001;49: Jabri B, De Serre NP, Cellier C, et al :Selective expansion of intraepithelial lymphocytes expressing the HLA-E-specific natural killer receptor CD94 in celiac disease. Gastroenterology 2000; 118: Maiuri L, Ciacci C, Raia V, et al: FAS engagement drives apoptosis of enterocytes of coeliac patients. Gut. 2001;48: Ciccocioppo R, Di Sabatino A, Parroni R, et al: Cytolytic mechanisms of 28
29 intraepithelial lymphocytes in coeliac disease. Clin Exp Immunol 2000;120: Dieterich W, Ehnis T, Bauer M, et al: Identification of tissue transglutaminase as the autoantigen of celiac disease. Mat Med 1997;3: Esposito C, Paparo F, Caputo I, et al: Anti-tissue transglutaminase antibodies from coeliac patients inhibit transglutaminase activity both in vitro and in situ. Antitissue transglutaminase antibodies from coeliac patients inhibit transglutaminase activity both in vitro and in situ. Gut 2002; 51: Halttunen T, Maki M: Serum immunoglobulin A from patients with celiac disease inhibits human T84 intestinal crypt epithelial cell differentation. Gastroenterology 1999;116: Marzari R, Sblattero D, Florian F, et al: Molecular dissection of the tissue transglutaminase autoantibody response in celiac disease. J Immunol 2001;166: Korponay-Szabo IR, Halttunen T, Szalai Z, et al: In vivo targeting of intestinal and extraintestinal transglutaminase 2 coeliac autoantibodies. Gut in press. 51. Sollid LM, Molberg O, McAdam S, Lundin KE. Autoantibodies in coeliac disease: tissue transglutaminase guilt by association? Gut 1997; 41: Clemente MG, Musu MP, Frau F, et al: Immune reaction agiast the cytoskeleton in coeliac disease. Gut 2000; 47: Sanchez D, Tuckova L, Mothes T, et al: Epitopes of calreticulin recognised by IgA autoantibodies from patients with hepatic and celiac disease. J Autoimmun 29
30 2003;21: Stulik J, Hernychova L, Porkertova S, et al: Identification of new celiac disease autoantigens using proteomic analysis. Proteomics 2003; 3: Holm K, Savilahti E, Koskimies S, et al: Immunohistochemical changes in the jejunum in first degree relatives of patients with coeliac disease and the coeliac disease marker DQ genes. HLA class II antigen expression, interleukin-2 receptor positive cells and dividing crypt cells. Gut 1994; 35: Spencer J, Isaacson PG, MacDonald TT, et al: Gamma/delta T cells and the diagnosis of coeliac disease. Clin Exp Immunol 1991; 85: Kaukinen K, Maki M, Partanen J, et al: Celiac disease without atrophy. Dig Dis Sci 2001; 46: Cacciari E, Volta U, Lazzari R et al. Can antigliadin antibody defect symptomless coeliac disease in children with short stature? Lancet 1985; 1 (8444): Bottaro G, Cataldo F, Rotolo N, Spina M and Corazza GR. The clinical pattern of subclinical/silent celiac disease: an analysis on 1026 consecutive cases. Am J Gastroenterol 1999; 94: Corazza GR, Valentini RA, Andreani ML et al. Subclinical coeliac disease is a frequent cause of iron-deficiency anemia. Scand J Gastroenterol 1995; 30: Maki M, Hallstrom O, Verronen P et al. Reticulin antibody, arthritis, and coeliac disease in children. Lancet 1988; 1 (8583): Lindh E, Ljungahall S, Larsson K, Lavo B. Screening for antibodies against gliadin in patients with osteoporosis. J Intern Med 1992;231:
31 63. Molteni N, Caraceni MP, Bardella MT et al. Bone mineral density in adult celiac patients and the effect of gluten-free diet from childhood. Am J Gastroenterol 1990; 85: Gobbi G, Bouquet F, Greco L et al. Coeliac disease, epilepsy, and cerebral calcifications. Lancet 1992; 340: Hadjivassiliou M, Gibson A, Davies-Jones GAB et al. Does cryptic gluten sensitivity play a part in neurological illness? Lancet 1996; 347: Vajro P, Fontanella A, Mayer M et al. Elevated serum aminotransferase activity as a presentation of gluten-sensitive enteropathy. J Pediatr 1993; 122: Volta U, De Franceschi L, Lari F et al. Coeliac disease hidden by cryptogenic hypertransaminasemia. Lancet 1998; 352: Kaukinen K, Halme L, Collin P, et al: Celiac disease in patients with severe liver disease: gluten-free diet may reverse hepatic failture. Gastroenterology 2002;122: Collin P, Vilska S, Heinonen PK, Hallstrom O, Pikkarainen P. Infertility and coeliac disease. Gut 1996; 39: Martinelli P, Troncone R, Paparo F et al. Coeliac disease and unfavourable outcome of pregnancy. Gut 2000; 46: Aine L, Maki M, Collin P, Keyrilainen O. Dental enamel defects in celiac disease. J Oral Pathol 1990; 19: Corazza GR, Andreani ML, Venturo N et al. Celiac disease and alopecia areata: report of a new association. Gastroenterology 1995;
32 73. Reunala T, Kosnai T, Karpati S, et al: Dermatitis herpetiformis: jejunal findings and skin response to gluten-free diet. Arch Dis Child 1984;59: Mulder CJJ, '1:Ytgat GNJ, Groenland F, Pena AS: Combined coeliac disease and thyroid disease: a study of 17 cases. J Clin Nutr Gastroen- teroi1988;3: Reunala T, Salmi J, Karvonen J: Dermatitis herpetiformis and coeliac disease associated with Addison's disease. Arch Dermatol 1987;123: Stene-Larsen G, Mosvold J, Ly B: Selective vitarnin B'2 malabsorption in adult coeliac disease: report on three cases with associated autoim- mune diseases. Scand J Gastroenterol 1988;23: Stenhammar L, Ljunggren CG: Thrombocytopenic purpura and coeliac disease. Acta Paediatr Scand 1988;77: Douglas ID, Gillon J, Logan RFA, et al: Sarcoidosis and coeliac disease: an association. Lancet 1984;2: Savilahti E, Simell O, Koskimes S, et al: Coeliac disease in insulin- dependent diabetes mellitus. J Pediatr 1986;108: Corazza GR, Andreani ML, Venturo N, et al: Coeliac disease and alopecia areata: report of a new association. Gastroenterology 1995;109: Not T, Faleschini E, Tommasini A, et al: Celiac disease in patients with sporadic and inherited cardiomyopathies and in their relatives. Eur Heart J 2003; 24: Ventura A, Magazzu G, Greco L, et al: Autoimmune disorders, coeliac disease: relationship with duration of exposure to gluten. J Pediatr Gastroenterol Nutr 32
33 1997;24: Amil Dias J, Wa1ker-Smith J: Down's syndrome and coeliac disease. J Pediatr Gastroenterol Nutr 1990;10: Bonamico M, Pasquino AM, Mariani P, et al: Prevalence and clinical picture of celiac disease in Turner sindrome. J Clin Endocrinol Metab 2002;87: Giannotti A, Tiberio G, Castro M, et al : Coeliac disease in Williams sindrome. J Med Genet 2001;38: Savilahti E, Pelkonen P, Visakorpi JK: IgA deficiency in children: a clinical study with special reference to intestinal findings. Arch Dis Child 1971;46: Juby LD, Rothwell J, Axon ATR: Lactuloselmannitol test: an ideal screen for coeliac disease. Gastroenterology 1989;96: Juby LD, Rothwell J, Axon ATR: Cellobioselmannitol sugar test-a sensitive tubeless test for coeliac disease: results on 1010 unselected patients. Gut 1989;30: Sulkanen S, Halttunen T, Laurila K, et al. Tissue transglutaminase autoantibody enzyme-linked immunosorbent assay in detecting celiac disease. Gastroenterology 1998; 115: Collin P, Helin H, Maki M, Hallstrom O, Karvonen AL. Follow-up of patients positive in reticulin and gliadin antibody tests with normal small bowel biopsy findings. Scand J Gastroenterol 1993; 28: Rostami K, Kerckhaert J, Tiemessen R, von Blomberg ME, Mejer JWR, Mulder CJJ. Sensitivity of anti-endomysium and anti-gliadin antibodies in untreated 33
Diseases of the gastrointestinal system Dr H Awad Lecture 5: diseases of the small intestine
 Diseases of the gastrointestinal system 2018 Dr H Awad Lecture 5: diseases of the small intestine Small intestinal villi Small intestinal villi -Villi are tall, finger like mucosal projections, found
Diseases of the gastrointestinal system 2018 Dr H Awad Lecture 5: diseases of the small intestine Small intestinal villi Small intestinal villi -Villi are tall, finger like mucosal projections, found
November Laboratory Testing for Celiac Disease. Inflammation in Celiac Disease
 November 2011 Gary Copland, MD Chair, Department of Pathology, Unity Hospital Laboratory Medical Director, AMC Crossroads Chaska and AMC Crossroads Dean Lakes Laboratory Testing for Celiac Disease Celiac
November 2011 Gary Copland, MD Chair, Department of Pathology, Unity Hospital Laboratory Medical Director, AMC Crossroads Chaska and AMC Crossroads Dean Lakes Laboratory Testing for Celiac Disease Celiac
Primary Care Update January 26 & 27, 2017 Celiac Disease: Concepts & Conundrums
 Primary Care Update January 26 & 27, 2017 Celiac Disease: Concepts & Conundrums Alia Hasham, MD Assistant Professor Division of Gastroenterology, Hepatology & Nutrition What is the Preferred Initial Test
Primary Care Update January 26 & 27, 2017 Celiac Disease: Concepts & Conundrums Alia Hasham, MD Assistant Professor Division of Gastroenterology, Hepatology & Nutrition What is the Preferred Initial Test
Diagnosis Diagnostic principles Confirm diagnosis before treating
 Diagnosis 1 1 Diagnosis Diagnostic principles Confirm diagnosis before treating Diagnosis of Celiac Disease mandates a strict gluten-free diet for life following the diet is not easy QOL implications Failure
Diagnosis 1 1 Diagnosis Diagnostic principles Confirm diagnosis before treating Diagnosis of Celiac Disease mandates a strict gluten-free diet for life following the diet is not easy QOL implications Failure
CELIAC DISEASE - GENERAL AND LABORATORY ASPECTS Prof. Xavier Bossuyt, Ph.D. Laboratory Medicine, Immunology, University Hospital Leuven, Belgium
 CELIAC DISEASE - GENERAL AND LABORATORY ASPECTS Prof. Xavier Bossuyt, Ph.D. Laboratory Medicine, Immunology, University Hospital Leuven, Belgium 5.1 Introduction Celiac disease is a chronic immune-mediated
CELIAC DISEASE - GENERAL AND LABORATORY ASPECTS Prof. Xavier Bossuyt, Ph.D. Laboratory Medicine, Immunology, University Hospital Leuven, Belgium 5.1 Introduction Celiac disease is a chronic immune-mediated
Gluten Sensitivity Fact from Myth. Disclosures OBJECTIVES 18/09/2013. Justine Turner MD PhD University of Alberta. None Relevant
 Gluten Sensitivity Fact from Myth Justine Turner MD PhD University of Alberta Disclosures None Relevant OBJECTIVES Understand the spectrum of gluten disorders Develop a diagnostic algorithm for gluten
Gluten Sensitivity Fact from Myth Justine Turner MD PhD University of Alberta Disclosures None Relevant OBJECTIVES Understand the spectrum of gluten disorders Develop a diagnostic algorithm for gluten
Epidemiology. The old Celiac Disease Epidemiology:
 Epidemiology 1 1 Epidemiology The old Celiac Disease Epidemiology: A rare disorder typical of infancy Wide incidence fluctuates in space (1/400 Ireland to 1/10000 Denmark) and in time A disease of essentially
Epidemiology 1 1 Epidemiology The old Celiac Disease Epidemiology: A rare disorder typical of infancy Wide incidence fluctuates in space (1/400 Ireland to 1/10000 Denmark) and in time A disease of essentially
Meredythe A. McNally, M.D. Gastroenterology Associates of Cleveland Beachwood, OH
 Meredythe A. McNally, M.D. Gastroenterology Associates of Cleveland Beachwood, OH Case in point 42 year old woman with bloating, gas, intermittent diarrhea alternating with constipation, told she has IBS
Meredythe A. McNally, M.D. Gastroenterology Associates of Cleveland Beachwood, OH Case in point 42 year old woman with bloating, gas, intermittent diarrhea alternating with constipation, told she has IBS
Celiac Disease: The Quintessential Autoimmune Disease Ivor D. Hill, MB, ChB, MD.
 Celiac Disease: The Quintessential Autoimmune Disease Ivor D. Hill, MB, ChB, MD..... Celiac Disease Autoimmune Diseases What are they? How do you get them? Why does it matter? Celiac Disease Autoimmune
Celiac Disease: The Quintessential Autoimmune Disease Ivor D. Hill, MB, ChB, MD..... Celiac Disease Autoimmune Diseases What are they? How do you get them? Why does it matter? Celiac Disease Autoimmune
Diagnostic Testing Algorithms for Celiac Disease
 Diagnostic Testing Algorithms for Celiac Disease HOT TOPIC / 2018 Presenter: Melissa R. Snyder, Ph.D. Co-Director, Antibody Immunology Laboratory Department of Laboratory Medicine and Pathology, Mayo Clinic
Diagnostic Testing Algorithms for Celiac Disease HOT TOPIC / 2018 Presenter: Melissa R. Snyder, Ph.D. Co-Director, Antibody Immunology Laboratory Department of Laboratory Medicine and Pathology, Mayo Clinic
Peter HR Green MD. Columbia University New York, NY
 CELIAC DISEASE, 2008 Peter HR Green MD Celiac Disease Center Columbia University New York, NY pg11@columbia.edu DIAGNOSIS OF CELIAC DISEASE Presence of consistent pathology and response to a gluten-free
CELIAC DISEASE, 2008 Peter HR Green MD Celiac Disease Center Columbia University New York, NY pg11@columbia.edu DIAGNOSIS OF CELIAC DISEASE Presence of consistent pathology and response to a gluten-free
Celiac Disease. Detlef Schuppan HARVARD MEDICAL SCHOOL
 Celiac Disease Detlef Schuppan Falk Symposium in the Intestinal Tract: Pathogenesis and Treatment, Kiev,, Ukraine, May 15-16, 16, 2009 HARVARD MEDICAL SCHOOL Celiac Disease Intolerance to gluten from wheat,
Celiac Disease Detlef Schuppan Falk Symposium in the Intestinal Tract: Pathogenesis and Treatment, Kiev,, Ukraine, May 15-16, 16, 2009 HARVARD MEDICAL SCHOOL Celiac Disease Intolerance to gluten from wheat,
See Policy CPT CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: LAB Policy No: 404 Medical Policy Committee Approved Date: 12/17; 12/18 1/1/19 Medical Officer Date APPLIES TO: All lines of business See Policy CPT CODE section below
Effective Date: 1/1/2019 Section: LAB Policy No: 404 Medical Policy Committee Approved Date: 12/17; 12/18 1/1/19 Medical Officer Date APPLIES TO: All lines of business See Policy CPT CODE section below
Celiac Disease Ce. Celiac Disease. Barry Z. Hirsch, M.D. Baystate Pediatric Gastroenterology and Nutrition. baystatehealth.org/bch
 Celiac Disease Ce Celiac Disease Barry Z. Hirsch, M.D. Baystate Pediatric Gastroenterology and Nutrition baystatehealth.org/bch Autoimmune Disease Inappropriate inflammation 1 1/21/15 Celiac Disease Classic
Celiac Disease Ce Celiac Disease Barry Z. Hirsch, M.D. Baystate Pediatric Gastroenterology and Nutrition baystatehealth.org/bch Autoimmune Disease Inappropriate inflammation 1 1/21/15 Celiac Disease Classic
Disclosures GLUTEN RELATED DISORDERS CELIAC DISEASE UPDATE OR GLUTEN RELATED DISORDERS 6/9/2015
 Disclosures CELIAC DISEASE UPDATE OR GLUTEN RELATED DISORDERS 2015 Scientific Advisory Board: Alvine Pharmaceuticals, Alba Therapeutics, ImmunsanT Peter HR Green MD Columbia University New York, NY GLUTEN
Disclosures CELIAC DISEASE UPDATE OR GLUTEN RELATED DISORDERS 2015 Scientific Advisory Board: Alvine Pharmaceuticals, Alba Therapeutics, ImmunsanT Peter HR Green MD Columbia University New York, NY GLUTEN
Spectrum of Gluten Disorders
 Food Intolerance:Celiac Disease and Gluten Sensitivity-A Guide for Healthy Lifestyles Ellen Karlin 2018 Spectrum of Gluten Disorders Wheat allergy - prevalence 3-8 % (up to 3 years old) Non-celiac gluten
Food Intolerance:Celiac Disease and Gluten Sensitivity-A Guide for Healthy Lifestyles Ellen Karlin 2018 Spectrum of Gluten Disorders Wheat allergy - prevalence 3-8 % (up to 3 years old) Non-celiac gluten
Is It Celiac Disease or Gluten Sensitivity?
 Is It Celiac Disease or Gluten Sensitivity? Mark T. DeMeo MD, FACG Rush University Med Center Case Study 35 y/o female Complains of diarrhea, bloating, arthralgias, and foggy mentation Cousin with celiac
Is It Celiac Disease or Gluten Sensitivity? Mark T. DeMeo MD, FACG Rush University Med Center Case Study 35 y/o female Complains of diarrhea, bloating, arthralgias, and foggy mentation Cousin with celiac
New Insights on Gluten Sensitivity
 New Insights on Gluten Sensitivity Sheila E. Crowe, MD, FRCPC, FACP, FACG, AGAF Department of Medicine University of California, San Diego Page 1 1 low fat diet low carb diet gluten free diet low fat diet
New Insights on Gluten Sensitivity Sheila E. Crowe, MD, FRCPC, FACP, FACG, AGAF Department of Medicine University of California, San Diego Page 1 1 low fat diet low carb diet gluten free diet low fat diet
Am I a Silly Yak? Laura Zakowski, MD. No financial disclosures
 Am I a Silly Yak? Laura Zakowski, MD No financial disclosures Patient NP 21 year old male with chronic headaches for 6 years extensively evaluated and treated Acupuncturist suggests testing for celiac
Am I a Silly Yak? Laura Zakowski, MD No financial disclosures Patient NP 21 year old male with chronic headaches for 6 years extensively evaluated and treated Acupuncturist suggests testing for celiac
Celiac Disease. Etiology. Food Intolerance:Celiac Disease and Gluten Sensitivity-A Guide for Healthy Lifestyles
 Food Intolerance:Celiac Disease and Gluten Sensitivity-A Guide for Healthy Lifestyles Ellen Karlin 2017 Celiac Disease World s most common genetic food disorder Rising prevalence - over past 5 decades,
Food Intolerance:Celiac Disease and Gluten Sensitivity-A Guide for Healthy Lifestyles Ellen Karlin 2017 Celiac Disease World s most common genetic food disorder Rising prevalence - over past 5 decades,
Celiac Disease 1/13/2016. Objectives. Question 1. Understand the plethora of conditions or symptoms that require testing for Celiac Disease (CD)
 Celiac Disease MONTE E. TROUTMAN, DO, FACOI JANUARY 6, 2016 Objectives Understand the plethora of conditions or symptoms that require testing for Celiac Disease (CD) Develop a knowledge of testing needed
Celiac Disease MONTE E. TROUTMAN, DO, FACOI JANUARY 6, 2016 Objectives Understand the plethora of conditions or symptoms that require testing for Celiac Disease (CD) Develop a knowledge of testing needed
Evidence Based Guideline
 Evidence Based Guideline Serologic Diagnosis of Celiac Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: serologic_diagnosis_of_celiac_disease 4/2012 Description of Procedure
Evidence Based Guideline Serologic Diagnosis of Celiac Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: serologic_diagnosis_of_celiac_disease 4/2012 Description of Procedure
BIOPSY AVOIDANCE IN CHILDREN: THE EVIDENCE
 BIOPSY AVOIDANCE IN CHILDREN: THE EVIDENCE Steffen Husby Hans Christian Andersen Children s Hospital Odense University Hospital DK-5000 Odense C, Denmark Agenda Background Algorithm Symptoms HLA Antibodies
BIOPSY AVOIDANCE IN CHILDREN: THE EVIDENCE Steffen Husby Hans Christian Andersen Children s Hospital Odense University Hospital DK-5000 Odense C, Denmark Agenda Background Algorithm Symptoms HLA Antibodies
Celiac Disease. Sheryl Pfeil, MD The Ohio State University Division of Gastroenterology, Hepatology, and Nutrition. January 2015
 Celiac Disease Sheryl Pfeil, MD The Ohio State University Division of Gastroenterology, Hepatology, and Nutrition January 2015 Objectives Review the clinical presentation of celiac disease, including intestinal
Celiac Disease Sheryl Pfeil, MD The Ohio State University Division of Gastroenterology, Hepatology, and Nutrition January 2015 Objectives Review the clinical presentation of celiac disease, including intestinal
Activation of Innate and not Adaptive Immune system in Gluten Sensitivity
 Activation of Innate and not Adaptive Immune system in Gluten Sensitivity Update: Differential mucosal IL-17 expression in gluten sensitivity and the autoimmune enteropathy celiac disease A. Sapone, L.
Activation of Innate and not Adaptive Immune system in Gluten Sensitivity Update: Differential mucosal IL-17 expression in gluten sensitivity and the autoimmune enteropathy celiac disease A. Sapone, L.
Esperanza Garcia-Alvarez MD Medical Director Pediatric Celiac Center at Advocate Children s Hospital
 Esperanza Garcia-Alvarez MD Medical Director Pediatric Celiac Center at Advocate Children s Hospital Nothing to disclose Objectives Better understanding pathogenesis celiac disease Better understanding
Esperanza Garcia-Alvarez MD Medical Director Pediatric Celiac Center at Advocate Children s Hospital Nothing to disclose Objectives Better understanding pathogenesis celiac disease Better understanding
Challenges in Celiac Disease. Adam Stein, MD Director of Nutrition Support Northwestern University Feinberg School of Medicine
 Challenges in Celiac Disease Adam Stein, MD Director of Nutrition Support Northwestern University Feinberg School of Medicine Disclosures None Overview Celiac disease Cases Celiac disease Inappropriate
Challenges in Celiac Disease Adam Stein, MD Director of Nutrition Support Northwestern University Feinberg School of Medicine Disclosures None Overview Celiac disease Cases Celiac disease Inappropriate
Therapeutical implication of regulatory cells and cytokines in celiac disease
 Institute of Food Sciences, CNR Avellino, Italy Therapeutical implication of regulatory cells and cytokines in celiac disease Carmen Gianfrani Mastering the coeliac condition: from medicine to social sciences
Institute of Food Sciences, CNR Avellino, Italy Therapeutical implication of regulatory cells and cytokines in celiac disease Carmen Gianfrani Mastering the coeliac condition: from medicine to social sciences
Celiac Disease. Gluten-Sensitive Enteropathy Celiac Sprue Non-tropical Sprue
 Celiac Disease Gluten-Sensitive Enteropathy Celiac Sprue Non-tropical Sprue Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
Celiac Disease Gluten-Sensitive Enteropathy Celiac Sprue Non-tropical Sprue Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
Presentation and Evaluation of Celiac Disease
 Presentation and Evaluation of Celiac Disease C. CUFFARI, MD, FRCPC, FACG, AGAF The Johns Hopkins Hospital Baltimore MD. Main Points Celiac disease is not rare (1 in 100-300) It can present in many ways:
Presentation and Evaluation of Celiac Disease C. CUFFARI, MD, FRCPC, FACG, AGAF The Johns Hopkins Hospital Baltimore MD. Main Points Celiac disease is not rare (1 in 100-300) It can present in many ways:
Slides and Resources.
 Update on Celiac Disease Douglas L. Seidner, MD, AGAF, FACG Director, Center for Human Nutrition Vanderbilt University As revised/retold by Edward Saltzman, MD Tufts University None Disclosures This ppt
Update on Celiac Disease Douglas L. Seidner, MD, AGAF, FACG Director, Center for Human Nutrition Vanderbilt University As revised/retold by Edward Saltzman, MD Tufts University None Disclosures This ppt
CONTEMPORARY CONCEPT ON BASIC APSECTS OF GLUTEN-SENSITIVE ENTEROPATHY IN ELDERLY PATIENTS
 VIII, 2014, 1 33. 1,. 2,. - 1,. 1. 3 1,., 2,., 3, CONTEMPORARY CONCEPT ON BASIC APSECTS OF GLUTEN-SENSITIVE ENTEROPATHY IN ELDERLY PATIENTS Ts. Velikova 1, Z. Spassova 2,. Ivanova-Todorova 1, D. Kyurkchiev
VIII, 2014, 1 33. 1,. 2,. - 1,. 1. 3 1,., 2,., 3, CONTEMPORARY CONCEPT ON BASIC APSECTS OF GLUTEN-SENSITIVE ENTEROPATHY IN ELDERLY PATIENTS Ts. Velikova 1, Z. Spassova 2,. Ivanova-Todorova 1, D. Kyurkchiev
Sheila E. Crowe, MD, FACG
 1A: Upper Gut Celiac Disease: When to Look and How? Sheila E. Crowe, MD, FACG Learning Objectives At the end of this presentation, the successful learner should be able to: Identify the many groups of
1A: Upper Gut Celiac Disease: When to Look and How? Sheila E. Crowe, MD, FACG Learning Objectives At the end of this presentation, the successful learner should be able to: Identify the many groups of
Coeliac disease. Do I have coeliac. disease? Diagnosis, monitoring & susceptibilty. Laboratory flowsheet included
 Laboratory flowsheet included I have coeliac disease. What monitoring tests should be performed? Do I have coeliac disease? Are either of our children susceptible to coeliac disease? Monitoring tests Diagnostic
Laboratory flowsheet included I have coeliac disease. What monitoring tests should be performed? Do I have coeliac disease? Are either of our children susceptible to coeliac disease? Monitoring tests Diagnostic
Baboons Affected by Hereditary Chronic Diarrhea as a Possible Non-Human Primate Model of Celiac Disease
 Baboons Affected by Hereditary Chronic Diarrhea as a Possible Non-Human Primate Model of Celiac Disease Debby Kryszak 1, Henry McGill 2, Michelle Leland 2,, Alessio Fasano 1 1. Center for Celiac Research,
Baboons Affected by Hereditary Chronic Diarrhea as a Possible Non-Human Primate Model of Celiac Disease Debby Kryszak 1, Henry McGill 2, Michelle Leland 2,, Alessio Fasano 1 1. Center for Celiac Research,
Gluten-Free China Gastro Q&A
 Gluten-Free China Gastro Q&A Akiko Natalie Tomonari MD akiko.tomonari@parkway.cn Gastroenterology Specialist ParkwayHealth Introduction (of myself) Born in Japan, Raised in Maryland, USA Graduated from
Gluten-Free China Gastro Q&A Akiko Natalie Tomonari MD akiko.tomonari@parkway.cn Gastroenterology Specialist ParkwayHealth Introduction (of myself) Born in Japan, Raised in Maryland, USA Graduated from
CELIAC SPRUE. What Happens With Celiac Disease
 CELIAC SPRUE Celiac Disease (CD) is a lifelong, digestive disorder affecting children and adults. When people with CD eat foods that contain gluten, it creates an immune-mediated toxic reaction that causes
CELIAC SPRUE Celiac Disease (CD) is a lifelong, digestive disorder affecting children and adults. When people with CD eat foods that contain gluten, it creates an immune-mediated toxic reaction that causes
Understanding Celiac Disease
 Understanding Diagnostic Challenges Sheryl Pfeil, MD Professor of Clinical Medicine Division of Gastroenterology, Hepatology and Nutrition Department of Internal Medicine The Ohio State University Wexner
Understanding Diagnostic Challenges Sheryl Pfeil, MD Professor of Clinical Medicine Division of Gastroenterology, Hepatology and Nutrition Department of Internal Medicine The Ohio State University Wexner
Understanding Celiac Disease
 Understanding Celiac Disease Diagnostic Challenges Sheryl Pfeil, MD Professor of Clinical Medicine Division of Gastroenterology, Hepatology and Nutrition Department of Internal Medicine The Ohio State
Understanding Celiac Disease Diagnostic Challenges Sheryl Pfeil, MD Professor of Clinical Medicine Division of Gastroenterology, Hepatology and Nutrition Department of Internal Medicine The Ohio State
CELIAC DISEASE. Molly Jennings Deb McCafferty MS, RD
 CELIAC DISEASE Molly Jennings Deb McCafferty MS, RD WHAT IS CELIAC DISEASE? In short In this disease, exposure to gluten results in damge to the intestinal mucosa. Immune-mediated disorder Also known as
CELIAC DISEASE Molly Jennings Deb McCafferty MS, RD WHAT IS CELIAC DISEASE? In short In this disease, exposure to gluten results in damge to the intestinal mucosa. Immune-mediated disorder Also known as
HLA types in Turkish children with celiac disease
 The Turkish Journal of Pediatrics 2008; 50: 515-520 Original HLA types in Turkish children with celiac disease Zarife Kuloğlu 1, Tümay Doğancı 2, Aydan Kansu 1, Fulya Demirçeken 1, Murat Duman 3, Hüseyin
The Turkish Journal of Pediatrics 2008; 50: 515-520 Original HLA types in Turkish children with celiac disease Zarife Kuloğlu 1, Tümay Doğancı 2, Aydan Kansu 1, Fulya Demirçeken 1, Murat Duman 3, Hüseyin
Celiac Disease: The Past and The Present
 Celiac Disease: The Past and The Present The Center for Celiac Research and Mucosal Biology Research Center University of Maryland School of Medicine Baltimore, Maryland, U.S.A. 1 Celiac Disease Roadmap:
Celiac Disease: The Past and The Present The Center for Celiac Research and Mucosal Biology Research Center University of Maryland School of Medicine Baltimore, Maryland, U.S.A. 1 Celiac Disease Roadmap:
Alliance for Best Practice in Health Education
 Alliance for Best Practice in Health Education Objectives Following this program, participants will 1. List the clinical situations where celiac disease should be suspected 2. Distinguish between celiac
Alliance for Best Practice in Health Education Objectives Following this program, participants will 1. List the clinical situations where celiac disease should be suspected 2. Distinguish between celiac
EAT ACCORDING TO YOUR GENES. NGx-Gluten TM. Personalized Nutrition Report
 EAT ACCORDING TO YOUR GENES NGx-Gluten TM Personalized Nutrition Report Introduction Hello Caroline: Nutrigenomix is pleased to provide you with your NGx-Gluten TM Personalized Nutrition Report based on
EAT ACCORDING TO YOUR GENES NGx-Gluten TM Personalized Nutrition Report Introduction Hello Caroline: Nutrigenomix is pleased to provide you with your NGx-Gluten TM Personalized Nutrition Report based on
Celiac Disease: The Future. Alessio Fasano, M.D. Mucosal Biology Research Center University of Maryland School of Medicine
 Celiac Disease: The Future Alessio Fasano, M.D. Mucosal Biology Research Center University of Maryland School of Medicine Normal small bowel Celiac disease Gluten Gluten-free diet Treatment Only treatment
Celiac Disease: The Future Alessio Fasano, M.D. Mucosal Biology Research Center University of Maryland School of Medicine Normal small bowel Celiac disease Gluten Gluten-free diet Treatment Only treatment
Genetics and Epidemiology of Celiac Disease
 1 Genetics and Epidemiology of Celiac Disease Alessio Fasano, M.D. Mucosal Bilology Research Center and Center for Celiac Research University of Maryland, School of Medicine Address correspondence to:
1 Genetics and Epidemiology of Celiac Disease Alessio Fasano, M.D. Mucosal Bilology Research Center and Center for Celiac Research University of Maryland, School of Medicine Address correspondence to:
Celiac disease is a unique disorder that is both a food
 GASTROENTEROLOGY 2006;131:1981 2002 American Gastroenterological Association () Institute Technical Review on the Diagnosis and Management of Celiac Disease This technical review addresses the state of
GASTROENTEROLOGY 2006;131:1981 2002 American Gastroenterological Association () Institute Technical Review on the Diagnosis and Management of Celiac Disease This technical review addresses the state of
DEAMIDATED GLIADIN PEPTIDES IN COELIAC DISEASE DIAGNOSTICS
 DEAMIDATED GLIADIN PEPTIDES IN COELIAC DISEASE DIAGNOSTICS Z. Vanickova 1, P. Kocna 1, K. Topinkova 1, M. Dvorak 2 1 Institute of Clinical Biochemistry & Laboratory Diagnostics; 2 4th Medical Department,
DEAMIDATED GLIADIN PEPTIDES IN COELIAC DISEASE DIAGNOSTICS Z. Vanickova 1, P. Kocna 1, K. Topinkova 1, M. Dvorak 2 1 Institute of Clinical Biochemistry & Laboratory Diagnostics; 2 4th Medical Department,
What is celiac disease?
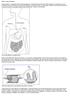 What is celiac disease? Celiac disease is a digestive disease that damages the small intestine and interferes with absorption of nutrients from food. People who have celiac disease cannot tolerate gluten,
What is celiac disease? Celiac disease is a digestive disease that damages the small intestine and interferes with absorption of nutrients from food. People who have celiac disease cannot tolerate gluten,
Celiac Disease and Non Celiac Gluten Sensitivity. John R Cangemi, MD Mayo Clinic Florida
 Celiac Disease and Non Celiac Gluten Sensitivity John R Cangemi, MD Mayo Clinic Florida DISCLOSURE Commercial Interest None Off Label Usage None Learning Objectives Review the clinical presentation of
Celiac Disease and Non Celiac Gluten Sensitivity John R Cangemi, MD Mayo Clinic Florida DISCLOSURE Commercial Interest None Off Label Usage None Learning Objectives Review the clinical presentation of
Diet Isn t Working, We Need to Do Something Else
 Diet Isn t Working, We Need to Do Something Else Ciarán P Kelly, MD Celiac Center Beth Israel Deaconess Medical Center & Celiac Program Harvard Medical School Boston Gluten Free Diet (GFD) Very good but
Diet Isn t Working, We Need to Do Something Else Ciarán P Kelly, MD Celiac Center Beth Israel Deaconess Medical Center & Celiac Program Harvard Medical School Boston Gluten Free Diet (GFD) Very good but
No relevant financial relationships to disclose
 CELIAC DISEASE Michael H. Piper, MD, FACP, FACG Gastroenterology Program Director Chief of Gastroenterology Providence-Providence Park Hospitals/St. John Macomb Hospital No relevant financial relationships
CELIAC DISEASE Michael H. Piper, MD, FACP, FACG Gastroenterology Program Director Chief of Gastroenterology Providence-Providence Park Hospitals/St. John Macomb Hospital No relevant financial relationships
Biomedical Sciences. 26 February Celiac Disease and Malabsorption. Prof. Dr. Christoph Mueller
 Biomedical Sciences 26 February 2014 Celiac Disease and Malabsorption Prof. Dr. Christoph Mueller Institute of Pathology christoph.mueller@pathology.unibe.ch Malabsorption Definition Malabsorption represents
Biomedical Sciences 26 February 2014 Celiac Disease and Malabsorption Prof. Dr. Christoph Mueller Institute of Pathology christoph.mueller@pathology.unibe.ch Malabsorption Definition Malabsorption represents
Celiac & Gluten Sensitivity; serum
 TEST NAME: Celiac & Gluten Sensitivity (Serum) Celiac & Gluten Sensitivity; serum ANTIBODIES REFERENCE RESULT/UNIT INTERVAL NEG WEAK POS POSITIVE Tissue Transglutaminase (ttg) IgA 1420 U < 20.0 Tissue
TEST NAME: Celiac & Gluten Sensitivity (Serum) Celiac & Gluten Sensitivity; serum ANTIBODIES REFERENCE RESULT/UNIT INTERVAL NEG WEAK POS POSITIVE Tissue Transglutaminase (ttg) IgA 1420 U < 20.0 Tissue
Larazotide Acetate. Alessio Fasano, M.D. Mucosal Biology Research Center and Center for Celiac Research University of Maryland School of Medicine
 Larazotide Acetate Alessio Fasano, M.D. Mucosal Biology Research Center and Center for Celiac Research University of Maryland School of Medicine Alternative/Integrative Approaches To The Gluten Free Diet
Larazotide Acetate Alessio Fasano, M.D. Mucosal Biology Research Center and Center for Celiac Research University of Maryland School of Medicine Alternative/Integrative Approaches To The Gluten Free Diet
Coeliac disease: pathogenesis. Riccardo Troncone
 Coeliac disease: pathogenesis Riccardo Troncone Department of Pediatrics & European Laboratory for the Investigation of Food-Induced Diseases University Federico II, Naples, Italy Definition of Celiac
Coeliac disease: pathogenesis Riccardo Troncone Department of Pediatrics & European Laboratory for the Investigation of Food-Induced Diseases University Federico II, Naples, Italy Definition of Celiac
ImuPro shows you the way to the right food for you. And your path for better health.
 Your personal ImuPro Screen + documents Sample ID: 33333 Dear, With this letter, you will receive the ImuPro result for your personal IgG food allergy test. This laboratory report contains your results
Your personal ImuPro Screen + documents Sample ID: 33333 Dear, With this letter, you will receive the ImuPro result for your personal IgG food allergy test. This laboratory report contains your results
Celiac disease Crohn s disease Ulcerative colitis Pseudomembranous colitis
 2017 / 2018 2nd semester/3rd practice Celiac disease Crohn s disease Ulcerative colitis Pseudomembranous colitis Semmelweis University 2nd Department of Pathology CELIAC DISEASE = Gluten-sensitive enteropathy
2017 / 2018 2nd semester/3rd practice Celiac disease Crohn s disease Ulcerative colitis Pseudomembranous colitis Semmelweis University 2nd Department of Pathology CELIAC DISEASE = Gluten-sensitive enteropathy
Current Management of Celiac Disease and Identifying an Appropriate Patient Population(s) for Pharmacologic Therapies in Adult Patients
 Current Management of Celiac Disease and Identifying an Appropriate Patient Population(s) for Pharmacologic Therapies in Adult Patients Joe Murray The Mayo Clinic 1 DISCLOSURES Relevant Financial Relationship(s)
Current Management of Celiac Disease and Identifying an Appropriate Patient Population(s) for Pharmacologic Therapies in Adult Patients Joe Murray The Mayo Clinic 1 DISCLOSURES Relevant Financial Relationship(s)
Gluten Free and Still Symptomatic
 How many celiac patients are affected? Gluten Free and Still Symptomatic 6.2% of all celiac patients have continuing diarrhea after 2 years on a gluten free diet 18% will develop constipation in this time
How many celiac patients are affected? Gluten Free and Still Symptomatic 6.2% of all celiac patients have continuing diarrhea after 2 years on a gluten free diet 18% will develop constipation in this time
Celiac Disease The Great Masquerader Anca M. Safta MD
 Celiac Disease The Great Masquerader Anca M. Safta MD Disclosures Dr. Anca Safta - none Angie Almond, M.Ed., RD, LDN invited attendee of The Gluten Free Summit sponsored by General Mills Wake Forest Baptist
Celiac Disease The Great Masquerader Anca M. Safta MD Disclosures Dr. Anca Safta - none Angie Almond, M.Ed., RD, LDN invited attendee of The Gluten Free Summit sponsored by General Mills Wake Forest Baptist
Name of Policy: Human Leukocyte Antigen (HLA) Testing for Celiac Disease
 Name of Policy: Human Leukocyte Antigen (HLA) Testing for Celiac Disease Policy #: 545 Latest Review Date: June 2015 Category: Laboratory Policy Grade: B Background/Definitions: As a general rule, benefits
Name of Policy: Human Leukocyte Antigen (HLA) Testing for Celiac Disease Policy #: 545 Latest Review Date: June 2015 Category: Laboratory Policy Grade: B Background/Definitions: As a general rule, benefits
Food Intolerance & Expertise SARAH KEOGH CONSULTANT DIETITIAN EATWELL FOOD & NUTRITION
 Food Intolerance & Expertise SARAH KEOGH CONSULTANT DIETITIAN EATWELL FOOD & NUTRITION Food Intolerance & Expertise What is food intolerance? Common food intolerances Why are consumers claiming more food
Food Intolerance & Expertise SARAH KEOGH CONSULTANT DIETITIAN EATWELL FOOD & NUTRITION Food Intolerance & Expertise What is food intolerance? Common food intolerances Why are consumers claiming more food
Coeliac Disease BE AWARE OF HOW YOU PREPARE
 Coeliac Disease BE AWARE OF HOW YOU PREPARE What is it? Auto-immune disorder affecting the small intestine. Triggered by gluten (protein found in wheat, rye, barley, and oats) Strong genetic link: 1 st
Coeliac Disease BE AWARE OF HOW YOU PREPARE What is it? Auto-immune disorder affecting the small intestine. Triggered by gluten (protein found in wheat, rye, barley, and oats) Strong genetic link: 1 st
Institute of Medical Technology, University of Tampere and Department of Pediatrics, Tampere University Hospital, Tampere, Finland
 Gastrointestinal Functions, edited by Edgard E. Delvin and Michael J. Lentze. Nestle Nutrition Workshop Series. Pediatric Program, Vol. 46. Nestec Ltd.. Vevey/Lippincott Williams & Wilkins. Philadelphia
Gastrointestinal Functions, edited by Edgard E. Delvin and Michael J. Lentze. Nestle Nutrition Workshop Series. Pediatric Program, Vol. 46. Nestec Ltd.. Vevey/Lippincott Williams & Wilkins. Philadelphia
Immune mediated enteropathies. Aurora Tatu Bern 26/07/2017
 Immune mediated enteropathies Aurora Tatu Bern 26/07/2017 Definition/classification Systemic disease, mediated by antibodies, caracterised by histological changes of the small bowel Coeliac and noncoeliac
Immune mediated enteropathies Aurora Tatu Bern 26/07/2017 Definition/classification Systemic disease, mediated by antibodies, caracterised by histological changes of the small bowel Coeliac and noncoeliac
GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE
 GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE These are the lactose intolerance guidelines and it is recommended that they are used in conjunction with the Cow s Milk Allergy guidance.
GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE These are the lactose intolerance guidelines and it is recommended that they are used in conjunction with the Cow s Milk Allergy guidance.
Saeeda Almarzooqi, 1 Ronald H. Houston, 2 and Vinay Prasad Introduction
 Pathology Research International Volume 2013, Article ID 602985, 5 pages http://dx.doi.org/10.1155/2013/602985 Clinical Study Utility of Tissue Transglutaminase Immunohistochemistry in Pediatric Duodenal
Pathology Research International Volume 2013, Article ID 602985, 5 pages http://dx.doi.org/10.1155/2013/602985 Clinical Study Utility of Tissue Transglutaminase Immunohistochemistry in Pediatric Duodenal
Celiac Disease. Samuel Gee (1888) first described Celiac disease in On the Coeliac Affection Gluten sensitive entropathy Non-tropical sprue
 Celiac disease Mohammad Rostami Nejad, PhD Head of Celiac disease department Gastroenterology and Liver Diseases Research Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran Celiac Disease
Celiac disease Mohammad Rostami Nejad, PhD Head of Celiac disease department Gastroenterology and Liver Diseases Research Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran Celiac Disease
Kamran Rostami, MD, PhD Gastroenterology Unit, Milton Keynes, University Hospital UK
 Kamran Rostami, MD, PhD Gastroenterology Unit, Milton Keynes, University Hospital UK Outline Gluten related disorders -Classification Pathogenesis Histology of coeliac disease What is a normal intestinal
Kamran Rostami, MD, PhD Gastroenterology Unit, Milton Keynes, University Hospital UK Outline Gluten related disorders -Classification Pathogenesis Histology of coeliac disease What is a normal intestinal
OHTAC Recommendation
 OHTAC Recommendation Clinical Utility of Serologic Testing for Celiac Disease in Ontario Presented to the Ontario Health Technology Advisory Committee in April and October, 2010 December 2010 Background
OHTAC Recommendation Clinical Utility of Serologic Testing for Celiac Disease in Ontario Presented to the Ontario Health Technology Advisory Committee in April and October, 2010 December 2010 Background
Gliadin antibody detection in gluten
 The Ulster Medical Journal, Volume 55, No. 2, pp. 160-164, October 1986. Gliadin antibody detection in gluten enteropathy R G P Watson, S A McMillan, Clare Dolan, Cliona O'Farrelly, R J G Cuthbert, Margaret
The Ulster Medical Journal, Volume 55, No. 2, pp. 160-164, October 1986. Gliadin antibody detection in gluten enteropathy R G P Watson, S A McMillan, Clare Dolan, Cliona O'Farrelly, R J G Cuthbert, Margaret
Celiac Disease and Malabsorption
 Biomedical Sciences 23 February 2015 Celiac Disease and Malabsorption Christoph Mueller Institute of Pathology christoph.mueller@pathology.unibe.ch Malabsorption Definition Malabsorption represents the
Biomedical Sciences 23 February 2015 Celiac Disease and Malabsorption Christoph Mueller Institute of Pathology christoph.mueller@pathology.unibe.ch Malabsorption Definition Malabsorption represents the
Gluten sensitivity in Multiple Sclerosis Experimental myth or clinical truth?
 Gluten sensitivity in Multiple Sclerosis Experimental myth or clinical truth? Annals of the New York Academy of Sciences, Vol 1173, Issue 1, page 44, Issue published online 3 Sep 2009. Dana Ben-Ami Shor,
Gluten sensitivity in Multiple Sclerosis Experimental myth or clinical truth? Annals of the New York Academy of Sciences, Vol 1173, Issue 1, page 44, Issue published online 3 Sep 2009. Dana Ben-Ami Shor,
Organic - functional. Opposing views. Simple investigation of GI disorders. The dollar questions. Immune homeostasis of mucosa
 Mucosal immunology and immunopathology (IBD, CD & NCGS) Ass. Prof. Knut E. A. Lundin, MD, PhD Endoscopy Unit, Dept of Transplantation medicine Centre for Immune Regulation www.med.uio.no/cir/english Oslo
Mucosal immunology and immunopathology (IBD, CD & NCGS) Ass. Prof. Knut E. A. Lundin, MD, PhD Endoscopy Unit, Dept of Transplantation medicine Centre for Immune Regulation www.med.uio.no/cir/english Oslo
GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE AND PRESCRIPTION OF LOW LACTOSE INFANT FORMULA.
 GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE AND PRESCRIPTION OF LOW LACTOSE INFANT FORMULA. These are the lactose intolerance guidelines and it is recommended that they are used in
GUIDANCE ON THE DIAGNOSIS AND MANAGEMENT OF LACTOSE INTOLERANCE AND PRESCRIPTION OF LOW LACTOSE INFANT FORMULA. These are the lactose intolerance guidelines and it is recommended that they are used in
Celiac Disease For Dummies By Sheila Crowe, Ian Blumer READ ONLINE
 Celiac Disease For Dummies By Sheila Crowe, Ian Blumer READ ONLINE Celiac disease definition, a hereditary digestive disorder involving intolerance to gluten, usually occurring in young children, characterized
Celiac Disease For Dummies By Sheila Crowe, Ian Blumer READ ONLINE Celiac disease definition, a hereditary digestive disorder involving intolerance to gluten, usually occurring in young children, characterized
A young woman with fatigue
 IM BOARD REVIEW CME CREDIT KATHRYN A. TENG, MD Department of General Internal Medicine, Cleveland Clinic JAMES K. STOLLER, MD, EDITOR A SELF-TEST ON A CLINICAL CASE A young woman with fatigue A 22-YEAR-OLD
IM BOARD REVIEW CME CREDIT KATHRYN A. TENG, MD Department of General Internal Medicine, Cleveland Clinic JAMES K. STOLLER, MD, EDITOR A SELF-TEST ON A CLINICAL CASE A young woman with fatigue A 22-YEAR-OLD
Pediatric Food Allergies: Physician and Parent. Robert Anderson MD Rachel Anderson Syracuse, NY March 3, 2018
 Pediatric Food Allergies: Physician and Parent Robert Anderson MD Rachel Anderson Syracuse, NY March 3, 2018 Learning Objectives Identify risk factors for food allergies Identify clinical manifestations
Pediatric Food Allergies: Physician and Parent Robert Anderson MD Rachel Anderson Syracuse, NY March 3, 2018 Learning Objectives Identify risk factors for food allergies Identify clinical manifestations
The first and only fully-automated, random access, multiplex solution for Celiac IgA and Celiac IgG autoantibody testing.
 Bio-Rad Laboratories BIOPLEX 2200 SYSTEM BioPlex 2200 Celiac IgA and IgG Kits The first and only fully-automated, random access, multiplex solution for Celiac IgA and Celiac IgG autoantibody testing. The
Bio-Rad Laboratories BIOPLEX 2200 SYSTEM BioPlex 2200 Celiac IgA and IgG Kits The first and only fully-automated, random access, multiplex solution for Celiac IgA and Celiac IgG autoantibody testing. The
Living with Coeliac Disease Information & Support is key
 Living with Coeliac Disease Information & Support is key Mary Twohig Chairperson Coeliac Society of Ireland What is Coeliac Disease? LIVING WITH COELIAC DISEASE Fact Not Fad Auto immune disease - the body
Living with Coeliac Disease Information & Support is key Mary Twohig Chairperson Coeliac Society of Ireland What is Coeliac Disease? LIVING WITH COELIAC DISEASE Fact Not Fad Auto immune disease - the body
Health Canada s Position on Gluten-Free Claims
 June 2012 Bureau of Chemical Safety, Food Directorate, Health Products and Food Branch 0 Table of Contents Background... 2 Regulatory Requirements for Gluten-Free Foods... 2 Recent advances in the knowledge
June 2012 Bureau of Chemical Safety, Food Directorate, Health Products and Food Branch 0 Table of Contents Background... 2 Regulatory Requirements for Gluten-Free Foods... 2 Recent advances in the knowledge
Dermatitis Herpetiformis
 Dermatitis Herpetiformis Celiac Support Group Marshfield Clinic September 21, 2009 Jacob M. Kusmak, M.D., Pharm.D. Dermatology Resident Physician Marshfield Clinic Disclosure: I have no relevant financial
Dermatitis Herpetiformis Celiac Support Group Marshfield Clinic September 21, 2009 Jacob M. Kusmak, M.D., Pharm.D. Dermatology Resident Physician Marshfield Clinic Disclosure: I have no relevant financial
Seriously, CELIAC. talk.
 Seriously, Celiac Disease. talk. If you have celiac disease, your family members might have it too. Talk to them about your experience and how celiac disease runs in families. Tell them the facts. Urge
Seriously, Celiac Disease. talk. If you have celiac disease, your family members might have it too. Talk to them about your experience and how celiac disease runs in families. Tell them the facts. Urge
The immunology of gluten sensitivity: beyond the gut
 Opinion TRENDS in Immunology Vol.25 No.11 November 2004 The immunology of gluten sensitivity: beyond the gut Marios Hadjivassiliou 1, Clare A. Williamson 2 and Nicola Woodroofe 2 1 Department of Neurology,
Opinion TRENDS in Immunology Vol.25 No.11 November 2004 The immunology of gluten sensitivity: beyond the gut Marios Hadjivassiliou 1, Clare A. Williamson 2 and Nicola Woodroofe 2 1 Department of Neurology,
Functional Medicine Is the application of alternative holistic measures to show people how to reverse thyroid conditions, endocrine issues, hormone
 Functional Medicine Is the application of alternative holistic measures to show people how to reverse thyroid conditions, endocrine issues, hormone issues, fibromyalgia, autoimmunity diseases and the like.
Functional Medicine Is the application of alternative holistic measures to show people how to reverse thyroid conditions, endocrine issues, hormone issues, fibromyalgia, autoimmunity diseases and the like.
The first and only fully-automated, random access, multiplex solution for Celiac IgA and Celiac IgG autoantibody testing.
 Bio-Rad Laboratories bioplex 2200 SYSTEM BioPlex 2200 Celiac IgA and IgG Kits * The first and only fully-automated, random access, multiplex solution for Celiac IgA and Celiac IgG autoantibody testing.
Bio-Rad Laboratories bioplex 2200 SYSTEM BioPlex 2200 Celiac IgA and IgG Kits * The first and only fully-automated, random access, multiplex solution for Celiac IgA and Celiac IgG autoantibody testing.
Vaccination for Celiac Disease: utopia or concrete hope for Celiac Disease recovery
 Vaccination for Celiac Disease: utopia or concrete hope for Celiac Disease recovery January 31, 2012 ImmusanT, Inc One Broadway, 14th Floor Cambridge, MA 02142 Key Points Objective: Treatment of celiac
Vaccination for Celiac Disease: utopia or concrete hope for Celiac Disease recovery January 31, 2012 ImmusanT, Inc One Broadway, 14th Floor Cambridge, MA 02142 Key Points Objective: Treatment of celiac
Celiac Disease: A Holistic Review
 Celiac Disease: A Holistic Review Ryan Seals B.S. (Bachelor of Science) Celiac disease is a condition characterized by an abnormality of the small intestine caused by the consumption of gluten in the diet.
Celiac Disease: A Holistic Review Ryan Seals B.S. (Bachelor of Science) Celiac disease is a condition characterized by an abnormality of the small intestine caused by the consumption of gluten in the diet.
Insight into the genetics and immunologic mechanisms CLINICAL GENOMICS. Celiac Disease Genetics: Current Concepts and Practical Applications
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:843 851 CLINICAL GENOMICS Celiac Disease Genetics: Current Concepts and Practical Applications LUDVIG M. SOLLID and BENEDICTE A. LIE Institute of Immunology,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:843 851 CLINICAL GENOMICS Celiac Disease Genetics: Current Concepts and Practical Applications LUDVIG M. SOLLID and BENEDICTE A. LIE Institute of Immunology,
Innate and adaptive immunity: the Yin and Yang of celiac disease
 Bana Jabri Donald D. Kasarda Peter H. R. Green Innate and adaptive immunity: the Yin and Yang of celiac disease Authors addresses Bana Jabri 1, Donald D. Kasarda 2, Peter H. R. Green 3 1 Department of
Bana Jabri Donald D. Kasarda Peter H. R. Green Innate and adaptive immunity: the Yin and Yang of celiac disease Authors addresses Bana Jabri 1, Donald D. Kasarda 2, Peter H. R. Green 3 1 Department of
L y mp h o c y t i c D i s o r d e r s of t h e. What does too many mean? Unifying theory 2/24/2011
 L y mp h o c y t i c D i s o r d e r s of t h e G a s t Robert r o M. i Genta n t e s t i Caris n alife l Sciences, T rirving, a ctexas t Dallas VAMC UT Southwestern Dallas, Texas Esophagus Stomach Small
L y mp h o c y t i c D i s o r d e r s of t h e G a s t Robert r o M. i Genta n t e s t i Caris n alife l Sciences, T rirving, a ctexas t Dallas VAMC UT Southwestern Dallas, Texas Esophagus Stomach Small
Follow-up Management of Patients with Celiac Disease: Resource for Health Professionals
 Follow-up Management of Patients with Celiac Disease: Resource for Health Professionals Jocelyn Silvester, MD PhD FRCPC April 27, 2017 Research grants Disclosures Canadian Institutes of Health Research
Follow-up Management of Patients with Celiac Disease: Resource for Health Professionals Jocelyn Silvester, MD PhD FRCPC April 27, 2017 Research grants Disclosures Canadian Institutes of Health Research
Clinical updates on diagnosing glutensensitive enteropathy
 Editorial Acta Medica Academica 2011;40(2):105-109 DOI 10.5644/ama2006-124.13 Clinical updates on diagnosing glutensensitive enteropathy Faruk Hadziselimovic 1, 2, Annemarie Bürgin-Wolff 1 1 Institute
Editorial Acta Medica Academica 2011;40(2):105-109 DOI 10.5644/ama2006-124.13 Clinical updates on diagnosing glutensensitive enteropathy Faruk Hadziselimovic 1, 2, Annemarie Bürgin-Wolff 1 1 Institute
Matt McCollough, MD Fellow, GI/Hep University of Louisville March 19, 2009
 Matt McCollough, MD Fellow, GI/Hep University of Louisville March 19, 2009 Define Celiac Disease Recognize the epidemiology Understand basic pathophysiology Be able to employ a diagnostic approach Review
Matt McCollough, MD Fellow, GI/Hep University of Louisville March 19, 2009 Define Celiac Disease Recognize the epidemiology Understand basic pathophysiology Be able to employ a diagnostic approach Review
New York, New York 10032; 2 Department of Pathology, Medicine and Pediatrics, University of Chicago, Chicago,
 I 5 Sep 2005 17:27 AR ANRV262-ME57-14.tex XMLPublish SM P1: OKZ /POI P2: (Some corrections may occur before final publication online and in print) R E V I E W S N A D V A N E C Annu. Rev. Med. 2006. 57:14.1
I 5 Sep 2005 17:27 AR ANRV262-ME57-14.tex XMLPublish SM P1: OKZ /POI P2: (Some corrections may occur before final publication online and in print) R E V I E W S N A D V A N E C Annu. Rev. Med. 2006. 57:14.1
History of Food Allergies
 Grand Valley State University From the SelectedWorks of Jody L Vogelzang PhD, RDN, FAND, CHES Spring 2013 History of Food Allergies Jody L Vogelzang, PhD, RDN, FAND, CHES, Grand Valley State University
Grand Valley State University From the SelectedWorks of Jody L Vogelzang PhD, RDN, FAND, CHES Spring 2013 History of Food Allergies Jody L Vogelzang, PhD, RDN, FAND, CHES, Grand Valley State University
Food Allergies on the Rise in American Children
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/hot-topics-in-allergy/food-allergies-on-the-rise-in-americanchildren/3832/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/hot-topics-in-allergy/food-allergies-on-the-rise-in-americanchildren/3832/
Utility in Clinical Practice of Immunoglobulin A Anti-Tissue Transglutaminase Antibody for the Diagnosis of Celiac Disease
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:726 730 Utility in Clinical Practice of Immunoglobulin A Anti-Tissue Transglutaminase Antibody for the Diagnosis of Celiac Disease JULIAN A. ABRAMS,* PARDEEP
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:726 730 Utility in Clinical Practice of Immunoglobulin A Anti-Tissue Transglutaminase Antibody for the Diagnosis of Celiac Disease JULIAN A. ABRAMS,* PARDEEP
Frontiers in Food Allergy and Allergen Risk Assessment and Management. 19 April 2018, Madrid
 Frontiers in Food Allergy and Allergen Risk Assessment and Management 19 April 2018, Madrid Food allergy is becoming one of the serious problems of China's food safety and public health emergency. 7 Number
Frontiers in Food Allergy and Allergen Risk Assessment and Management 19 April 2018, Madrid Food allergy is becoming one of the serious problems of China's food safety and public health emergency. 7 Number
